Initial Workup - Code Red, Brain Bleed
- ABCs first: Secure airway, breathing, circulation.
- Immediate non-contrast CT head: The single most important initial test.
- Vitals & Neuro Exam: Glasgow Coma Scale (GCS), NIH Stroke Scale (NIHSS).
- Key Labs: Stat coagulation panel (PT/INR, aPTT), CBC, platelets, glucose.
- Blood Pressure: Keep SBP <160 mmHg initially; use IV labetalol or nicardipine.
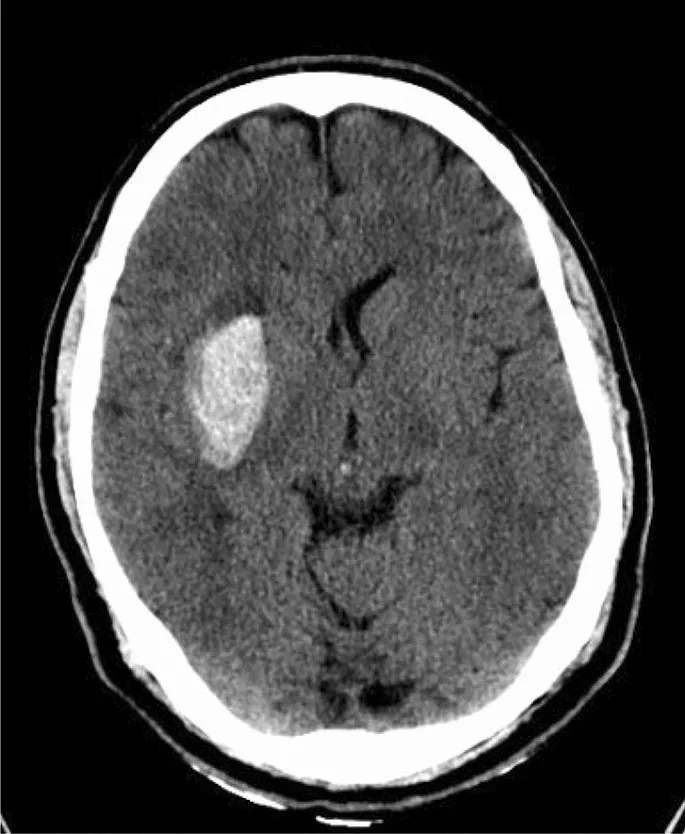
⭐ Non-contrast CT is paramount. Thrombolytics (for ischemic stroke) are absolutely contraindicated in hemorrhagic stroke and would be catastrophic.
Acute BP & Coags - The First Hour
-
Immediate Goal: Aggressively lower BP and reverse any coagulopathy to limit hematoma expansion, the primary driver of early neurological deterioration.
-
Blood Pressure Control:
- Target Systolic BP <140 mmHg.
- Use easily titratable IV agents like Labetalol or Nicardipine.
-
Coagulopathy Reversal:
- Warfarin: Vitamin K + 4-factor Prothrombin Complex Concentrate (4F-PCC).
- DOACs: Use specific reversal agents (Idarucizumab for Dabigatran; Andexanet Alfa for Xa inhibitors).
- Antiplatelets: Platelet transfusions are generally not recommended but may be considered for patients requiring neurosurgery.
⭐ For warfarin reversal, 4F-PCC is superior to FFP. It provides faster INR correction with a lower infusion volume, minimizing the risk of fluid overload.
ICH vs. SAH - Two Flavors of Trouble
-
Intracerebral Hemorrhage (ICH)
- Cause: Chronic hypertension → Charcot-Bouchard microaneurysms; cerebral amyloid angiopathy.
- Presentation: Focal neurological deficits that worsen over minutes to hours.
- CT Finding: Blood within the brain parenchyma.
- Management: Strict BP control (target SBP <140 mmHg), reverse anticoagulation.
-
Subarachnoid Hemorrhage (SAH)
- Cause: Ruptured saccular (berry) aneurysm (85%).
- Presentation: Sudden, explosive "worst headache of my life"; meningeal signs.
- CT Finding: Blood in cisterns and sulci.
- Management: Nimodipine for vasospasm prevention; surgical clipping or endovascular coiling.
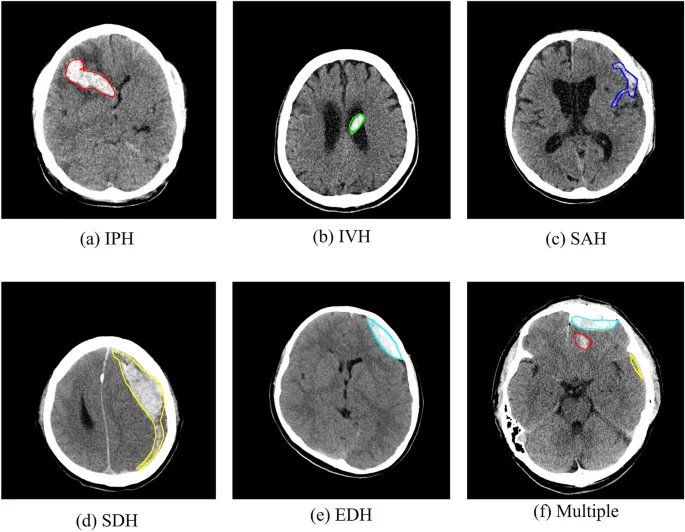
⭐ Nimodipine in SAH does not prevent re-bleeding but is critical to prevent delayed cerebral ischemia from vasospasm, a major cause of morbidity/mortality days after the initial event.
Complications - Watching for Waves
- Re-bleeding: Highest risk in first 24h; sudden neurological decline, ↑ mortality.
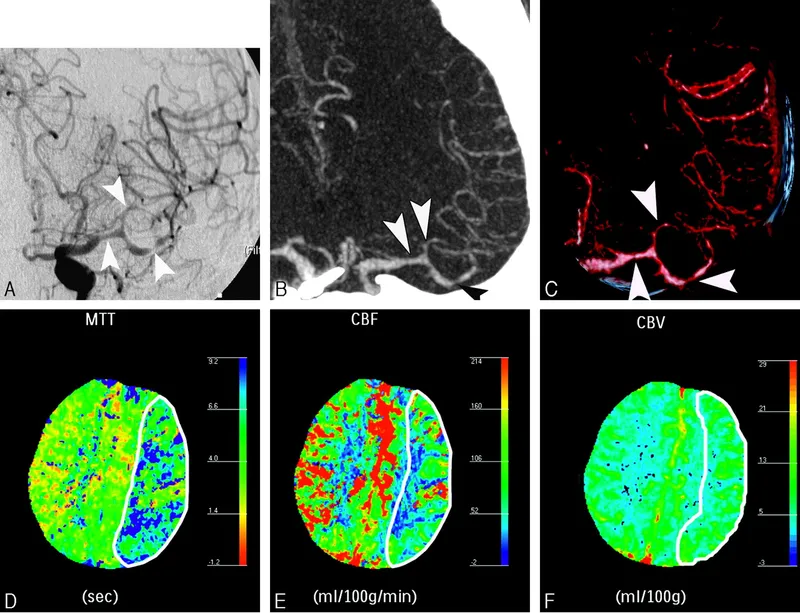
- Vasospasm: Peaks 4-14 days post-SAH. Causes delayed cerebral ischemia. Prevent with nimodipine.
- Hydrocephalus: Obstructive/communicating due to blood in ventricles/cisterns. May require external ventricular drain (EVD).
- Seizures: Can occur due to cortical irritation from blood. Prophylaxis is controversial.
- Hyponatremia: From SIADH or cerebral salt wasting.
⭐ Nimodipine is the only drug shown to improve outcomes in SAH by preventing vasospasm-related ischemia, but it does not reduce the incidence of vasospasm itself.
High-Yield Points - ⚡ Biggest Takeaways
- Immediate BP control is the first crucial step; aggressively lower to SBP < 140 mmHg.
- Urgently reverse any anticoagulation; use Vitamin K, FFP, or prothrombin complex concentrates (PCC).
- Secure emergent neurosurgical consultation for potential hematoma evacuation.
- Manage elevated intracranial pressure (ICP) with head elevation, mannitol, and hyperventilation.
- Seizure prophylaxis is often indicated, particularly for lobar hemorrhages.
- Non-contrast CT is the essential first diagnostic step to differentiate from ischemic stroke.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

