Initial Assessment - Time is Brain!
- Priority #1: Stabilize patient (ABCs), establish IV access, and get vital signs.
- ASAP Actions:
- Finger-stick glucose to rule out hypoglycemia (a key stroke mimic).
- Focused history: Pinpoint "Last Known Well" (LKW) time.
- Baseline neurologic exam using the NIH Stroke Scale (NIHSS).
- Crucial Diagnostic: Immediate non-contrast head CT to differentiate ischemic vs. hemorrhagic stroke. This dictates all subsequent therapy.
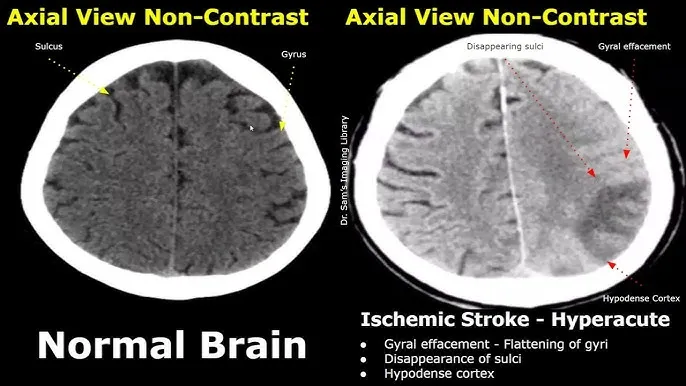
⭐ The single most important initial imaging study for a suspected stroke patient is a non-contrast head CT to rule out intracranial hemorrhage before considering thrombolysis.
IV Thrombolysis - Clot Buster Crew
- Drug: Alteplase (tPA), a recombinant tissue plasminogen activator.
- Mechanism: Converts plasminogen to plasmin → degrades fibrin clot.
- Time Window: Crucial! Administer within 3 to 4.5 hours of "last known well" time.
Key Criteria:
- Inclusion: Disabling ischemic stroke, age >18.
- Exclusion (Common):
- BP > 185/110 mmHg (refractory to treatment).
- Active bleed, recent major surgery/trauma (<3 months).
- Platelets <100,000, INR >1.7.
- History of intracranial hemorrhage.
⭐ Blood pressure control is critical. BP must be < 185/110 mmHg before starting and maintained < 180/105 mmHg for 24h after infusion. Use IV Labetalol or Nicardipine.
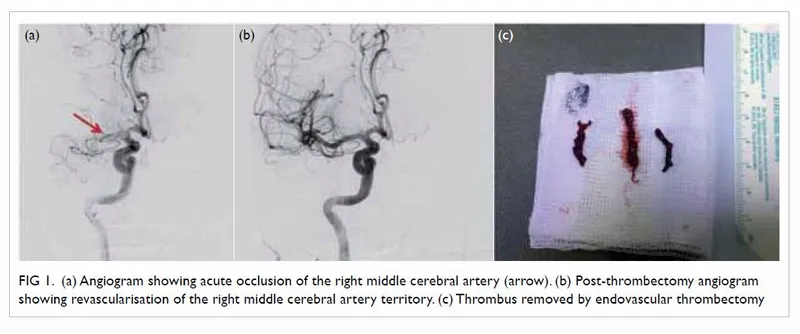
Endovascular Therapy - The Clot Claw
- Indication: Mechanical thrombectomy for Large Vessel Occlusion (LVO) in the anterior circulation (e.g., ICA, MCA-M1).
- Time Window:
- Standard: Within 6 hours of symptom onset.
- Extended: Up to 24 hours if DAWN or DEFUSE-3 trial criteria are met.
- Core Criteria:
- Pre-stroke mRS 0-1.
- NIHSS ≥ 6.
- Alberta Stroke Program Early CT Score (ASPECTS) ≥ 6.
⭐ The key to the extended 6-24 hour window is imaging-based selection. A significant mismatch between a small, irreversible infarct core and a large, salvageable penumbra on CT perfusion or MRI justifies intervention.
Supportive Care - Pressure & Prevention
- Blood Pressure Control: Crucial to balance perfusion & hemorrhage risk.
-
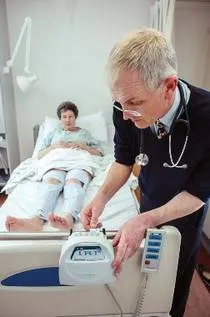
DVT Prophylaxis:
- Start intermittent pneumatic compression (IPC) devices immediately.
- Delay subcutaneous heparin/LMWH for 24h post-thrombolysis.
-
Aspiration Prevention:
- Keep patient NPO (nil per os) initially.
- Perform a formal swallow screen before allowing any oral intake.
⭐ Permissive Hypertension: In patients not receiving thrombolysis, higher blood pressure is tolerated to maintain cerebral perfusion to the ischemic penumbra. Aggressively lowering BP can worsen the stroke.
High‑Yield Points - ⚡ Biggest Takeaways
- Time is brain: A non-contrast CT is crucial to rule out hemorrhage before any intervention.
- IV alteplase (tPA) is the standard of care if administered within 3 to 4.5 hours of symptom onset, assuming no contraindications.
- Mechanical thrombectomy is indicated for large vessel occlusions (LVO) with a treatment window of up to 24 hours.
- Blood pressure must be <185/110 mmHg before tPA. Otherwise, permissive hypertension is generally allowed.
- Initiate aspirin within 24-48 hours, but delay for 24 hours if the patient received tPA.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

