Common Sources - The Usual Suspects
📌 Mnemonic: LUCAS → Lungs, Urine, Catheters, Abdomen, Skin.
- Lungs (~50%):
- Pneumonia, empyema.
- Action: Chest X-ray, sputum culture.
- Intra-abdominal (~20%):
- Peritonitis, cholangitis, abscess.
- Action: CT Abdomen/Pelvis.
- Urinary Tract (~15%):
- UTI/Pyelonephritis, often catheter-related.
- Action: Urinalysis, urine culture.
- Catheter-Related (CRBSI):
- Central or peripheral lines.
- Action: Paired blood cultures (line + peripheral).
- Skin/Soft Tissue:
- Cellulitis, fasciitis, infected ulcers.
⭐ Occult abscesses (e.g., intra-abdominal, pelvic) are a classic cause of persistent fever and non-resolving sepsis despite appropriate antibiotic therapy.
Diagnostic Imaging - Seeing the Source
- Goal: Rapidly confirm & localize suspected infection to guide source control.
- Chest X-ray (CXR): First-line for suspected pneumonia. Look for infiltrates, consolidation. Portable CXR is key for unstable patients.
- CT Scan (IV contrast): Gold standard for deep-seated infections.
- Abdomen/Pelvis: Abscesses, collections, pyelonephritis.
- Soft Tissue: Necrotizing fasciitis (look for gas).
- Ultrasound (US): Rapid, bedside assessment.
- RUSH exam: Screens for effusions, hydronephrosis.
- Excellent for cholecystitis, DVT, and guiding procedures.
- Echocardiogram (TTE/TEE): Essential for suspected infective endocarditis to visualize vegetations.
⭐ A CT scan with IV contrast is the diagnostic test of choice for most suspected deep space infections or intra-abdominal abscesses, providing a roadmap for intervention.
Labs & Cultures - The Bug Hunt
-
Core Blood Work:
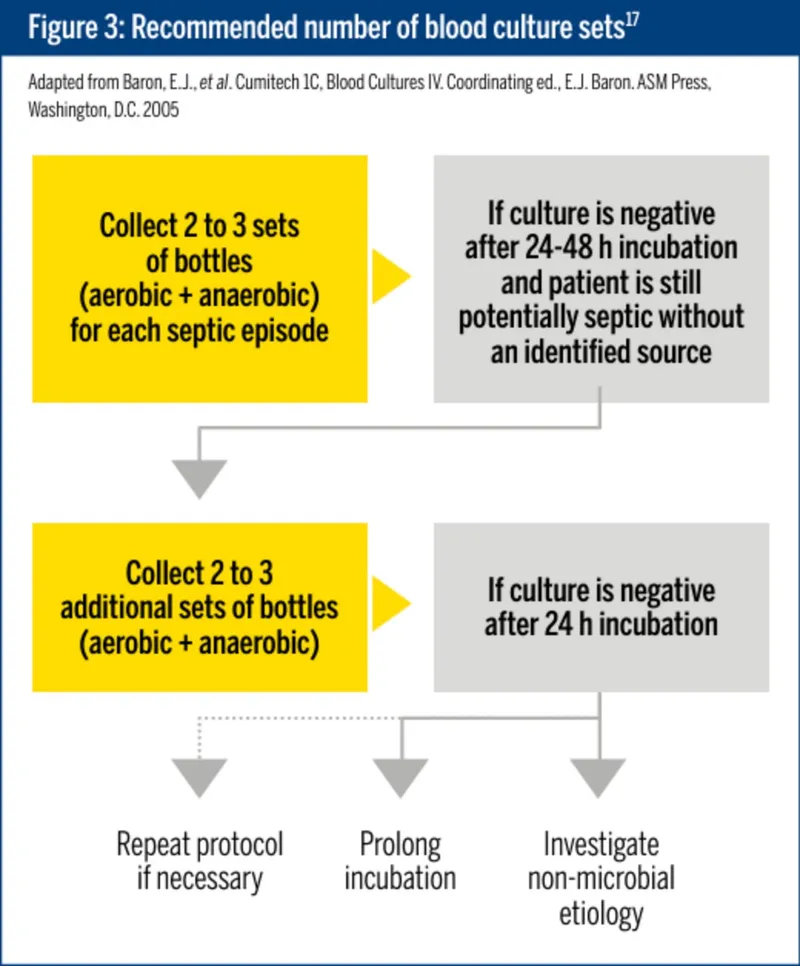
- Blood Cultures: 2 sets from different venipuncture sites, drawn before starting antibiotics. Use aerobic & anaerobic bottles.
- Lactate: Key diagnostic and prognostic marker. Re-measure if initial is > 2 mmol/L to guide resuscitation.
- CBC with differential: Look for leukocytosis (WBC > 12,000), leukopenia (WBC < 4,000), or >10% bands (left shift).
- CMP: Assesses for end-organ damage (e.g., ↑ creatinine, ↑ LFTs).
- Coagulation studies: PT, PTT, INR, fibrinogen to screen for DIC.
-
Targeted Investigations:
- Source-specific cultures: Urine, sputum, wound, or CSF based on clinical suspicion.
⭐ Procalcitonin (PCT) rises more rapidly and is more specific for bacterial sepsis than C-reactive protein (CRP). It's a key biomarker for guiding antibiotic therapy duration.
Source Control - The Fix-It Plan
- Goal: Eradicate the source of infection. Intervene as soon as sepsis is identified and initial resuscitation is underway, ideally within 6-12 hours.
- Core Principles (The "4 D's"):
- Drainage: Purulent collections (e.g., abscess, empyema).
- Debridement: Infected, necrotic tissue (e.g., necrotizing fasciitis).
- Device Removal: Infected lines, catheters, or prosthetics.
- Definitive Management: Correcting anatomical derangements to stop ongoing contamination (e.g., bowel perforation repair).
⭐ High-Yield: For severe intra-abdominal infections, definitive source control is critical. Delays beyond 12 hours are associated with significantly increased mortality. This often requires emergent surgical or percutaneous procedures.
High‑Yield Points - ⚡ Biggest Takeaways
- Promptly identify and control the source of infection, ideally within 6-12 hours of presentation.
- Early imaging (e.g., CT abdomen/pelvis) is crucial for diagnosing occult intra-abdominal or deep space infections.
- The most common sources are lungs, abdomen, urinary tract, and skin/soft tissue.
- Remove infected intravascular catheters and other devices after establishing alternative access.
- Urgent surgical or percutaneous drainage is critical for abscesses, empyema, or obstructive cholangitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

