Hemodynamic Support - Shock & Awe Resuscitation
- Initial Fluid Resuscitation:
- Rapid infusion of 30 mL/kg isotonic crystalloid within the first 3 hours. Reassess fluid responsiveness dynamically.
- Vasopressor Therapy (if hypotensive during/after fluids):
- Target Mean Arterial Pressure (MAP): ≥65 mmHg.
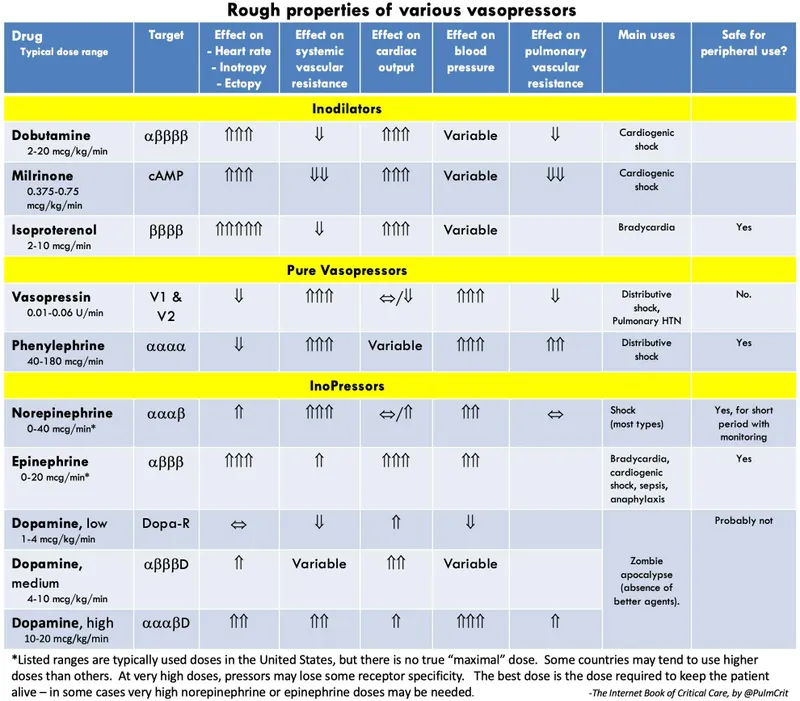
- First-line: Norepinephrine (potent α-1, modest β-1 agonist).
- Second-line: Add Vasopressin (V1 agonist) to decrease norepinephrine needs, or Epinephrine.
- 📌 "No-Va-E": Norepinephrine → Vasopressin → Epinephrine.
- Inotropic Support:
- Add Dobutamine for persistent hypoperfusion or signs of myocardial dysfunction (e.g., ↑ cardiac filling pressures, ↓ cardiac output) despite adequate volume and MAP.
⭐ The arterial catheter for continuous blood pressure monitoring should be placed as soon as practical in patients requiring vasopressors. This provides more accurate MAP readings than cuff measurements.
Respiratory Failure - Lungs Under Pressure
-
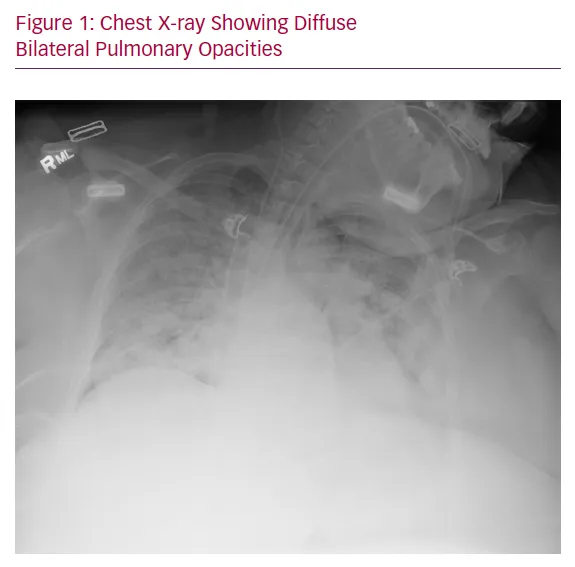
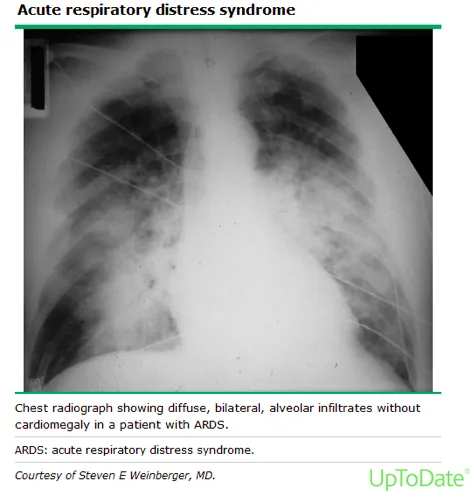
ARDS: Sepsis-induced hypoxemia ($PaO₂/FiO₂ \le 300$) with bilateral infiltrates on CXR. A major cause of mortality.
-
Core Strategy: Lung-Protective Ventilation (LPV)
- Low Tidal Volume (LTV): 6 mL/kg (predicted body weight).
- Plateau Pressure (Pplat): Keep < 30 cm H₂O.
- PEEP: Use to recruit alveoli and improve oxygenation.
- Permissive Hypercapnia: Tolerate ↑PaCO₂ to minimize ventilator-induced lung injury (VILI).
-
Adjunctive Therapies:
- Prone Positioning: For moderate-to-severe ARDS ($PaO₂/FiO₂ < 150$).
- Conservative Fluids: After initial resuscitation, diurese to a neutral/negative balance.
⭐ Low tidal volume ventilation is the cornerstone of ARDS management and is proven to decrease mortality.
Renal & Metabolic - Kidney & Sugar Crisis
-
Acute Kidney Injury (AKI):
- Monitor urine output (goal > 0.5 mL/kg/hr) & creatinine.
- Ensure adequate fluid resuscitation to maintain renal perfusion.
- Consider Renal Replacement Therapy (RRT) for anuria, severe metabolic acidosis, or refractory hyperkalemia.
-
Glycemic Control:
- Target blood glucose 140-180 mg/dL using an insulin infusion.
- Monitor frequently to prevent iatrogenic hypoglycemia.
⭐ In septic patients, tight glycemic control (<110 mg/dL) is associated with increased mortality due to hypoglycemia risk.
Systemic Support - Collateral Damage Control
- Lung Protective Ventilation (ARDS): Low tidal volume ($4-6$ mL/kg ideal body weight), plateau pressure <30 cm H₂O. Use PEEP.
- Glycemic Control: Target glucose <180 mg/dL with insulin infusion. Avoid hypoglycemia.
- VTE Prophylaxis: LMWH/unfractionated heparin. Use mechanical if bleeding risk is high.
- Stress Ulcer Prophylaxis: PPI/H2 blockers for major bleeding risk factors (coagulopathy, mechanical ventilation >48h).
- Nutrition: Early enteral feeding is preferred.
- Corticosteroids: Consider IV hydrocortisone for refractory shock unresponsive to fluids/vasopressors.
⭐ In septic ARDS, low tidal volume ventilation is the only intervention proven to reduce mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Aggressive fluid resuscitation is the initial cornerstone, but judicious use is key to prevent volume overload.
- Norepinephrine is the first-line vasopressor to maintain a Mean Arterial Pressure (MAP) ≥65 mmHg.
- Add vasopressin or epinephrine as second-line agents for persistent hypotension despite adequate fluids and norepinephrine.
- Consider IV hydrocortisone for patients in refractory septic shock.
- Provide organ support: mechanical ventilation for ARDS and renal replacement therapy for acute kidney injury.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

