Sepsis Recognition - Spotting the Enemy

- Sepsis: Life-threatening organ dysfunction from a dysregulated host response to infection.
- Screening Tool (Bedside): quick SOFA (qSOFA) score identifies high-risk patients outside the ICU. Suspect sepsis if score is $≥ extbf{2}$.
- Hypotension: Systolic BP ≤ 100 mmHg
- Altered Mental Status: Glasgow Coma Scale < 15
- Tachypnea: Respiratory Rate ≥ 22/min
- 📌 Mnemonic: HAT
⭐ Lactate > 2 mmol/L indicates tissue hypoperfusion and is a critical marker, even if blood pressure is normal. It prompts immediate resuscitation.
- Systemic Inflammatory Response Syndrome (SIRS): Broader criteria, less specific for sepsis. Requires ≥2 of:
- Temp > 38°C or < 36°C
- HR > 90
- RR > 20 or PaCO₂ < 32
- WBC > 12,000 or < 4,000
Hour-1 Bundle - Race Against Time
Immediate, coordinated actions within the first hour of recognizing sepsis or septic shock. The goal is to stabilize the patient and prevent progression to multi-organ failure.
- Measure Lactate: Re-measure if initial lactate is elevated (> 2 mmol/L).
- Obtain Blood Cultures: Crucial before starting antibiotics, but must not delay therapy.
- Administer Broad-Spectrum Antibiotics: Administer within 1 hour of recognition.
- Rapid Fluid Resuscitation: Begin 30 mL/kg IV crystalloid for hypotension or lactate ≥ 4 mmol/L.
- Apply Vasopressors: If hypotensive during or after fluid challenge, to maintain Mean Arterial Pressure (MAP) ≥ 65 mmHg. Norepinephrine is the first-line agent.
⭐ For septic shock patients, every hour of delay in administering effective antibiotics is associated with a measurable increase in mortality.
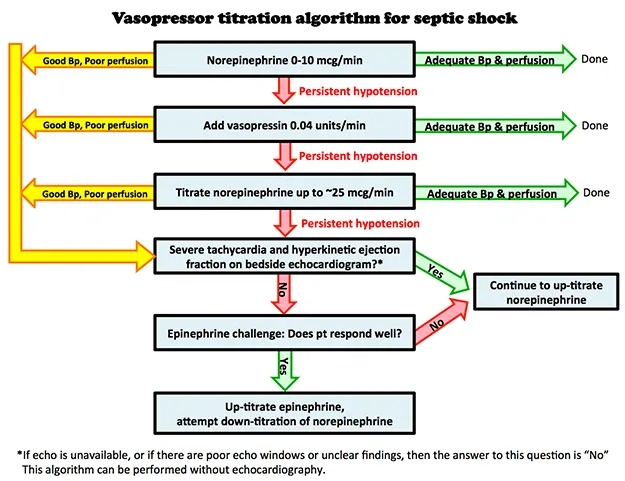
Refractory Shock - When Fluids Fail
Persistent hypotension despite adequate fluid resuscitation (30 mL/kg crystalloid) necessitates vasopressors to maintain Mean Arterial Pressure (MAP) ≥ 65 mmHg.
- Norepinephrine: First-line. Potent α1 & moderate β1 agonist.
- Vasopressin: Add-on therapy, not titrated. Acts on V1 receptors, often sparing catecholamine requirements.
- Epinephrine: For refractory shock despite initial pressors. Potent α & β effects.
- Dobutamine: Consider for myocardial dysfunction (↑CI, ScvO2) once MAP is stable.
⭐ For patients on high-dose catecholamines, consider IV hydrocortisone (200 mg/day). This is thought to reverse acquired adrenal insufficiency in severe stress states.
Monitoring & Goals - Are We Winning?
- CVP: 8-12 mmHg
- MAP: ≥ 65 mmHg
- Urine Output: > 0.5 $mL/kg/hr$
- ScvO₂ (Central Venous O₂ Sat): ≥ 70%
- Lactate Clearance: Trend towards normalization, indicating improved tissue perfusion.
⭐ Lactate clearance is a key marker of resuscitation success, reflecting improved tissue perfusion, and should be monitored alongside hemodynamic parameters.
High‑Yield Points - ⚡ Biggest Takeaways
- Initial resuscitation: rapid 30 mL/kg isotonic crystalloid infusion within the first 3 hours.
- Persistent hypotension despite fluids requires vasopressors; norepinephrine is first-line.
- The primary hemodynamic target is a Mean Arterial Pressure (MAP) ≥ 65 mmHg.
- Measure lactate initially and serially to guide resuscitation; a ↓ lactate indicates improved perfusion.
- Obtain blood cultures before administering broad-spectrum antibiotics, but do not delay antibiotics beyond 1 hour.
- Crucially, identify and address the source of infection early.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

