Sepsis Definitions - The Body's Overreaction
-
Sepsis: Life-threatening organ dysfunction caused by a dysregulated host response to infection. Diagnosed via suspected infection plus an acute increase in SOFA score of ≥2 points.
-
Septic Shock: A subset of sepsis with critical circulatory and metabolic abnormalities.
- Persistent hypotension requiring vasopressors to maintain MAP ≥65 mmHg.
- Serum lactate level >2 mmol/L despite adequate fluid resuscitation.
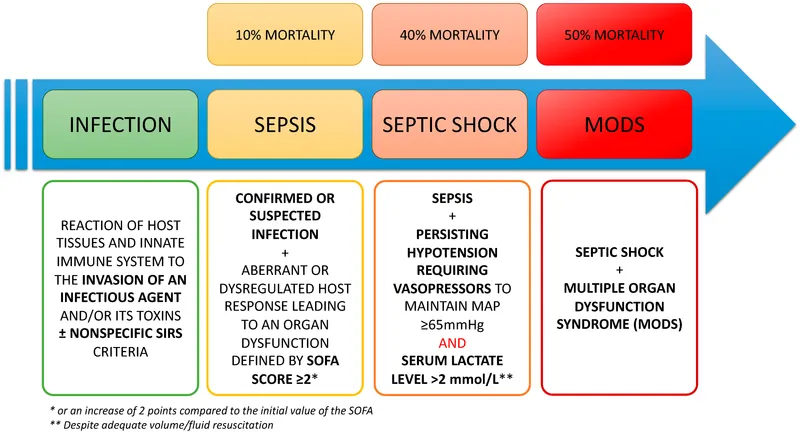
⭐ Lactate is a marker of tissue hypoperfusion; its elevation can identify high-risk patients even with normal blood pressure.
Screening Tools - Spotting Sepsis Early
- Goal: Rapidly identify patients with suspected infection who are likely to have poor outcomes. Key tools are SIRS and qSOFA for initial bedside assessment, especially in non-ICU settings.
| Criteria | SIRS (Systemic Inflammatory Response) | qSOFA (quick SOFA) |
|---|---|---|
| Use | High sensitivity, low specificity | Bedside screen for sepsis risk (non-ICU) |
| Threshold | ≥2 criteria | ≥2 criteria |
| Parameters | Temp >38°C/<36°C, HR >90, RR >20, WBC >12k/<4k | RR ≥22, GCS <15, SBP ≤100 |
- Hypotension (SBP ≤ 100 mmHg)
- Altered Mental Status (GCS < 15)
- Tachypnea (RR ≥ 22/min)
⭐ qSOFA is a risk stratification tool, not a diagnostic criterion for sepsis. It has better prognostic accuracy for in-hospital mortality than SIRS in patients outside the ICU.
- Clinical Workflow:
Organ Dysfunction - The Domino Effect
Sepsis triggers a systemic inflammatory cascade, leading to widespread endothelial damage and microvascular thrombosis, culminating in organ failure.
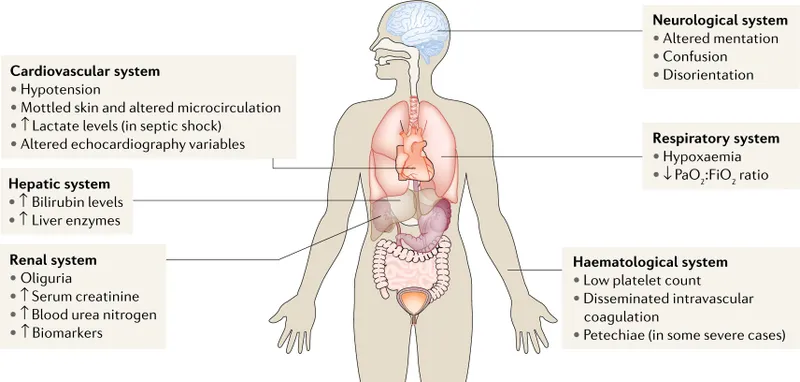
- Cardiovascular
- Hypotension (SBP < 90 mmHg, MAP < 65 mmHg)
- Tachycardia
- ↑ Serum lactate (> 2 mmol/L)
- Respiratory
- Tachypnea & increased work of breathing
- Hypoxemia (PaO2/FiO2 ratio < 300)
- Acute Respiratory Distress Syndrome (ARDS)
- Renal
- Oliguria (< 0.5 mL/kg/hr for > 2 hrs)
- ↑ Serum creatinine
- Central Nervous System (CNS)
- Altered mental status (GCS < 15)
- Delirium, confusion, or coma
- Hepatic
- ↑ Bilirubin (> 2 mg/dL)
- ↑ Transaminases (ALT/AST)
- Hematologic
- Thrombocytopenia (Platelets < 100,000/μL)
- Coagulopathy (INR > 1.5)
⭐ Lactate is not just a marker of tissue hypoxia but also contributes to cardiovascular depression and vasodilation.
Initial Workup - The First Hour
- Goal: Complete bundle within 1 hour of recognition.
- Administer 30 mL/kg crystalloid for hypotension or lactate ≥4 mmol/L.
- Start vasopressors if hypotensive during or after fluid resuscitation to maintain MAP ≥65 mmHg.
⭐ Repeat lactate measurement within 2-4 hours if the initial level is elevated (> 2 mmol/L) to guide resuscitation.
High-Yield Points - ⚡ Biggest Takeaways
- The qSOFA score (GCS < 15, RR ≥ 22, SBP ≤ 100) is a key bedside tool to identify high-risk patients.
- An elevated serum lactate (> 2 mmol/L) signifies tissue hypoperfusion, a hallmark of septic shock.
- Suspect sepsis with a known infection plus any sign of new-onset organ dysfunction.
- Draw blood cultures before giving antibiotics, but do not delay treatment.
- SIRS criteria are sensitive but not specific; use them to raise suspicion for organ failure.
- Prompt recognition is the most critical factor in reducing sepsis mortality.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

