De-escalation Kickstart - Timing is Everything
- Definition: Systematically narrowing the spectrum of antimicrobial therapy based on updated clinical and microbiological data.
- Primary Goals: Minimize antibiotic resistance, reduce drug toxicity, and lower healthcare costs.
- Crucial Window: Re-evaluate the patient and antibiotic regimen at 48-72 hours.
- Key Triggers for De-escalation:
- Clinical improvement (e.g., hemodynamic stability, ↓ fever).
- Culture and sensitivity results available.
- ↓ inflammatory markers (e.g., Procalcitonin, CRP).
⭐ A >80% decrease in procalcitonin (PCT) from its peak value is a strong indicator to consider discontinuing antibiotics, reducing duration of therapy.
The Art of the Taper - Narrowing the Net
De-escalation is a core antimicrobial stewardship principle, initiated once clinical stability is achieved and culture data is available (24-72h). The goal is to reduce antibiotic selective pressure, toxicity, and costs.
- Trigger: Review culture and sensitivity (C&S) results.
- Action: Switch from empiric broad-spectrum agents to a narrower, pathogen-specific antibiotic.
- Example: Vancomycin & Piperacillin-Tazobactam → Ceftriaxone for a sensitive E. coli bacteremia.
- Prerequisites:
- Achieved source control.
- Improving clinical markers (e.g., ↓ WBC, afebrile).
⭐ Procalcitonin (PCT) can guide de-escalation. A decrease of >80% from its peak value strongly supports stopping antibiotics, particularly in lower respiratory tract infections.
Biomarker Guidance - Procalcitonin's Role
-
Procalcitonin (PCT): A peptide precursor of calcitonin, released by parenchymal cells in response to bacterial endotoxins.
- More specific for bacterial infections than other acute-phase reactants like C-reactive protein (CRP).
- Levels correlate with infection severity and prognosis.
-
De-escalation Algorithm: PCT kinetics are a key tool to guide antibiotic discontinuation.
- Measure PCT at baseline and serially (e.g., every 24-48h).
- Strongly consider stopping antibiotics if:
- PCT level drops by >80% from its peak value.
- Absolute PCT value falls to <0.5 ng/mL.
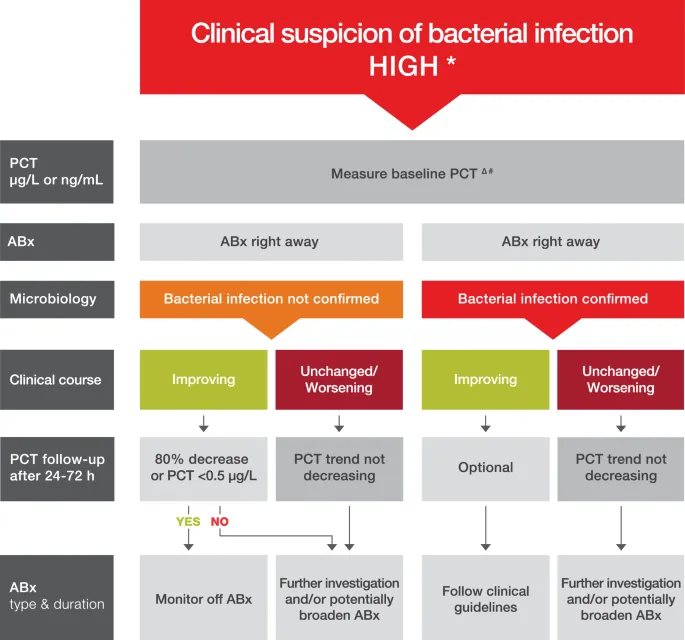
⭐ Exam Favorite: PCT-guided algorithms can significantly reduce antibiotic duration and total exposure in patients with respiratory infections and sepsis, without negatively impacting clinical outcomes like mortality or length of stay.
The Finish Line - How Long is Enough?
- Standard Duration: Most uncomplicated sepsis cases are treated for 7-10 days.
- Source Control is Key: Duration depends on successful drainage or removal of the infection source (e.g., abscess, infected line).
- Clinical Stability Markers:
- Afebrile for 48-72 hours.
- Normalizing WBC count.
- Hemodynamically stable (no vasopressors).
- Biomarker Guidance:
- Procalcitonin (PCT) can guide de-escalation.
- Consider stopping antibiotics if PCT drops by >80% from peak or to <0.5 ng/mL.
⭐ Using procalcitonin (PCT) algorithms to guide antibiotic cessation is safe and can decrease the total duration of antibiotic therapy without adversely affecting clinical outcomes.
High‑Yield Points - ⚡ Biggest Takeaways
- De-escalation is the practice of narrowing antibiotic coverage, typically after 48-72 hours, guided by culture data and clinical improvement.
- Primary goals are to combat antibiotic resistance, reduce drug toxicity, and lower healthcare costs.
- Key decision drivers include clinical stability, pathogen identification with susceptibilities, and negative cultures.
- A significant drop in procalcitonin (PCT) supports shortening antibiotic duration or de-escalating therapy.
- This involves switching from broad-spectrum to pathogen-directed or narrow-spectrum agents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

