NSTEMI Diagnosis - Spotting the Clues
- Pathophysiology: Partial coronary artery occlusion → myocardial ischemia.
- Clinical Presentation: Anginal chest pain lasting >20 minutes, potentially radiating to the jaw, neck, or left arm.
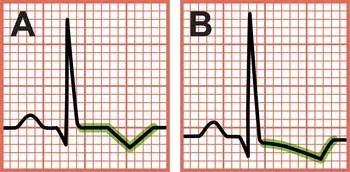
- ECG Findings:
- ST-segment depression
- T-wave inversion
- Can be normal
- Cardiac Biomarkers: ↑ Troponin I or T is the hallmark. Levels rise within 2-4 hours.
⭐ Serial troponin measurements are crucial; a single negative troponin at presentation does not rule out NSTEMI.
Risk Stratification - Sorting the Players
-
Goal: To identify patients who benefit most from an early invasive strategy. This is guided by risk scores and key clinical features.
-
Risk Scores:
- TIMI Score: Assesses 7 factors; a score of ≥ 3 indicates high risk.
- GRACE Score: More predictive for mortality; a score > 140 signifies high risk.
-
High-Risk Features (Mandating an Invasive Strategy):
- Refractory angina despite medical therapy.
- Dynamic ST changes (e.g., new ST depression).
- Hemodynamic instability (hypotension, heart failure).
- Ventricular arrhythmias (VT/VF).
⭐ The GRACE score is a better predictor of in-hospital and long-term mortality than the TIMI score.
Initial Medical Therapy - The Drug Cocktail
Immediate treatment for NSTEMI involves a combination of drugs, often remembered by the mnemonic 📌 MONA-BASH. Note: Oxygen is only given if SpO2 < 90%, and Morphine is used cautiously for persistent pain.
- Dual Antiplatelet Therapy (DAPT):
- Aspirin: 325 mg loading dose, then 81 mg daily.
- P2Y12 Inhibitor: Clopidogrel, Ticagrelor (180 mg loading), or Prasugrel.
- Anticoagulation:
- Unfractionated Heparin (UFH) or Low Molecular Weight Heparin (LMWH).
- Adjunctive Therapy:
- Beta-blockers: Start within 24 hours if no signs of heart failure.
- Nitrates: For ongoing chest pain.
- High-Intensity Statin: e.g., Atorvastatin 80 mg.
⭐ Prasugrel is contraindicated in patients with a history of stroke or TIA.
Invasive vs. Conservative - The Big Decision
Central choice after risk stratification (e.g., TIMI, GRACE score). High-risk patients benefit most from an invasive approach.
-
Immediate Invasive (<2h): For unstable patients.
- Refractory angina
- Hemodynamic instability / cardiogenic shock
- Acute HF
- Sustained VT/VF
-
Ischemia-Guided (Conservative): Medical management, with angiography reserved for recurrent symptoms or positive stress test.
⭐ An early invasive strategy is preferred for high-risk patients (e.g., GRACE score >140) to reduce future ischemic events.
High-Yield Points - ⚡ Biggest Takeaways
- Initial management includes MONA-B (Morphine, Oxygen, Nitrates, Aspirin, Beta-blocker) and anticoagulation (e.g., Heparin).
- All patients receive Dual Antiplatelet Therapy (DAPT), typically aspirin plus a P2Y12 inhibitor.
- Risk stratify using TIMI or GRACE scores to determine invasive vs. conservative strategy.
- High-risk features warrant an early invasive strategy (angiography within 24 hours).
- Low-risk patients can be managed conservatively, often with a stress test to guide further care.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

