Beta-Blockers - The Heart's Bouncers
-
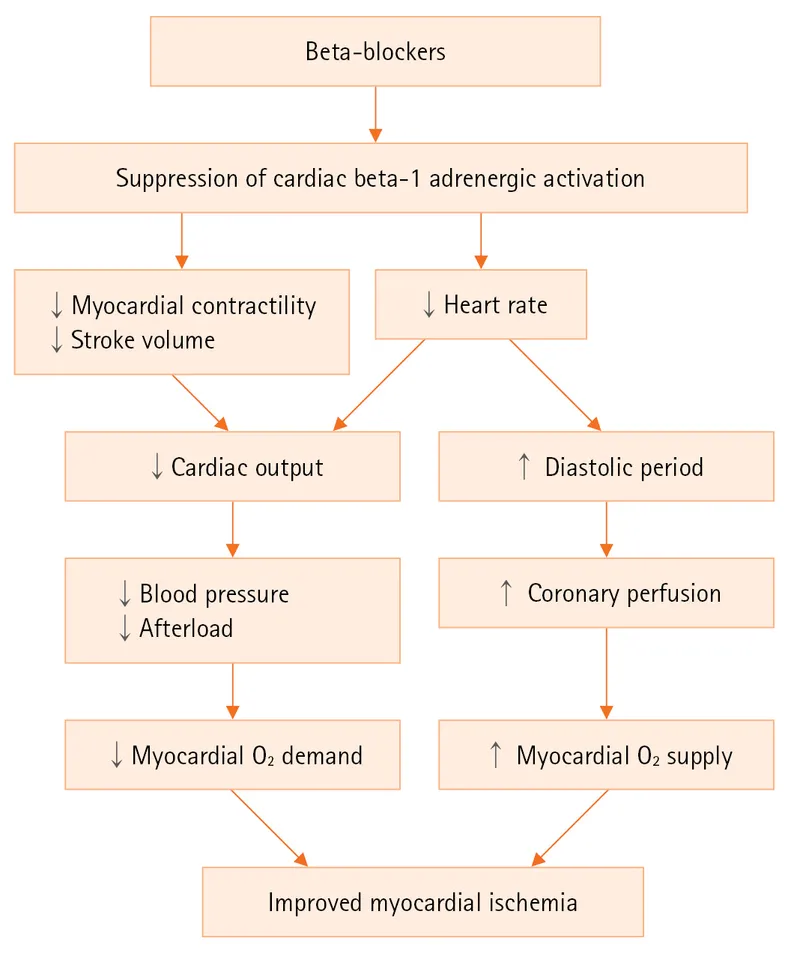
Action: ↓ Heart rate, ↓ contractility, and ↓ blood pressure, leading to decreased myocardial oxygen demand.
-
Initiation: Start within 24 hours post-MI if no contraindications.
-
Cardioselective (β1 > β2): Metoprolol, Atenolol, Bisoprolol. Preferred to minimize side effects.
-
Non-selective (β1 + β2) with α-blocking: Carvedilol, Labetalol.
-
Contraindications:
- Decompensated heart failure (e.g., pulmonary edema)
- Bradycardia (<60 bpm) or high-degree AV block
- Hypotension (SBP <100 mmHg)
- ⚠️ Cocaine-induced MI (risk of unopposed α-adrenergic stimulation).
⭐ Post-MI, beta-blockers are proven to reduce mortality, decrease infarct size, and prevent reinfarction.
ACE-I/ARBs - Remodeling Renegades
- Mechanism: Inhibit the Renin-Angiotensin-Aldosterone System (RAAS) to block Angiotensin II's effects. This ↓ vasoconstriction, ↓ aldosterone secretion, and crucially, prevents adverse cardiac remodeling.
- Clinical Use: Start within 24 hours post-MI in stable patients to reduce mortality and prevent heart failure.
- Key Side Effects:
- Dry cough (ACE-I only 📌 mnemonic: "ACE gives a Cough")
- Hyperkalemia
- Angioedema (rare but serious)
- ⚠️ Contraindicated in pregnancy & bilateral renal artery stenosis.
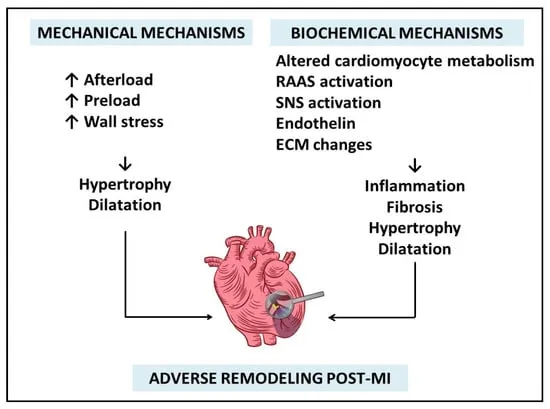
⭐ ACE-I/ARBs are proven to decrease mortality and reduce the incidence of subsequent heart failure by mitigating ventricular remodeling, a key long-term complication of MI.
Statins - Plaque's Worst Enemy
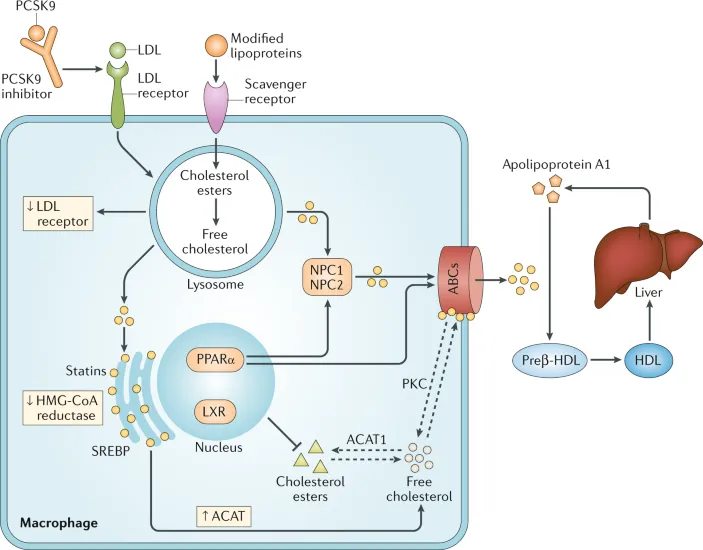
- Mechanism: Inhibit HMG-CoA reductase, the rate-limiting step in cholesterol synthesis. This ↑ LDL receptor expression on hepatocytes, leading to ↑ clearance of LDL from circulation.
- Primary Goal: Lower LDL cholesterol (↓ 20-60%). All post-MI patients should be on a high-intensity statin (e.g., Atorvastatin 80 mg, Rosuvastatin 40 mg).
- Key Side Effects:
- Myopathy/rhabdomyolysis (check CK if symptomatic).
- Hepatotoxicity (monitor LFTs).
⭐ Pleiotropic Effects: Beyond lipid lowering, statins stabilize plaques, reduce inflammation, and improve endothelial function, contributing significantly to cardiovascular risk reduction.
The MI Triple Threat - Synergistic Super-drugs
Post-MI care combines three drug classes targeting distinct pathways to reduce mortality. This synergistic approach is standard for secondary prevention.
⭐ ACE-inhibitors are critical for preventing adverse ventricular remodeling after an MI, which is a primary driver of post-MI heart failure. This benefit is a class effect.
High‑Yield Points - ⚡ Biggest Takeaways
- Beta-blockers (metoprolol, carvedilol) started within 24 hours post-MI ↓ mortality by decreasing myocardial O₂ demand and risk of arrhythmia.
- ACE inhibitors (e.g., lisinopril) are critical to prevent adverse ventricular remodeling and reduce the risk of subsequent heart failure.
- Use ARBs (e.g., valsartan) as an alternative for patients who are intolerant to ACE inhibitors (e.g., due to cough).
- High-intensity statins (atorvastatin, rosuvastatin) must be started immediately in all patients, regardless of baseline cholesterol, for plaque stabilization.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

