Pre-Insulin Steps - Laying the Groundwork
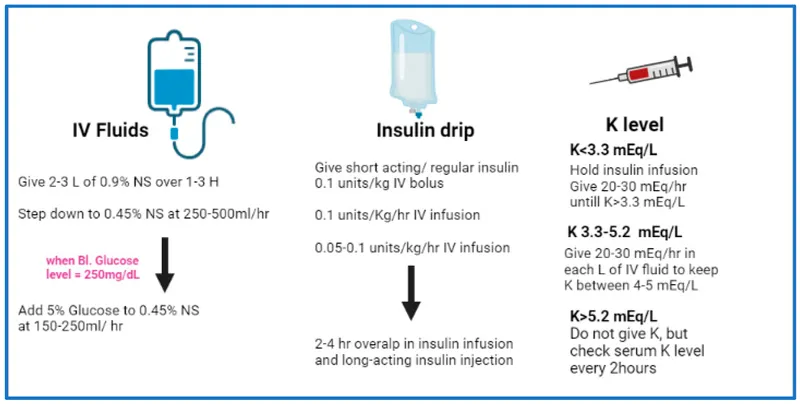
- Secure 2 large-bore IV lines for aggressive fluid and electrolyte administration.
- Initial fluid resuscitation is key: infuse 1-1.5 L of 0.9% NaCl (isotonic saline) over the first hour to restore perfusion.
- Simultaneously, draw initial labs (CMP, ABG/VBG, serum ketones) to establish baseline values, especially for potassium and acidosis.
⭐ The most critical pre-insulin checkpoint is serum potassium. It MUST be > 3.3 mEq/L. Insulin drives K+ intracellularly; administering it during hypokalemia can precipitate life-threatening cardiac arrhythmias.
IV Insulin Protocol - The Main Drip
- Initiate with IV Regular Insulin: bolus of 0.1 units/kg, then a continuous drip at 0.1 units/kg/hr.
- Titrate the infusion to achieve a steady glucose decline of 50-75 mg/dL per hour.
⭐ The primary goal of insulin therapy in DKA is to resolve ketosis and close the anion gap, not just to normalize blood glucose. Insulin must be continued even after glucose normalizes, hence the addition of dextrose to prevent hypoglycemia.
Monitoring & Goals - The Watchful Eye
- Hourly Glucose: Track via fingerstick. Goal ↓ of 50-75 mg/dL per hour.
- ⚠️ A rapid drop >100 mg/dL/hr increases risk for cerebral edema.
- Metabolic Panel (BMP): Every 2-4 hours for K+, HCO3-, and anion gap.
- Anion Gap (AG): Primary marker for resolution. Calculated as $Na^+ - (Cl^- + HCO_3^-)$.
- Goal: Close the gap to <12 mEq/L.
- Resolution Criteria: Glucose <200 mg/dL AND two of the following:
- AG ≤12 mEq/L
- Bicarbonate (HCO3-) ≥15 mEq/L
- Venous pH >7.3
⭐ Once blood glucose reaches ~200 mg/dL, add dextrose (D5W) to IV fluids. This prevents iatrogenic hypoglycemia while allowing the insulin drip to continue, which is essential for resolving the underlying ketoacidosis.
The Transition - IV to SubQ Switch
- Initiate Switch When:
- Blood glucose < 200 mg/dL
- AND at least two of the following:
- Anion gap ≤ 12 mEq/L
- Serum bicarbonate ≥ 15 mEq/L
- Venous pH > 7.3
- Patient is able to tolerate oral intake.
- Protocol:
- Administer basal (long-acting) insulin 1-2 hours before discontinuing the IV insulin drip.
- This overlap prevents rebound hyperglycemia and ketosis.
- Calculate total daily insulin requirement (e.g., 0.5-0.8 U/kg/day), typically split 50% basal and 50% prandial (bolus).
⭐ Exam Favorite: The most common error is stopping the IV insulin infusion simultaneously with the first subcutaneous injection. This creates a gap in insulin coverage, as subcutaneous insulin has a delayed onset, leading to a rapid return to hyperglycemia and ketoacidosis.
High-Yield Points - ⚡ Biggest Takeaways
- IV regular insulin is the cornerstone of DKA management, typically started with a bolus followed by a continuous infusion.
- The primary goal is a steady glucose decline of 50-75 mg/dL per hour.
- Add dextrose (D5W) to IV fluids when serum glucose falls to ~200 mg/dL to prevent hypoglycemia.
- Continue the insulin drip until the anion gap closes and acidosis resolves.
- Administer subcutaneous insulin 1-2 hours before stopping the IV infusion to prevent rebound ketoacidosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

