Initial Assessment - The Acid Test
- Initial Labs: VBG/ABG & Basic Metabolic Panel (BMP).
- Core Triad:
- Metabolic Acidosis: pH < 7.3, HCO₃⁻ < 18 mEq/L.
- High Anion Gap: > 12. Formula: $Na^+ - (Cl^- + HCO_3^-)$.
- Ketosis: Positive serum or urine ketones.
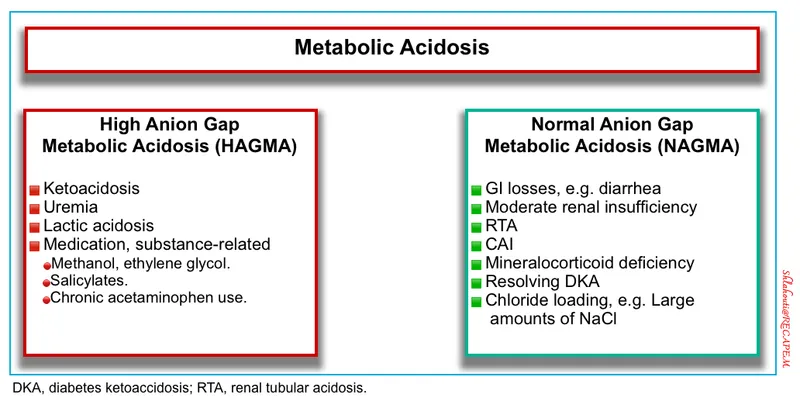
- 📌 MUDPILES for differential diagnosis of high anion gap metabolic acidosis.
⭐ A Venous Blood Gas (VBG) is often sufficient for initial pH and bicarbonate monitoring, sparing the patient from a more invasive ABG.
Bicarbonate Therapy - The Fizz Question
Generally avoided. Insulin is the key to stopping ketogenesis and resolving acidosis. Bicarbonate is a temporary fix with significant risks.
- Indication: Reserved for severe metabolic acidosis where pH < 6.9, leading to hemodynamic compromise.
- Risks:
- Hypokalemia (due to K⁺ shift into cells)
- Volume overload
- Left shift of oxyhemoglobin curve (↓ tissue O₂)
⭐ Paradoxical CNS Acidosis: Infused bicarbonate ($HCO_3^−$) is converted to $CO_2$, which readily crosses the blood-brain barrier. This worsens acidosis in the cerebrospinal fluid, potentially leading to cerebral edema and coma.
Monitoring Response - Gap Watching
- Primary Goal: Close the anion gap (AG). Resolution of DKA is defined by AG closure, not just euglycemia or pH normalization.
- Calculation: $AG = Na^+ - (Cl^- + HCO_3^-)$. Normal is < 12 mEq/L.
- Frequency: Monitor serum electrolytes and calculate the gap every 2-4 hours.
- Transition Criteria: Closing the anion gap to < 12 mEq/L is a key criterion for transitioning from IV insulin to subcutaneous insulin.
⭐ As the ketoacidosis resolves, a transient, non-anion gap hyperchloremic metabolic acidosis may emerge. This is due to renal bicarbonate loss and chloride retention from large-volume saline resuscitation and is typically self-limiting.
Resolution Criteria - The Finish Line
- Primary goal is anion gap closure, not just euglycemia. DKA resolves when the following are met:
- Anion Gap: < 12 mEq/L
- Blood Glucose: < 200 mg/dL
- Serum Bicarbonate: ≥ 15 mEq/L
- Venous pH: > 7.3
- Patient must be clinically stable and able to tolerate oral intake before stopping the insulin infusion.
- Transition Protocol:
- Administer long-acting subcutaneous insulin 1-2 hours before discontinuing the IV insulin drip to prevent relapse into ketoacidosis.
⭐ The anion gap is the first and most important parameter to normalize in DKA treatment; bicarbonate levels often lag behind. Closing the gap indicates cessation of ketone production.
High-Yield Points - ⚡ Biggest Takeaways
- Anion gap closure is the primary therapeutic endpoint, not pH or bicarbonate level.
- Continue IV insulin until the anion gap normalizes, even if glucose is <200 mg/dL.
- Reserve sodium bicarbonate for severe, life-threatening acidemia (pH < 6.9).
- Monitor the anion gap every 2-4 hours to assess DKA resolution.
- Overlap IV and subcutaneous insulin for 1-2 hours before discontinuing the infusion.
- A transient hyperchloremic non-anion gap metabolic acidosis is common during recovery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

