Shock Pathophysiology - Cellular Crisis Mode
- Inadequate tissue perfusion (↓ DO₂) forces cells into anaerobic glycolysis.
- ATP production plummets: $C_6H_{12}O_6 \to 2 \text{ ATP} + \text{Lactate}$.
- Lactic acidosis (↑ serum lactate > 2 mmol/L) develops.
- Failure of Na⁺/K⁺-ATPase pump → cellular edema, lysosomal rupture, and cell death (necrosis/apoptosis).
- Mitochondrial dysfunction becomes irreversible, sealing cell fate.
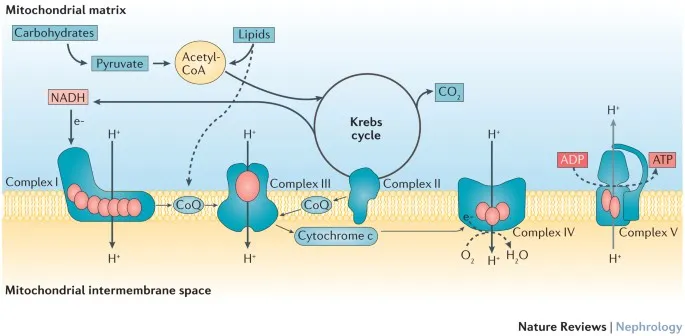
⭐ The transition to irreversible shock is marked by widespread mitochondrial failure, rendering cells unable to use oxygen even if perfusion is restored.
Shock Types - The Four Horsemen
- Hypovolemic: Loss of intravascular volume (e.g., hemorrhage, dehydration).
- Cardiogenic: Primary myocardial pump failure (e.g., MI, heart failure).
- Distributive: Severe peripheral vasodilation (e.g., sepsis, anaphylaxis, neurogenic).
- Obstructive: Extracardiac obstruction to blood flow (e.g., PE, tamponade, tension pneumothorax).
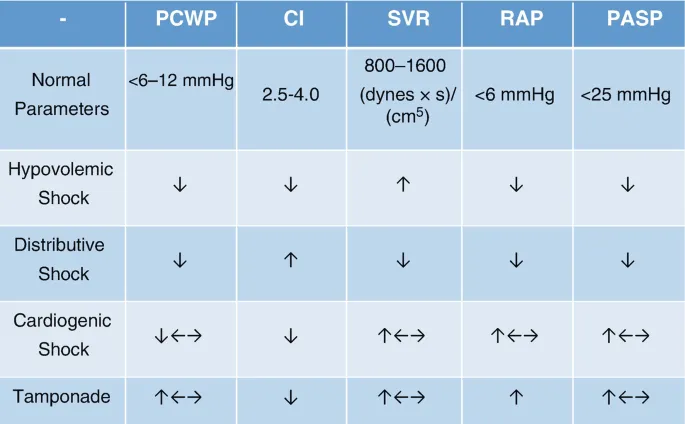
| Shock Type | CVP (Preload) | PCWP (Preload) | CO (Pump) | SVR (Afterload) |
|---|---|---|---|---|
| Hypovolemic | ↓ | ↓ | ↓ | ↑ |
| Cardiogenic | ↑ | ↑ | ↓ | ↑ |
| Distributive | ↓ | ↓ | ↑ (early) / ↓ (late) | ↓ |
| Obstructive | ↑ | N/↓ | ↓ | ↑ |
Patient Presentation - Reading The Signs
-
General Signs of Hypoperfusion:
- Hypotension (MAP < 65 mmHg), tachycardia, tachypnea.
- Altered mental status.
- Cool, clammy skin; oliguria (< 0.5 mL/kg/hr).
-
Key Differentiators:
- Cardiogenic: JVD, pulmonary edema (crackles).
- Hypovolemic: Flat neck veins, dry mucosa.
- Distributive (Septic): Fever, warm/flushed skin (early).
- Obstructive (Tamponade): Beck's Triad (JVD, hypotension, muffled heart sounds).

⭐ Neurogenic shock is unique: presents with hypotension and bradycardia following spinal injury.
Initial Response - Stabilize & Scramble
- ABCs: Airway, Breathing, Circulation. Prioritize immediate life threats.
- Access: Two large-bore (≥16G) peripheral IVs. Administer O₂.
- Action: Start IV fluid resuscitation, typically 30 mL/kg crystalloid bolus for hypotension.
⭐ Serum lactate > 2 mmol/L is a key indicator of tissue hypoperfusion and is associated with increased mortality in shock.
Targeted Treatment - Pick Your Poison
- Cardiogenic: ↓ Contractility → Inotropes (Dobutamine), Diuretics. If hypotensive, use Norepinephrine.
- Hypovolemic: ↓ Preload → Aggressive fluid resuscitation (crystalloids, blood). Vasopressors if refractory.
- Distributive: Massive vasodilation.
- Septic: Norepinephrine is the first-line vasopressor. Add broad-spectrum antibiotics.
- Anaphylactic: Epinephrine (IM first!), antihistamines, corticosteroids.
- Neurogenic: Norepinephrine or Phenylephrine to restore vascular tone.
- Obstructive: Relieve the physical obstruction.
- Tamponade → Pericardiocentesis.
- Tension Pneumothorax → Needle decompression.
- Pulmonary Embolism → Thrombolysis/Thrombectomy.
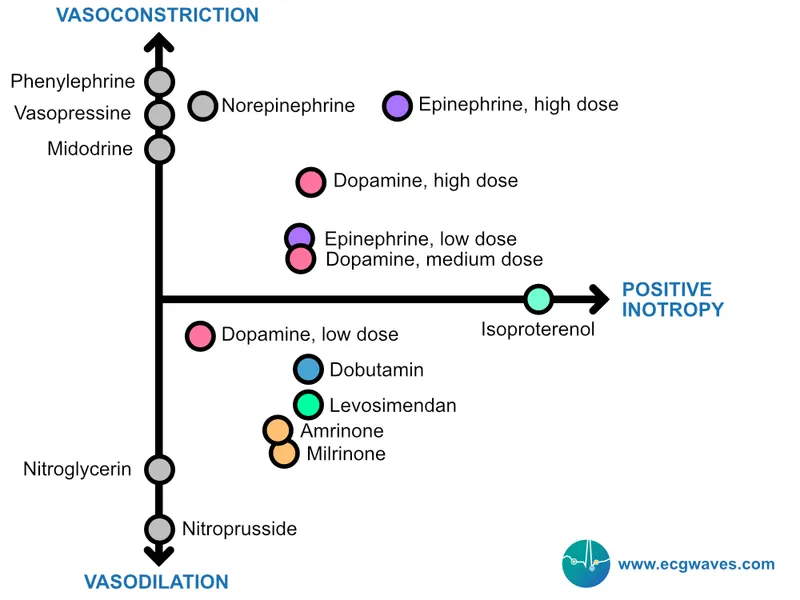
⭐ In septic shock, if Mean Arterial Pressure (MAP) remains < 65 mmHg despite adequate fluid resuscitation, initiate Norepinephrine within the first hour to improve perfusion.
High‑Yield Points - ⚡ Biggest Takeaways
- Distributive shock (septic, anaphylactic) is marked by ↓ Systemic Vascular Resistance (SVR). Septic shock requires IV fluids, broad-spectrum antibiotics, and vasopressors (norepinephrine).
- Cardiogenic shock presents with ↓ Cardiac Output (CO) and ↑ Pulmonary Capillary Wedge Pressure (PCWP). Use inotropes (dobutamine), not aggressive fluids.
- Hypovolemic shock shows ↓ preload (CVP, PCWP) and ↓ CO. Treat with aggressive volume resuscitation.
- Obstructive shock (e.g., PE, tamponade) has ↓ CO from obstruction; treat the underlying cause urgently.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

