ALF Defined - When the Liver Fails Fast
- Rapid, severe liver injury in a previously healthy individual, marked by:
- Hepatic Encephalopathy (HE): Any degree of altered mental status.
- Impaired Synthesis: Coagulopathy with an INR ≥ 1.5.
- Occurs in patients without pre-existing cirrhosis; illness duration is < 26 weeks.
⭐ The hallmark of ALF is the triad of coagulopathy, encephalopathy, and the absence of underlying chronic liver disease. Acetaminophen toxicity is the most common cause in the United States.
Presentation & Dx - Jaundice, Confusion, Crisis
- Clinical Triad:
- Jaundice: Scleral icterus, ↑ bilirubin.
- Hepatic Encephalopathy (HE): Confusion, personality changes, asterixis (liver flap). Graded I-IV.
- Coagulopathy: Bleeding, bruising. Defined by INR > 1.5 without prior cirrhosis.
- Key Labs:
- ↑↑ AST/ALT (often > 1000 IU/L)
- ↑ Ammonia (correlates with HE severity)
- Hypoglycemia
⭐ Acetaminophen toxicity is the leading cause of acute liver failure in the United States.
ALF Management - The Critical First Steps
- ABCs First: Secure airway, breathing, and circulation. Intubate for Grade ≥III encephalopathy to protect against aspiration.
- Transfer: Immediately transfer to an ICU at a liver transplant center.
- Initial Interventions:
- IV Fluids: Judicious use to maintain MAP >75 mmHg (cerebral perfusion).
- Hypoglycemia: Monitor glucose hourly; give IV dextrose if glucose <60 mg/dL.
- Coagulopathy: Correct with FFP/Vitamin K only if actively bleeding.
⭐ NAC for All: N-acetylcysteine (NAC) is given to nearly all ALF patients, regardless of etiology, as it improves systemic redox state and transplant-free survival.
Systemic Havoc - ALF's Complication Cascade
- Cerebral Edema & ↑ ICP: Leading cause of death. Mannitol, hypertonic saline. Goal: ICP < 20 mmHg, CPP > 60 mmHg.
- Coagulopathy: ↓ Synthesis of clotting factors (II, V, VII, IX, X). INR ≥ 1.5. High bleeding risk.
- Hemodynamic Instability: Systemic vasodilation, ↓ SVR, high-output state mimicking septic shock.
- Renal Failure: Acute kidney injury (AKI) is common. Hepatorenal syndrome (HRS) is a grim sign.
- Infections: Bacterial/fungal infections are frequent triggers and complications.
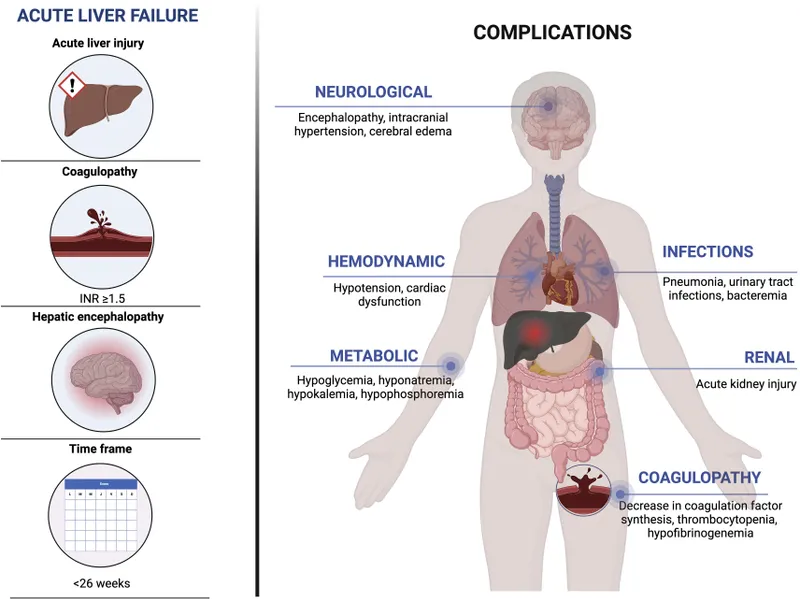
⭐ Grade III/IV hepatic encephalopathy carries the highest risk for cerebral edema and subsequent brainstem herniation.
Transplant Criteria - The Ultimate Lifeline
- King's College Criteria (KCC): Key for determining transplant need in ALF. Different criteria for acetaminophen vs. non-acetaminophen causes.
- Acetaminophen-induced ALF:
- Arterial pH < 7.3 (after resuscitation) OR
- All three: INR > 6.5, Creatinine > 3.4 mg/dL, Grade III-IV encephalopathy.
- Non-Acetaminophen ALF:
- INR > 6.5 OR
- Any 3: Age <10/>40, unfavorable etiology, jaundice >7 days before encephalopathy, INR > 3.5, Bilirubin > 17.5 mg/dL.
- Acetaminophen-induced ALF:
⭐ While KCC is classic, the MELD score is also frequently used, and a high MELD score ( >30) is a strong predictor of mortality and indication for transplant listing.
High-Yield Points - ⚡ Biggest Takeaways
- Acute liver failure is defined by hepatic encephalopathy and an INR ≥1.5 in a patient without pre-existing cirrhosis.
- Acetaminophen toxicity is the most common cause in the U.S.; always check an acetaminophen level.
- The classic presentation triad is jaundice, coagulopathy, and encephalopathy.
- Cerebral edema is the most life-threatening complication, causing intracranial hypertension.
- Management requires ICU-level care, treating the underlying cause (e.g., N-acetylcysteine), and urgent evaluation for liver transplantation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

