Pathophysiology & Presentation - The Synovial Showdown
- Pathogenesis: Genetic susceptibility (HLA-DR4) + environmental trigger → T-cell activation.
- B-cells produce Rheumatoid Factor (RF) & highly specific Anti-Citrullinated Protein Antibodies (ACPA).
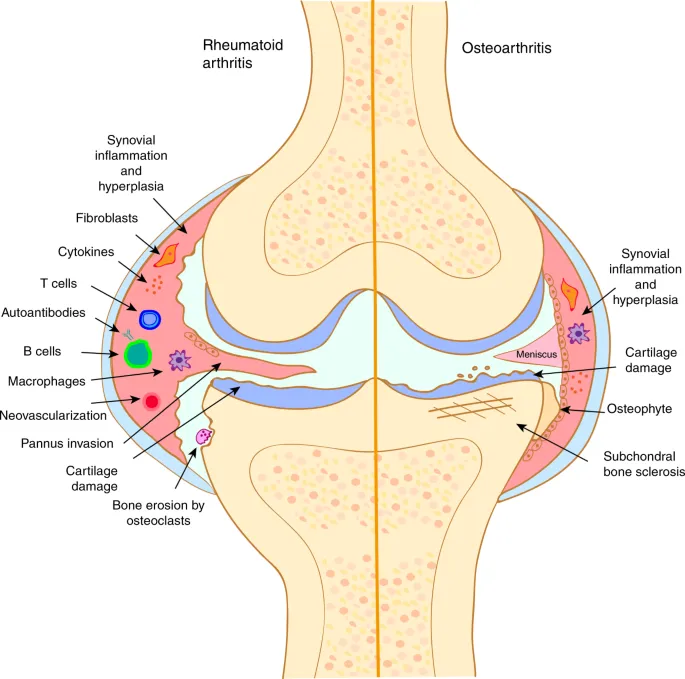
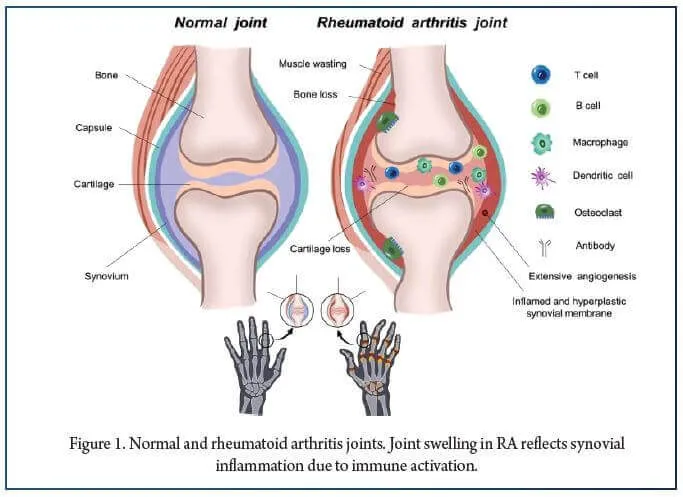
- Synovial inflammation & proliferation → pannus formation (destructive granulation tissue).
- Pannus erodes articular cartilage and bone.
- Key cytokines: TNF-α, IL-1, IL-6.
- Clinical Presentation: Insidious, symmetric, inflammatory polyarthritis.
- Morning stiffness > 1 hour, improves with activity.
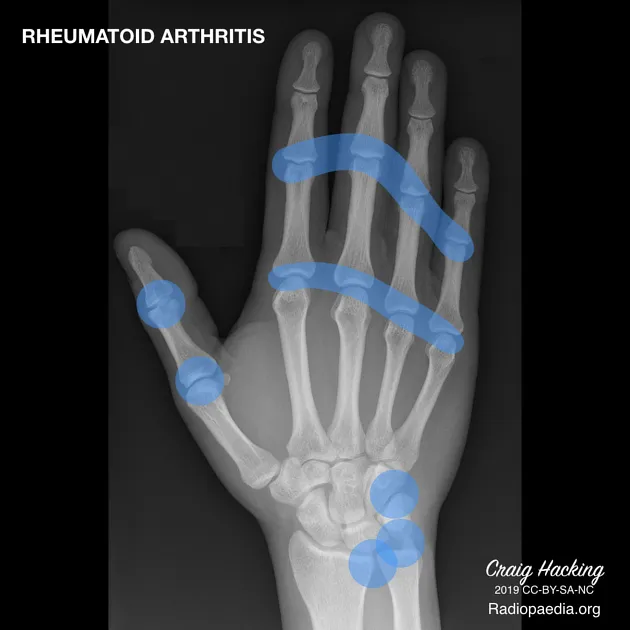
- Affects small joints: MCPs, PIPs, wrists, MTPs.
- Systemic symptoms: low-grade fever, fatigue, weight loss.
⭐ Exam Favorite: RA characteristically spares the distal interphalangeal (DIP) joints, a key feature distinguishing it from osteoarthritis.
Diagnosis & Serology - Cracking the RA Code
-
ACR/EULAR 2010 Criteria: Score ≥6/10 for definitive RA diagnosis.
- Joints (0-5): Based on number & size of joints.
- Serology (0-3): RF & anti-CCP levels.
- Acute Phase Reactants (0-1): ↑ESR or ↑CRP.
- Duration (0-1): Symptoms ≥6 weeks.
-
Key Antibodies:
- Anti-CCP (ACPA): Most specific marker (~95%); predicts erosive disease.
- Rheumatoid Factor (RF): Sensitive but not specific.
-
Other Labs:
- Synovial Fluid: Inflammatory (WBC 2,000-75,000/μL, >50% PMNs).
-
Imaging (X-ray):
- Early: Soft tissue swelling, periarticular osteopenia.
- Late: Joint space narrowing, marginal erosions.
⭐ High-Yield: Anti-CCP antibodies may be positive years before clinical symptoms manifest, identifying individuals at high risk for developing RA.
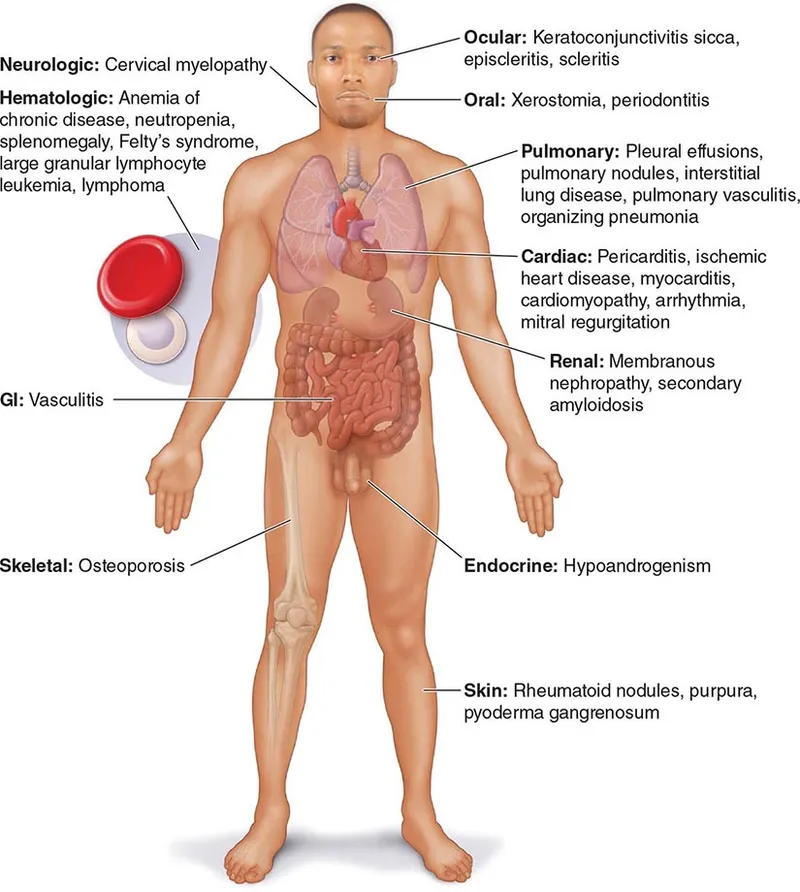
Extra-Articular Manifestations - Systemic Synovial Strike
- General: Fever, weight loss, fatigue, myalgias.
- Dermatologic:
- Rheumatoid nodules: Firm, subcutaneous on extensor surfaces (e.g., olecranon, occiput).
- Rheumatoid vasculitis: Palpable purpura, skin ulcers.
- Pulmonary:
- Pleuritis, pleural effusion (exudative, low glucose).
- Interstitial Lung Disease (ILD).
- Caplan Syndrome: Pneumoconiosis + rheumatoid nodules in lungs.
- Cardiovascular:
- Pericarditis is most common.
- Accelerated atherosclerosis, ↑ risk of MI.
- Ocular: Keratoconjunctivitis sicca, scleritis.
- Hematologic: Anemia of chronic disease, thrombocytosis.
⭐ Felty Syndrome: A severe complication characterized by the triad of long-standing RA, splenomegaly, and neutropenia (<2,000/mm³), leading to recurrent infections.
RA Management - Taming the Flame
- Goal: Control synovitis, prevent joint damage, preserve function. Bridge with NSAIDs/corticosteroids for flares.
- DMARDs:
- csDMARDs: Methotrexate, Sulfasalazine, Hydroxychloroquine (retinal toxicity), Leflunomide.
- bDMARDs (TNF-α inhibitors): Etanercept, Infliximab. ↑ risk of infection.
- tsDMARDs (JAK inhibitors): Tofacitinib. ↑ risk of thrombosis, shingles.
⭐ Before initiating biologic DMARDs (e.g., TNF-α inhibitors), screening for latent Tuberculosis (PPD/IGRA) and viral hepatitis (B & C) is mandatory.
High‑Yield Points - ⚡ Biggest Takeaways
- Symmetrical, inflammatory polyarthritis primarily affecting small joints (MCP, PIP) while sparing the DIP joints.
- Hallmark is morning stiffness lasting > 60 minutes that improves with activity.
- Key serological markers include Rheumatoid Factor (RF) and the more specific anti-citrullinated peptide (anti-CCP) antibodies.
- Characteristic deformities include ulnar deviation, swan-neck, and boutonnière deformities.
- Methotrexate is the cornerstone first-line DMARD for management.
- Associated with C1-C2 subluxation (atlantoaxial instability) and systemic features like rheumatoid nodules.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

