Giant Cell Arteritis - The Blinding Headache
- Patho: Granulomatous vasculitis of large & medium vessels, esp. cranial branches from aortic arch.
- Classic Patient: Female > 50 years old, often with Polymyalgia Rheumatica (PMR).
- Symptoms:
- New-onset, unilateral temporal headache.
- Jaw claudication (pain on chewing).
- Amaurosis fugax (transient vision loss) → can lead to permanent blindness.
- Constitutional: fever, fatigue, weight loss.
- Exam: Tender, thickened, or pulseless temporal artery.
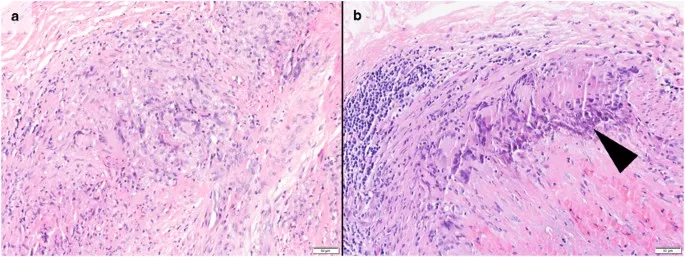
- Diagnosis & Management
⭐ High-Yield: Up to 50% of patients with GCA have concurrent Polymyalgia Rheumatica (PMR), presenting with pain and stiffness in the shoulders and hips.
Takayasu Arteritis - The Pulseless Disease
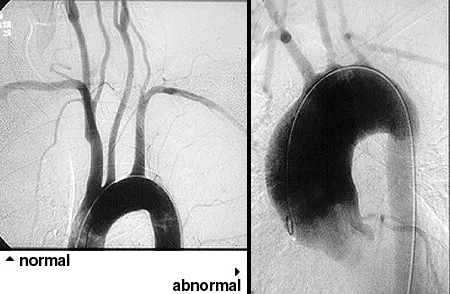
- Pathophysiology: Granulomatous vasculitis affecting the aorta and its major branches.
- Epidemiology: Typically presents in women of Asian descent, age < 50 years.
- Clinical Features ("Pulseless Disease"):
-
- Systemic: Fever, malaise, weight loss, arthralgias.
-
- Vascular: ↓ pulses, limb claudication, arterial bruits, and BP discrepancy >10 mmHg between arms.
-
- Diagnosis:
-
- Labs: ↑ ESR, ↑ CRP.
-
- Imaging: CT or MR Angiography (CTA/MRA) is the gold standard to visualize vessel wall thickening and stenosis.
-
- Treatment: High-dose corticosteroids (e.g., prednisone).
⭐ The subclavian artery is the most commonly affected vessel.
Diagnosis & Treatment - Compare & Conquer
| Feature | Giant Cell Arteritis (GCA) | Takayasu Arteritis (TAK) |
|---|---|---|
| Gold Std | Temporal Artery Biopsy: mononuclear infiltrates, giant cells | N/A (clinical + imaging) |
| Imaging | Ultrasound: "Halo sign" (edema) | MRA/CTA: Aortic/branch stenosis, wall thickening |
| Labs | ↑↑ ESR (>50), ↑ CRP | ↑ ESR, ↑ CRP |
| Initial Tx | High-dose prednisone (40-60mg/day) immediately to prevent blindness | High-dose prednisone |
| Long-term | Tocilizumab (anti-IL-6), Methotrexate | Tocilizumab, Methotrexate |
| Adjunct | Low-dose Aspirin (reduces stroke risk) | Anti-hypertensives, anti-platelets |
⭐ Visual confirmation is key: A positive "halo sign" on temporal artery ultrasound is highly specific for GCA, while angiography revealing stenosis or aneurysms of the aorta and its main branches is the cornerstone of Takayasu diagnosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Giant Cell Arteritis (GCA) typically affects females >50 with new-onset headache, jaw claudication, and scalp tenderness; it is strongly associated with Polymyalgia Rheumatica (PMR).
- The greatest risk is irreversible blindness, mandating immediate high-dose corticosteroids even before diagnosis is confirmed.
- Takayasu Arteritis (“pulseless disease”) classically affects Asian females <40, involving the aortic arch and causing disparate BPs and claudication.
- Definitive diagnosis for GCA is temporal artery biopsy; for Takayasu, it's imaging (MRA/CTA).
- Both present with constitutional symptoms and markedly elevated ESR and CRP.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

