Pulmonary Rehab - Get Up and Go!
- Indications: Symptomatic patients with COPD (GOLD 2-4), interstitial lung disease (ILD), cystic fibrosis, and selected pre/post-thoracic surgery cases.
- Goals: ↓ dyspnea, ↑ exercise capacity & quality of life (QoL), ↓ healthcare utilization.
- Core Components:
- Exercise Training: Aerobic (treadmill, cycling), strength training. Typically 6-12 weeks.
- Education: Disease process, medication adherence (esp. inhaler technique), nutrition, oxygen use.
- Psychosocial Support: Manages anxiety/depression common in chronic lung disease.

⭐ Primary benefit: Improved dyspnea, exercise tolerance, and quality of life. It does not typically improve underlying spirometry numbers (FEV1).
Patient Selection - Who Gets the Invite?
- Primary Indication: Patients with chronic respiratory disease who remain symptomatic despite optimal medical therapy.
- Eligible Conditions:
- COPD (most common, especially GOLD stages B-D)
- Interstitial Lung Disease (e.g., IPF, sarcoidosis)
- Bronchiectasis & Cystic Fibrosis
- Pre- and post-operative lung surgery (transplant, LVRS)
- Core Requirements:
- Significant dyspnea impacting quality of life (e.g., mMRC grade ≥ 2).
- Reduced exercise capacity limiting daily activities.
- Patient must be motivated and medically stable (e.g., >4 weeks post-exacerbation).
- Key Contraindications:
- Unstable cardiac disease (unstable angina, recent MI).
- Limiting comorbidities (severe arthritis, cognitive impairment).
⭐ High-Yield: The BODE index (Body-mass index, airflow Obstruction, Dyspnea, Exercise capacity) helps risk-stratify COPD patients. A higher score indicates a greater mortality risk and strengthens the case for referral.
Program Components - The Rehab Recipe
-
Exercise Training (Cornerstone):
- Minimum 6-8 week program, typically 2-3 sessions/week.
- Aerobic: Walking, cycling, targeting 60-80% of peak work rate.
- Strength: Resistance training for major muscle groups.
- Breathing Retraining: Pursed-lip & diaphragmatic breathing techniques to reduce dynamic hyperinflation.
-
Education & Self-Management:
- Inhaler and oxygen device proficiency.
- Airway clearance techniques.
- Early recognition and management of exacerbations.
-
Psychosocial Support:
- Counseling for anxiety and depression, which are common comorbidities.
- Group sessions foster peer support.
-
Nutritional Counseling:
- Address weight loss and muscle cachexia or obesity to optimize respiratory muscle function.
⭐ Primary Goal: The main benefits are ↑ exercise tolerance, ↓ dyspnea, and ↑ quality of life. It does not significantly alter FEV1 or reverse lung damage.
Benefits & Outcomes - The Winning Formula
-
Physiological Gains:
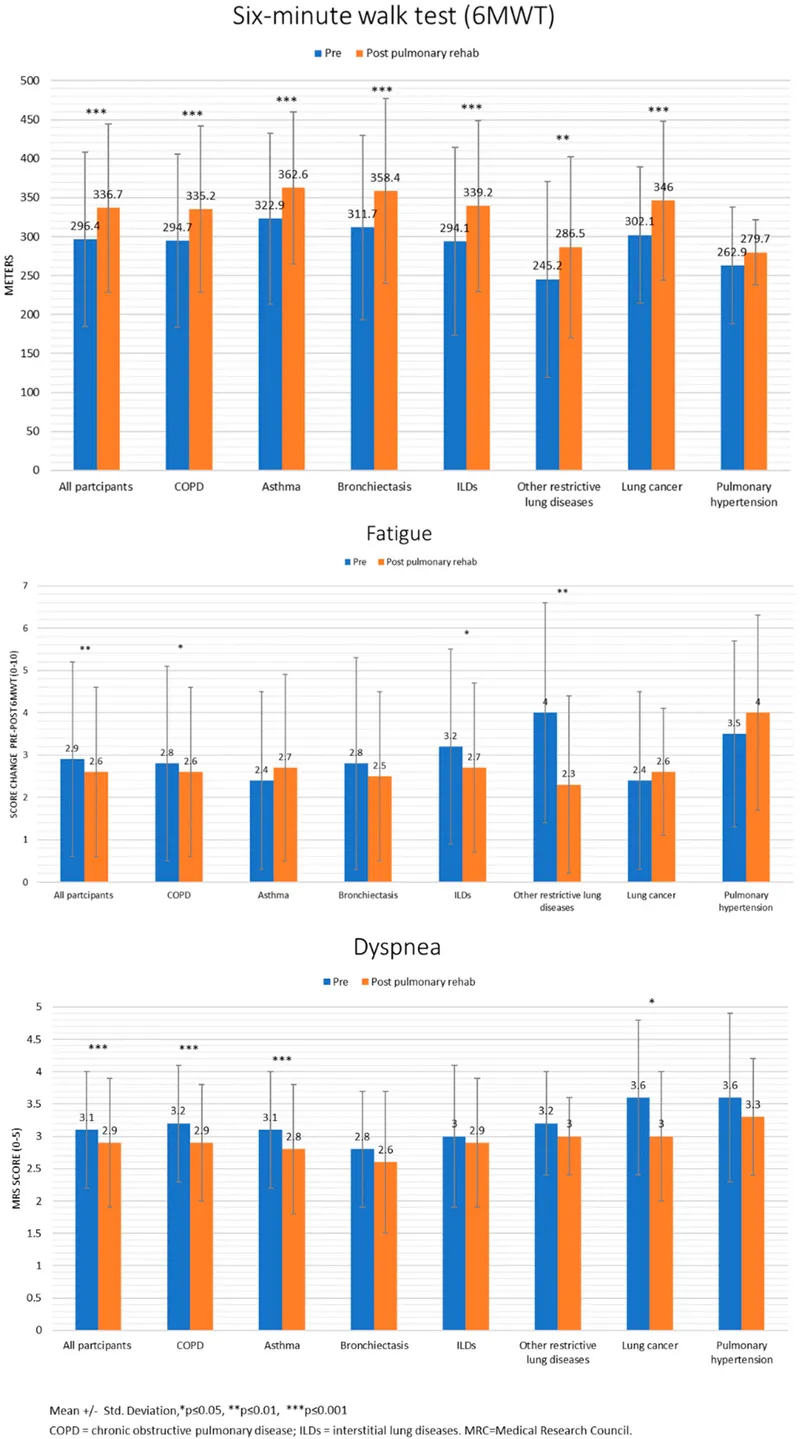
- ↑ Exercise capacity (e.g., improved 6-minute walk distance)
- ↓ Dyspnea perception (improved BDI/TDI scores)
- ↑ Peripheral muscle strength & endurance
- Improved respiratory muscle function
-
Psychosocial & Systemic Impact:
- ↑ Health-related quality of life (HRQoL)
- ↓ Anxiety and depression symptoms
- ↑ Self-efficacy for disease management
⭐ The most significant outcome is a ~50% reduction in hospital admissions and length of stay for COPD exacerbations.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary rehab is a multidisciplinary program: exercise training, education, and psychosocial support.
- Primary indication: Symptomatic COPD (MRC dyspnea grade ≥2), especially post-exacerbation.
- Key goals: Improve exercise capacity, reduce dyspnea, and enhance quality of life.
- Significantly reduces hospitalizations and healthcare utilization.
- Benefits are not from improving PFTs (FEV1) but from addressing peripheral muscle dysfunction and deconditioning.
- Also beneficial in interstitial lung disease and severe asthma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

