Pathophysiology - Scarred for Life
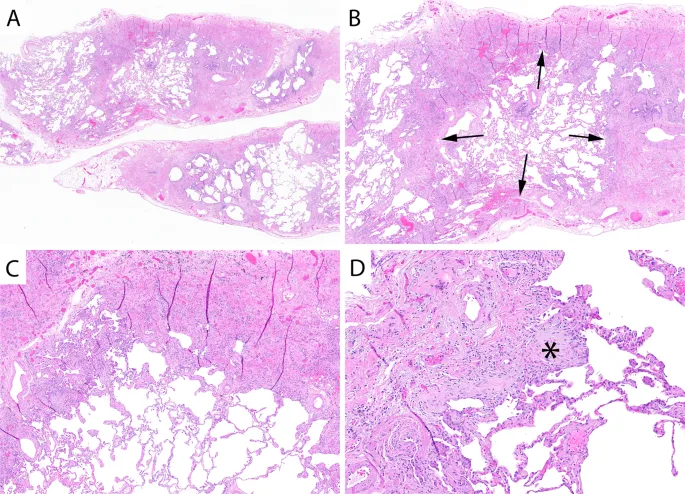
- Hallmark: Biopsy reveals Usual Interstitial Pneumonia (UIP), a pattern of progressive fibrosis.
- Mechanism: Begins with repetitive, microscopic injury to alveolar epithelial cells, leading to aberrant wound healing.
- Key Mediators: Involves pro-fibrotic cytokines, primarily TGF-β1, which stimulates fibroblast proliferation and excessive extracellular matrix (collagen) deposition.
⭐ Classic finding is spatial & temporal heterogeneity: patches of late-stage honeycomb fibrosis alternate with less affected or normal lung tissue.
Clinical Presentation & Diagnosis - Can't Catch a Breath
- Presentation: Insidious onset of dyspnea on exertion (DOE) and a persistent dry cough, typically for > 6 months.
- On Examination:
- Fine, bibasilar inspiratory crackles ("Velcro-like" rales).
- Digital clubbing is present in up to 50% of cases.
- Pulmonary Function Tests (PFTs):
- Classic restrictive pattern: ↓ FVC, ↓ TLC, with a normal or ↑ FEV1/FVC ratio.
- Markedly ↓ DLCO (diffusing capacity for carbon monoxide).
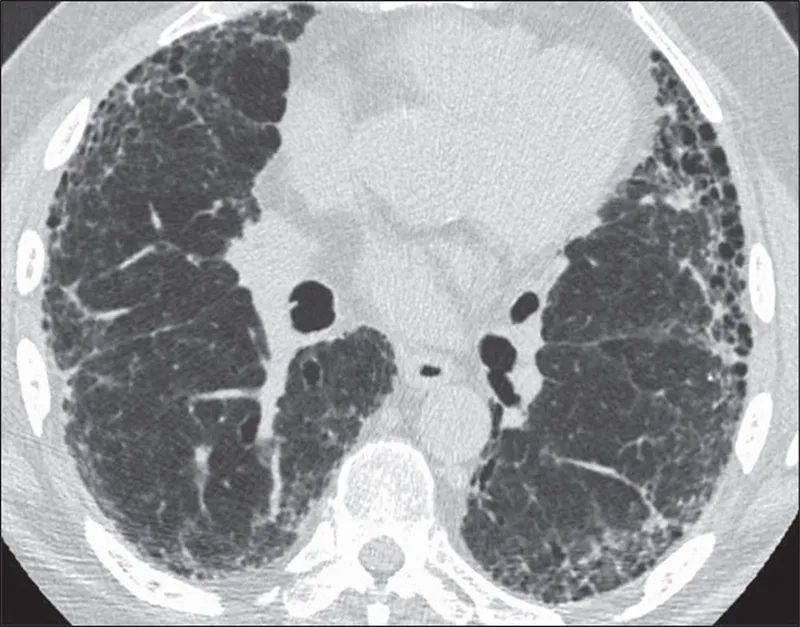
- High-Resolution CT (HRCT):
- The key diagnostic modality, often sufficient for diagnosis.
- Shows a "Usual Interstitial Pneumonia" (UIP) pattern:
- Honeycombing (clustered cystic airspaces).
- Traction bronchiectasis.
- Reticular opacities with a subpleural, bibasilar predominance.
⭐ The combination of bibasilar "Velcro-like" crackles and digital clubbing in a patient > 60 years old is highly suggestive of IPF.
Radiology & Histopathology - Honeycomb Lungs
-
High-Resolution CT (HRCT): Primary imaging modality.
- Hallmark: Honeycombing (clustered, thick-walled cystic airspaces).
- Distribution: Predominantly bibasilar and subpleural.
- Other findings: Reticular opacities, traction bronchiectasis, minimal ground-glass opacities.
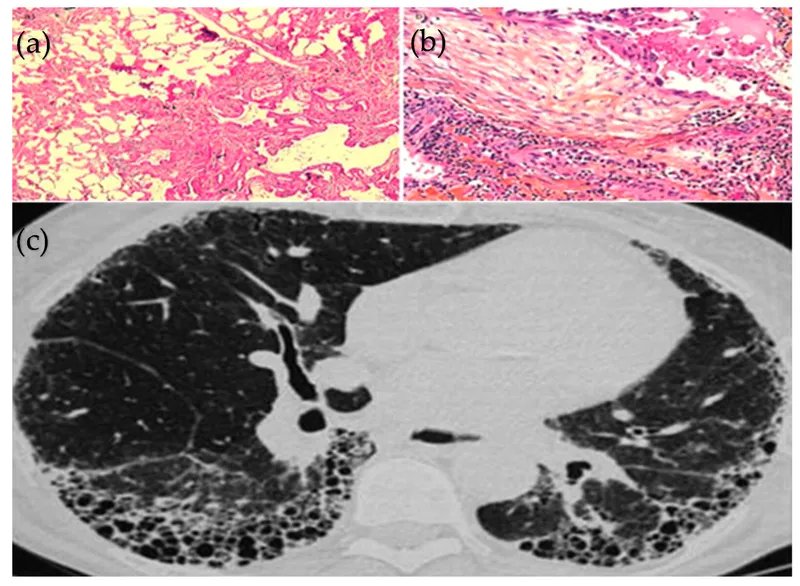
-
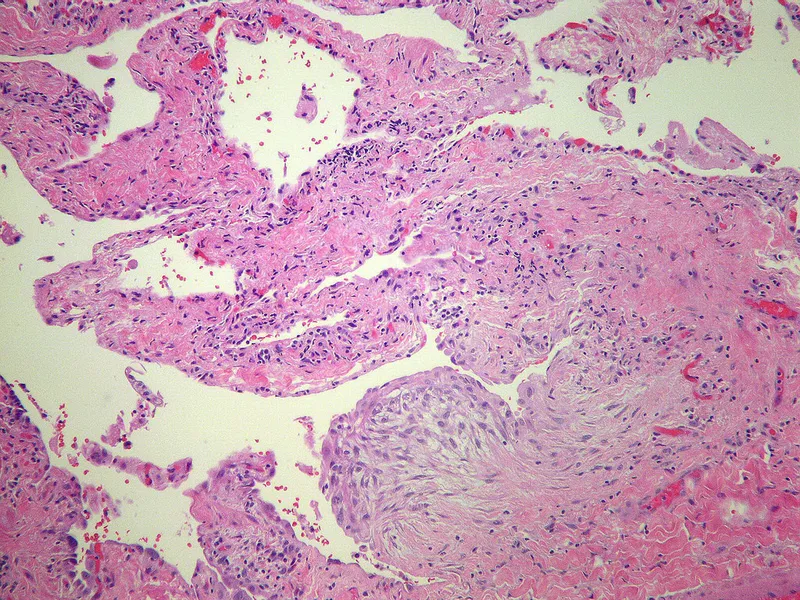
Histopathology (Biopsy): Shows Usual Interstitial Pneumonia (UIP) pattern.
- Key Feature: Temporal heterogeneity (alternating areas of normal lung, inflammation, and dense fibrosis).
- Microscopic hallmark: Fibroblastic foci (collections of active fibroblasts).
⭐ Exam Favorite: A "definite UIP" pattern on HRCT (bibasilar, subpleural honeycombing) is so specific that a surgical lung biopsy is often not required for diagnosis in the right clinical context.
Management & Prognosis - Slowing the Scarring
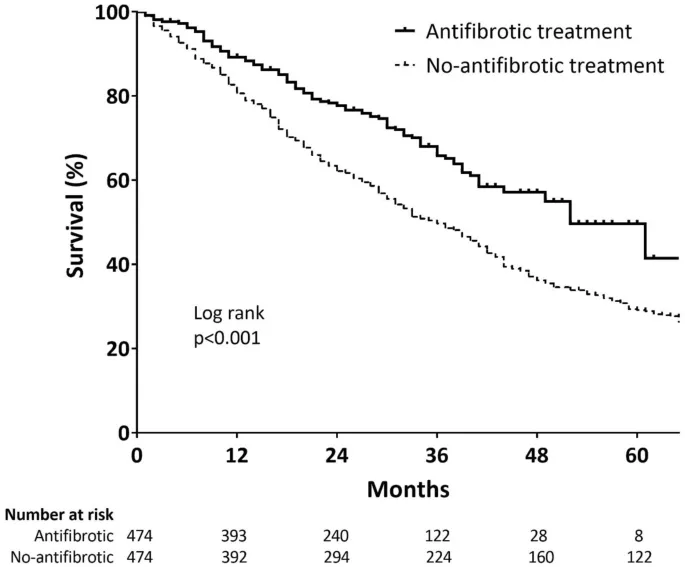
- Antifibrotic Therapy: Goal is to slow Forced Vital Capacity (FVC) decline.
- Pirfenidone: Inhibits TGF-β, a key mediator of fibrosis.
- Nintedanib: A tyrosine kinase inhibitor targeting pro-fibrotic pathways (VEGFR, FGFR, PDGFR).
- Supportive & Symptomatic Care:
- Supplemental O₂ for hypoxemia (maintain SaO₂ >88%).
- Pulmonary rehabilitation to improve dyspnea and quality of life.
- Vaccinations (influenza, pneumococcus).
- Definitive Treatment:
- Lung transplantation is the only curative option for eligible candidates.
- Prognosis:
- Median survival is 3-5 years post-diagnosis.
⭐ Acute exacerbations of IPF are a major cause of mortality, with in-hospital mortality rates often exceeding 50%.
High‑Yield Points - ⚡ Biggest Takeaways
- Idiopathic pulmonary fibrosis (IPF) is a progressive, fibrosing interstitial pneumonia, mainly in males >60.
- Presents with gradual dyspnea on exertion and a persistent non-productive cough.
- Classic physical finding: bibasilar inspiratory "Velcro-like" crackles.
- HRCT is key for diagnosis, showing a UIP pattern with bibasilar, subpleural honeycombing.
- PFTs show a restrictive pattern (↓ FVC, normal/↑ FEV1/FVC ratio) and severely ↓ DLCO.
- Pirfenidone and nintedanib slow disease progression; lung transplant is the only definitive cure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

