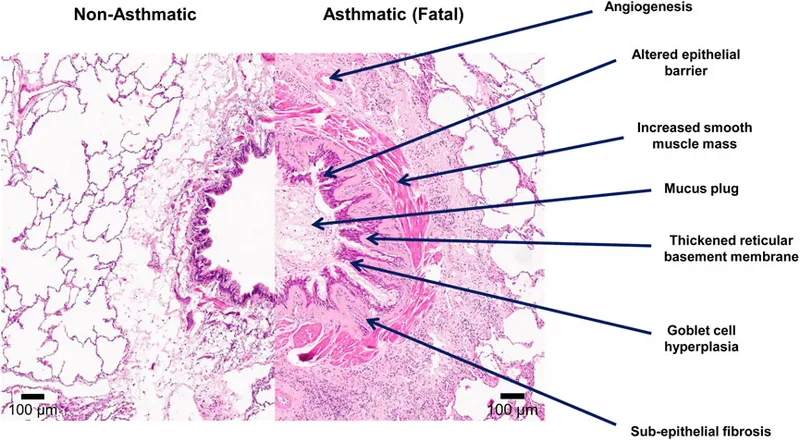
Pathophysiology - Bronchial Bedlam
- Core Mechanism: Chronic airway inflammation driven by a Type I (IgE-mediated) hypersensitivity reaction, leading to bronchial hyperresponsiveness and reversible obstruction.
- Key Cellular Players: Th2 lymphocytes, eosinophils, mast cells, and IgE antibodies.
- Phases:
- Early: Trigger exposure → mast cell degranulation → release of histamine & leukotrienes → acute bronchoconstriction.
- Late: Cytokine-mediated influx of inflammatory cells (esp. eosinophils) → sustained inflammation and edema.
⭐ Aspirin-Exacerbated Respiratory Disease (AERD) / Samter's Triad: A distinct asthma phenotype characterized by asthma, chronic rhinosinusitis with nasal polyps, and severe reactions to aspirin/NSAIDs.
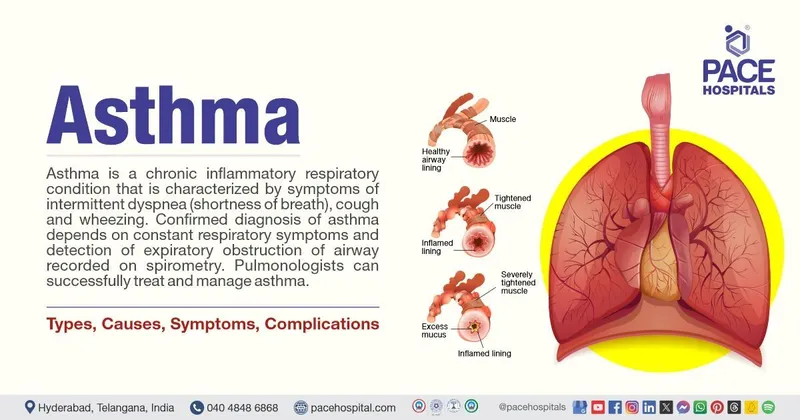
Clinical Presentation - The Wheezing Wail
- Episodic symptoms: dyspnea, chest tightness, and cough (often worse at night).
- Classic sign: High-pitched, polyphonic expiratory wheeze.
- Common Triggers:
- Allergens (dust mites, pollen), exercise, cold air.
- Viral infections, GERD, stress.
- Medications: Aspirin (AERD), non-selective β-blockers.
- Associated Conditions: 📌 Atopic Triad (Asthma + Allergic Rhinitis + Atopic Dermatitis).
- Severe Exacerbation Signs:
- Accessory muscle use, tripoding posture.
- Pulsus paradoxus: Inspiratory SBP drop > 10 mmHg.
⭐ A "silent chest" in an acutely dyspneic patient is an ominous sign indicating severe airflow limitation and impending respiratory failure.
Diagnosis - The Spirometry Story
- Spirometry: The cornerstone of asthma diagnosis, measuring airflow and lung volumes.
- Key Finding: Reversible obstructive pattern.
- Initial Test: ↓ Forced Expiratory Volume in 1 second (FEV1) and ↓ FEV1/FVC ratio ($< \textbf{0.7}$ in adults).
- Flow-volume loop shows a "scooped-out" or concave pattern during exhalation.
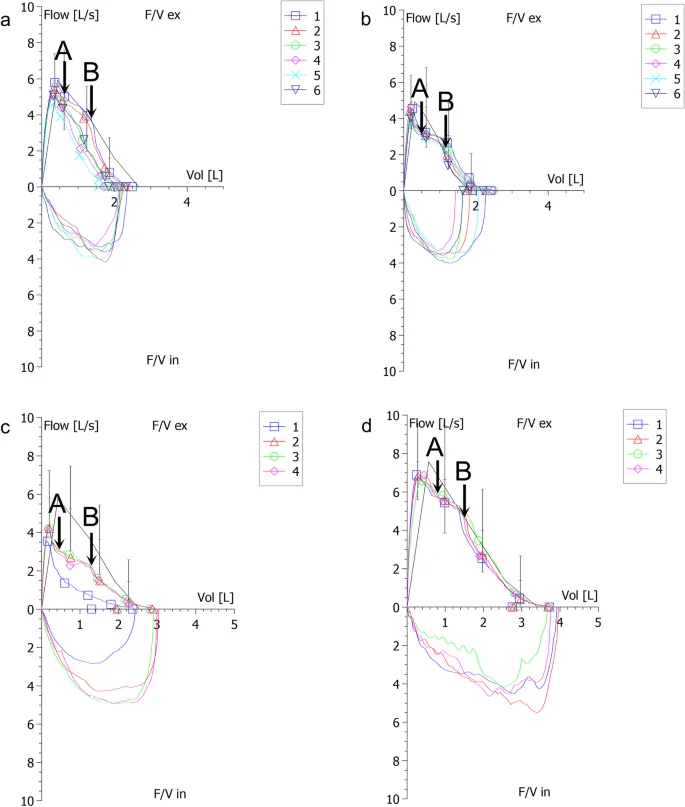
- Confirmation Algorithm:
⭐ Fractional Exhaled Nitric Oxide (FeNO): A non-invasive test measuring eosinophilic airway inflammation. An elevated FeNO level ($> \textbf{50}$ ppb in adults) can support a diagnosis of asthma, particularly in cases with normal spirometry.
Severity Classification - The Asthma Ladder
Classification is based on impairment (symptoms, SABA use, lung function) and risk of exacerbations. Assessed before treatment is initiated.
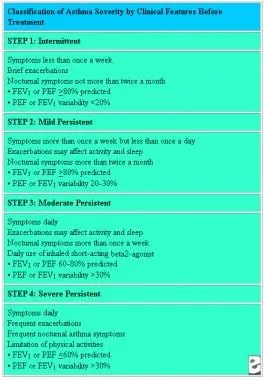

- Intermittent
- Symptoms: ≤2 days/week
- Nighttime awakenings: ≤2x/month
- SABA use: ≤2 days/week
- FEV1: >80% predicted
- Mild Persistent
- Symptoms: >2 days/week (not daily)
- Nighttime awakenings: 3-4x/month
- FEV1: >80% predicted
- Moderate Persistent
- Symptoms: Daily
- Nighttime awakenings: >1x/week (not nightly)
- FEV1: 60-80% predicted
- Severe Persistent
- Symptoms: Throughout the day
- Nighttime awakenings: Often 7x/week
- FEV1: <60% predicted
⭐ The goal of the "ladder" approach is to step up therapy to gain control, then step down to the minimum level needed to maintain control.
High‑Yield Points - ⚡ Biggest Takeaways
- Asthma is a chronic inflammatory disorder characterized by bronchial hyperresponsiveness and reversible airflow obstruction.
- It's a Type I hypersensitivity reaction involving IgE, mast cells, and eosinophils.
- Diagnosis is confirmed by spirometry showing an obstructive pattern (FEV1/FVC < 0.7).
- Reversibility is key: >12% and 200 mL ↑ in FEV1 post-bronchodilator.
- A methacholine challenge can diagnose asthma if initial spirometry is normal.
- Classic sputum findings include Curschmann spirals and Charcot-Leyden crystals.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

