SIRS & MODS - The Domino Effect
- A massive release of pancreatic enzymes & cytokines (TNF-α, IL-1, IL-6) triggers Systemic Inflammatory Response Syndrome (SIRS).
- SIRS Criteria (need ≥2):
- Temp: <36°C or >38°C
- Heart Rate: >90 bpm
- Resp Rate: >20 or PaCO₂ <32 mmHg
- WBC: <4k or >12k/mm³, or >10% bands
- Unchecked SIRS progresses to Multi-Organ Dysfunction Syndrome (MODS), the primary driver of late mortality.
⭐ Acute Respiratory Distress Syndrome (ARDS) is the most common cause of death in the first week of severe acute pancreatitis.
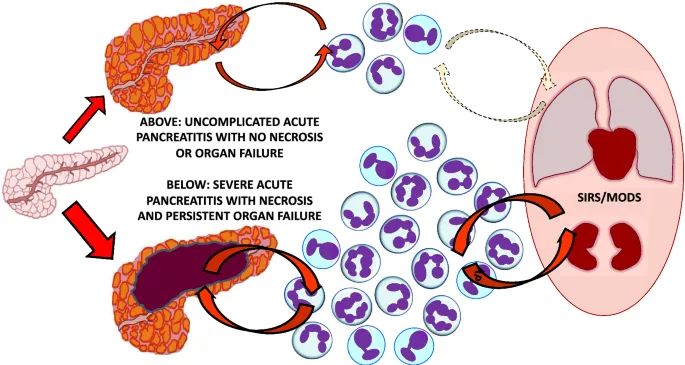
Pulmonary Failure - Lungs Under Siege
- Acute Respiratory Distress Syndrome (ARDS) is the most common systemic complication and a major cause of death.
- Pathophysiology: Circulating pancreatic enzymes (e.g., phospholipase A₂) and cytokines damage the alveolar-capillary membrane, leading to ↑ permeability and non-cardiogenic pulmonary edema.
- Clinical Features: Rapid onset of dyspnea, tachypnea, and severe hypoxemia refractory to supplemental oxygen.
- Auscultation: Bilateral crackles.
- CXR: Diffuse bilateral pulmonary infiltrates, resembling heart failure but with a normal pulmonary capillary wedge pressure (PCWP < 18 mmHg).
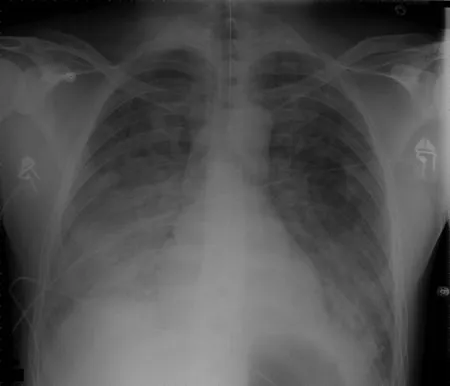
⭐ Exam Favorite: The hallmark of ARDS is severe hypoxemia with a PaO₂/FiO₂ ratio < 300, with bilateral "white-out" on chest X-ray, occurring within one week of the initial insult.
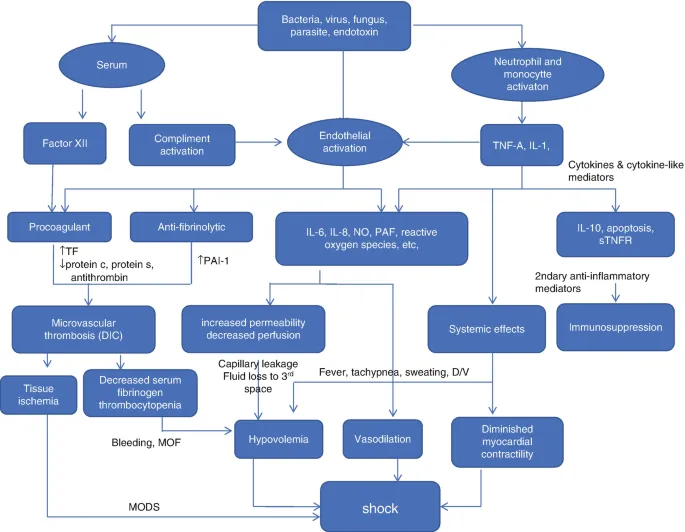
Cardiovascular Collapse - Pump & Pipes Problem
- Multifactorial Shock: Primarily a combination of distributive and hypovolemic shock.
- Hypovolemia ("Leaky Pipes"):
- Massive third-spacing of fluid into the retroperitoneum and peritoneal cavity due to ↑ capillary permeability.
- Leads to significant intravascular volume depletion, ↓ preload, and hemoconcentration (↑ hematocrit).
- Vasodilation ("Wide Pipes"):
- Systemic Inflammatory Response Syndrome (SIRS) triggers widespread release of inflammatory mediators (e.g., nitric oxide).
- Causes a sharp ↓ in Systemic Vascular Resistance (SVR).
- Myocardial Depression ("Pump Failure"):
- Circulating pancreatic enzymes (trypsin) and cytokines (TNF-α, IL-6) can directly suppress cardiac contractility.
- Hypovolemia ("Leaky Pipes"):
⭐ Early, aggressive intravenous fluid resuscitation is critical to manage the profound hypovolemia and prevent progression to organ failure.
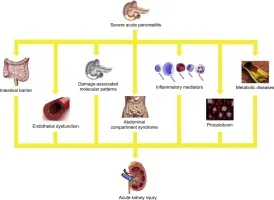
Renal & Metabolic Mayhem - Filters & Fuels Falter
- Acute Kidney Injury (AKI): Occurs in 20-40% of severe cases. Initially prerenal azotemia from profound hypovolemia (third-spacing, vomiting). Can progress to intrinsic AKI (Acute Tubular Necrosis) from hypotension and inflammatory mediators.
- Metabolic Derangements:
- Hypocalcemia: Fat necrosis consumes calcium via saponification. A key marker of severity.
- Hyperglycemia: Due to damage to β-cells in the islets of Langerhans, leading to ↓ insulin and ↑ glucagon.
- Hypomagnesemia: Often accompanies hypocalcemia.
⭐ Saponification-the binding of calcium to necrotic fat-is a hallmark of severe pancreatitis. A serum calcium <8.0 mg/dL is a poor prognostic indicator per Ranson's criteria.
High‑Yield Points - ⚡ Biggest Takeaways
- ARDS is the most common cause of death, presenting with refractory hypoxemia.
- Hypocalcemia from fat saponification is a classic sign of severity.
- Pleural effusion, typically left-sided and exudative, is a frequent pulmonary finding.
- Acute kidney injury (AKI) can develop from profound hypovolemia and hypotension.
- Disseminated intravascular coagulation (DIC) is a rare but lethal hematologic complication.
- Hyperglycemia and hypoalbuminemia are common metabolic derangements.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

