Initial Rx - First Moves Matter
- IV Fluids (Most Critical Step): Aggressive hydration is paramount.
- Solution: Lactated Ringer's is preferred; may reduce SIRS.
- Rate: Bolus of 15-20 mL/kg, then 3 mL/kg/hr (or 5-10 mL/kg/hr).
- Goal: ↓ BUN, urine output >0.5 mL/kg/hr.
- Analgesia: IV opioids (e.g., hydromorphone, fentanyl) for severe pain.
- NPO (Nil Per Os): Bowel rest to limit pancreatic stimulation.
⭐ Prophylactic antibiotics are NOT recommended for patients with interstitial (uncomplicated) pancreatitis, regardless of severity. They do not prevent progression to infected necrosis.
Cause & Crisis - Why & How Bad?
-
Etiology: 📌 I GET SMASHED
- Idiopathic, Gallstones, Ethanol (most common)
- Trauma, Steroids, Mumps, Autoimmune
- Scorpion sting, Hypercalcemia/lipidemia, ERCP, Drugs
-
Severity Assessment: Triage tool to predict mortality & necrosis.
- SIRS Criteria: ≥2 indicates high risk (Temp <36/>38°C, HR >90, RR >20, WBC <4k/>12k).
- Lab Markers: ↑ BUN, ↑ Hematocrit (hemoconcentration), ↑ CRP are poor prognostic signs.
- Scoring: BISAP score is a simple bedside tool.
⭐ An increasing BUN during the first 24 hours is one of the strongest independent predictors of mortality.
Support & Sustenance - The Core Care Plan
- NPO (Nil Per Os): Initially rest the pancreas. Advance diet to low-fat solids as pain and nausea resolve; no need for a clear liquid phase.
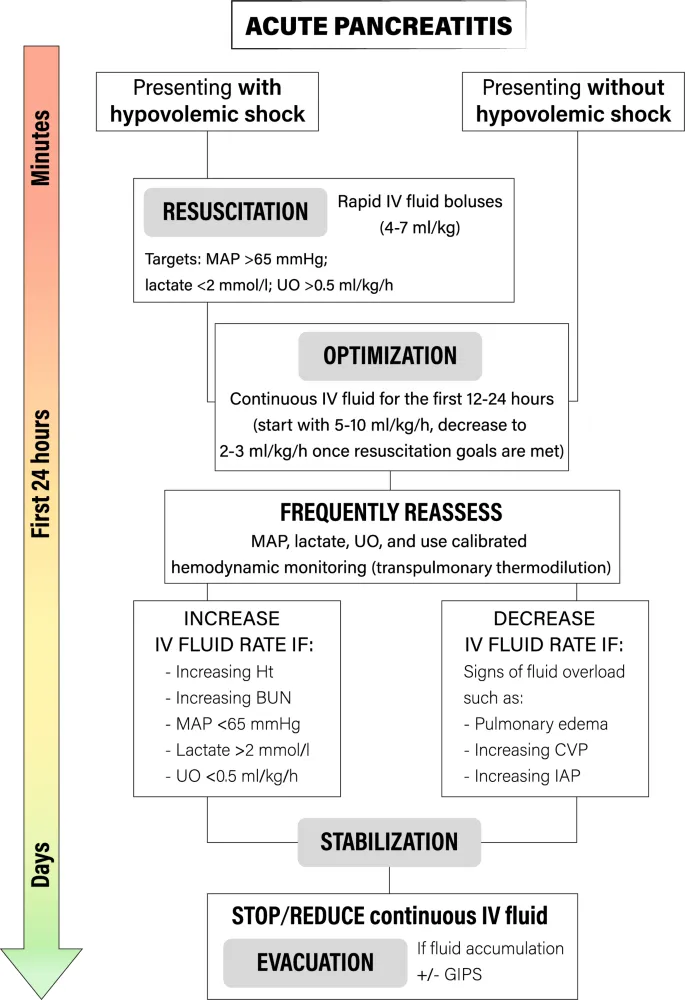
- IV Fluid Resuscitation: Crucial to prevent necrosis.
- Aggressive hydration: 5-10 mL/kg/hr of isotonic crystalloid solution.
- Lactated Ringer's is preferred.
- Goal: ↓ BUN & hematocrit, urine output > 0.5 mL/kg/hr.
- Analgesia: IV opioids (e.g., hydromorphone, fentanyl) are mainstays for severe pain.
- Nutritional Support:
- If unable to tolerate oral diet by day 3-5, start enteral nutrition.
- Nasogastric or nasojejunal routes are both effective.
⭐ High-Yield: Lactated Ringer's is superior to Normal Saline as it may reduce the incidence of Systemic Inflammatory Response Syndrome (SIRS).
Complications - When Things Go Wrong
-
Local Complications
- Pancreatic Pseudocyst: Encapsulated fluid collection developing >4 weeks after acute pancreatitis. Often asymptomatic. Intervene (drainage) only if symptomatic, infected, or >6 cm and persistent.
- Pancreatic Necrosis: Most severe local complication. Can be sterile or infected.
-
Systemic Complications
- ARDS, pleural effusion (often left-sided), atelectasis
- Hypocalcemia (from fat saponification), hyperglycemia
- Acute kidney injury
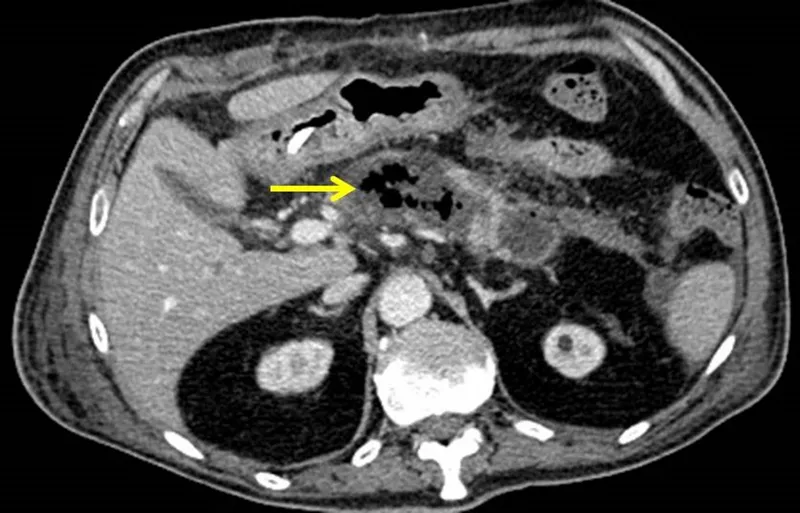
⭐ Infected necrosis is the primary driver of mortality. Gas bubbles on a CT scan are pathognomonic for infection by gas-forming organisms and mandate urgent intervention.
- Aggressive IV hydration is the most crucial initial step to prevent pancreatic necrosis.
- Pain management with IV opioids is a priority.
- Start enteral nutrition early if oral intake is not tolerated; avoid TPN.
- Prophylactic antibiotics are not recommended; use for confirmed infected necrosis only.
- ERCP is indicated within 24-48 hours for severe gallstone pancreatitis with cholangitis.
- Monitor closely for systemic complications like ARDS, hypocalcemia, and renal failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

