Top Causes - Stones & Spirits
The two most common causes account for ~80% of acute pancreatitis cases in the U.S.
| Feature | Gallstones (Cholelithiasis) | Alcohol |
|---|---|---|
| Pathophysiology | Ampullary obstruction by a stone → reflux of bile and/or duodenal contents into the pancreatic duct → premature enzyme activation. | Direct toxic effect on pancreatic acinar cells + sensitization to other injuries. Chronic use leads to protein plug formation. |
| Patient Profile | Classically, female, overweight, and >40 years old ("fat, female, forty"). Presents with acute, severe epigastric pain. | History of chronic, heavy alcohol use (typically >5-7 years). Often presents as an acute-on-chronic episode. |
⭐ An Alanine Aminotransferase (ALT) level >150 U/L has a >95% positive predictive value for gallstone pancreatitis.
Other Causes - The Usual Suspects
📌 Mnemonic: I GET SMASHED
- Idiopathic: No cause found after initial workup.
- Gallstones: (Covered previously)
- Ethanol (Alcohol): (Covered previously)
- Trauma: Blunt or penetrating abdominal injury; iatrogenic (e.g., post-operative).
- Steroids: High-dose corticosteroid therapy.
- Mumps: And other viruses (Coxsackie B, HIV).
- Autoimmune: IgG4-related disease, SLE, IBD.
- Scorpion sting: Venom from species like Tityus trinitatis.
- Hyperlipidemia/Hypercalcemia:
- Triglycerides > 1000 mg/dL.
- Calcium > 12 mg/dL (e.g., from hyperparathyroidism).
- ERCP: Post-procedure inflammation (5-10% of cases).
- Drugs: Thiazides, furosemide, azathioprine, valproic acid, sulfonamides.
⭐ Exam Favorite: Drug-induced pancreatitis is often idiosyncratic and dose-independent. Always review the patient's medication list for common offenders like diuretics (thiazides, furosemide) and immunosuppressants (azathioprine).
Pathophysiology - The Cascade Crash
- Core Defect: Premature activation of trypsinogen to trypsin within acinar cells, instead of the duodenal lumen.
- Mechanism: An initial insult (e.g., obstruction, toxins) disrupts normal acinar cell secretion and protective mechanisms.
- Autodigestion: Activated trypsin triggers a cascade, activating other zymogens:
- Elastase → vascular damage & hemorrhage.
- Phospholipase A2 → membrane destruction & coagulative necrosis.
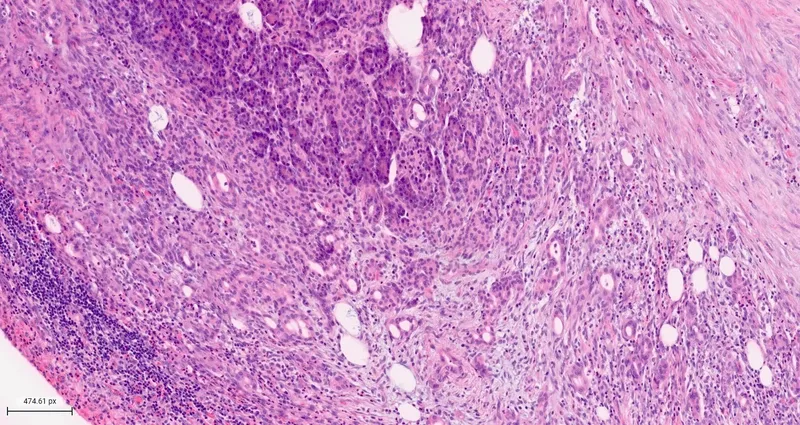
⭐ Trypsin is the key trigger. It not only digests pancreatic tissue but also activates the complement and kinin systems, amplifying inflammation and vascular permeability, leading to systemic complications.
High‑Yield Points - ⚡ Biggest Takeaways
- Gallstones and chronic alcohol abuse are overwhelmingly the most common causes of acute pancreatitis.
- Post-ERCP pancreatitis is the most frequent iatrogenic cause.
- Severe hypertriglyceridemia (TGs >1000 mg/dL) is a key metabolic trigger.
- Important drug-induced causes include diuretics, valproic acid, and azathioprine.
- Mumps virus is a classic infectious cause, especially in children.
- Autoimmune (IgG4-related) and idiopathic causes are considered after ruling out common etiologies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

