Etiology - Pancreas on Fire
📌 I GET SMASHED
- Idiopathic
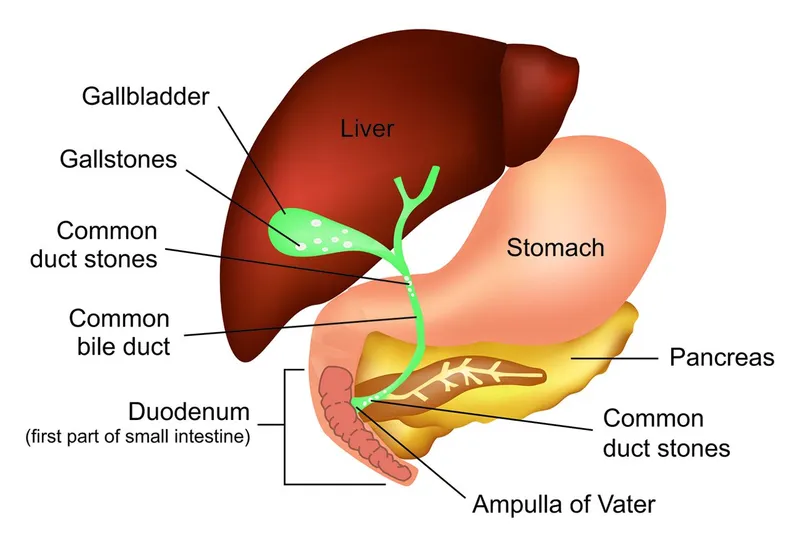
- Gallstones (commonest)
- Ethanol (2nd commonest)
- Trauma
- Steroids
- Mumps/Malignancy
- Autoimmune
- Scorpion sting
- Hyperlipidemia/Hypercalcemia
- ERCP
- Drugs (e.g., Azathioprine, Diuretics)
⭐ Gallstones and alcohol abuse account for >70% of acute pancreatitis cases. Severe hypertriglyceridemia (>1000 mg/dL) is another classic, albeit less common, cause.
Clinical Features - Belly Ache Drama
- Primary Symptom: Acute, severe, persistent epigastric pain.
- Radiation: Often "bores" straight through to the back.
- Relief: Sitting up and leaning forward.
- Aggravation: Lying supine, eating.
- Associated Features: Nausea, vomiting (which doesn't relieve the pain), anorexia.
- On Examination:
- Local: Epigastric tenderness, guarding, diminished bowel sounds.
- Systemic: Fever, tachycardia, hypotension (SIRS).
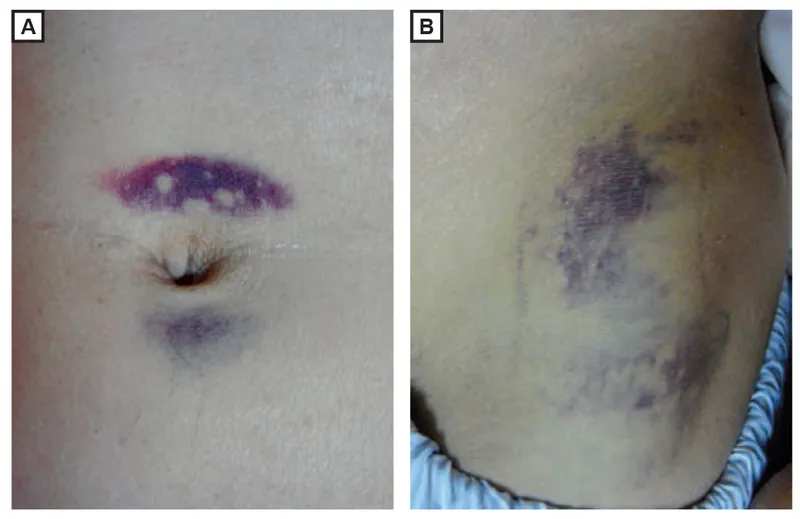
⭐ Ominous Signs: Cullen's (periumbilical) & Grey Turner's (flank) signs suggest retroperitoneal hemorrhage from severe necrotizing pancreatitis.
Diagnostic Criteria - The Detective's Toolkit
- Diagnosis requires 2 of 3 of the revised Atlanta criteria:
- Clinical Presentation: Acute onset of persistent, severe, epigastric abdominal pain, often radiating to the back.
- Laboratory Findings: Serum lipase or amylase elevation ≥3 times the upper limit of normal.
- 💡 Lipase is preferred due to higher specificity and longer half-life.
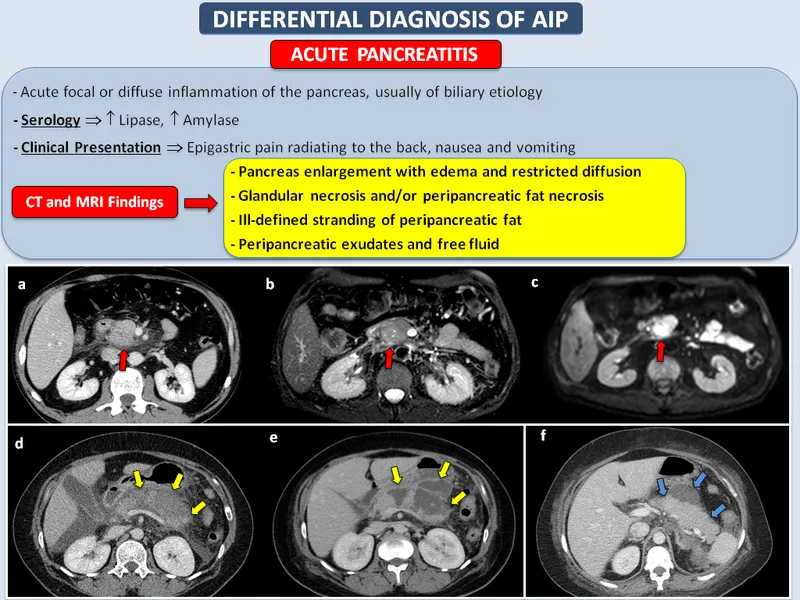
- Imaging Findings: Characteristic findings on contrast-enhanced CT (CECT), MRI, or transabdominal ultrasound.
⭐ If characteristic abdominal pain is present along with a lipase/amylase level ≥3x the upper limit of normal, imaging is not required to confirm the diagnosis.
Severity Scoring - Counting the Damage
- BISAP Score: Simpler bedside tool. Score ≥3 suggests severe disease & ↑ mortality.
- BUN >25 mg/dL
- Impaired mental status (GCS <15)
- SIRS criteria met
- Age >60 years
- Pleural effusion on imaging
- Ranson's Criteria: Classic but cumbersome (needs 48h data). Score ≥3 indicates severity.
- APACHE II: General ICU severity score, not specific to pancreatitis but accurate.
- CT Severity Index (Balthazar): Best performed >72 hours after onset to assess for necrosis.
⭐ A BISAP score of 0 is associated with <1% mortality, making it excellent for ruling out severe pancreatitis early on the floor.
High‑Yield Points - ⚡ Biggest Takeaways
- Diagnosis requires 2 of 3 criteria: acute epigastric pain radiating to the back, lipase or amylase ≥3x the upper limit of normal, or characteristic imaging findings.
- Lipase is more specific and sensitive than amylase; it remains elevated longer.
- Abdominal ultrasound is the best initial imaging test to identify gallstones as the cause.
- Contrast-enhanced CT is the gold standard for detecting complications like necrosis, not for initial diagnosis.
- Ranson's criteria and APACHE II scores are for assessing prognosis and severity, not for diagnosis.
- Hypocalcemia is a poor prognostic indicator resulting from fat saponification.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

