Nephrotic vs. Nephritic - Syndrome Showdown
| Feature | NephrOtic Syndrome | NephrItic Syndrome |
|---|---|---|
| Pathophysiology | Podocyte damage → ↑ protein leakage | Inflammation → glomerular damage |
| Proteinuria | Massive: >3.5 g/day | Mild-moderate: <3.5 g/day |
| Urine | Frothy urine, oval fat bodies | Hematuria, RBC casts (cola-colored) |
| Key Signs | Pitting edema, ascites, hyperlipidemia | Hypertension, oliguria, azotemia |
| Mnemonic | 📌 NOPHROTIC: Protein, Oedema | 📌 PHAROH: Proteinuria, Hematuria, Azotemia, RBC casts, Oliguria, Hypertension |
⭐ RBC casts are pathognomonic for glomerulonephritis, a hallmark of nephritic syndrome. They indicate glomerular bleeding.
Primary Nephrotic Diseases - Leaky Filters Club
-
Pathophysiology: Podocyte damage → ↑ glomerular permeability → massive proteinuria (>3.5 g/day), hypoalbuminemia, edema, hyperlipidemia.
-
Minimal Change Disease (MCD)
- Most common in children.
- Triggers: Idiopathic, NSAIDs, viral URI.
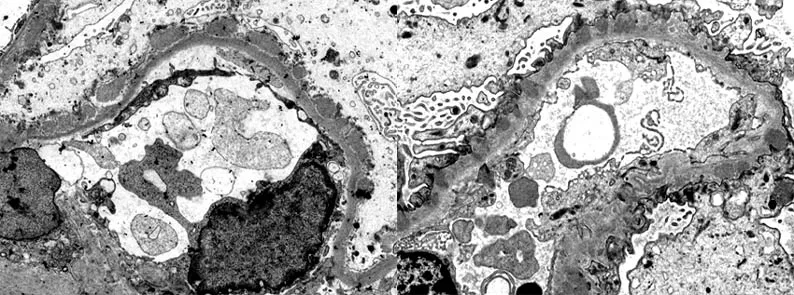
- Biopsy: Normal on light microscopy; EM shows effacement of podocyte foot processes.
- Treatment: Excellent response to corticosteroids.
-
Focal Segmental Glomerulosclerosis (FSGS)
- Most common cause in adults (esp. African American, Hispanic).
- Associations: HIV, heroin use, sickle cell disease, obesity.
- Biopsy: Sclerosis in parts (focal) of some (segmental) glomeruli.
-
Membranous Nephropathy
- 📌 Membranous: Malignancy (solid tumors), Medications (NSAIDs), anti-PLA2R Abs.
- Biopsy: LM shows thickened glomerular basement membrane. IF shows granular deposits.
⭐ Primary (Idiopathic) Membranous Nephropathy is most commonly associated with circulating antibodies to the phospholipase A2 receptor (PLA2R) on podocytes.
Primary Nephritic Diseases - Inflamed Filters Fight
- Post-Streptococcal Glomerulonephritis (PSGN):
- 2-4 weeks post-Group A Strep (pharyngitis/impetigo).
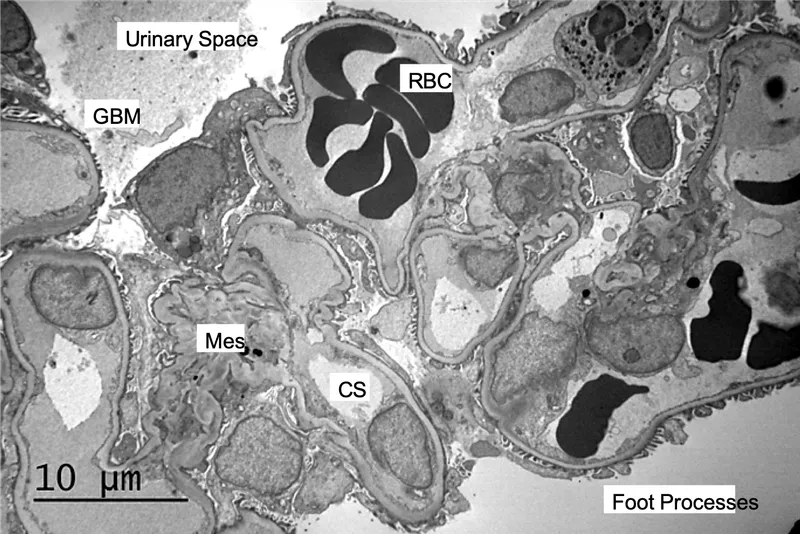
- LM: Hypercellular glomeruli. IF: Granular "lumpy-bumpy" IgG, C3. EM: Subepithelial humps.
- Presents with edema, hematuria, HTN. Low serum C3.
- IgA Nephropathy (Berger Disease):
- Most common primary GN worldwide. 📌 Berger's = Bloody urine after Bug (URI/GI).
- LM/IF: Mesangial IgA deposits & proliferation.
- Rapidly Progressive Glomerulonephritis (RPGN):
- Clinical syndrome: rapid loss of renal function.
- Histo: Crescent formation in Bowman's space.
⭐ Henoch-Schönlein purpura (HSP) is a systemic form of IgA nephropathy, presenting with a classic tetrad of palpable purpura, arthritis, abdominal pain, and renal disease.
Diagnostic Approach - Glomerular Roadmap
- Initial Clues: Urinalysis (hematuria, proteinuria) & urine microscopy (casts).
- Key Branching Point: Quantify proteinuria to distinguish syndromes.
- Nephritic: < 3.5 g/day, RBC casts, HTN, azotemia.
- Nephrotic: > 3.5 g/day, fatty casts, severe edema, HLD, hypoalbuminemia.
- Etiology Search: Serologies (Complements, ANA, ANCA, anti-GBM, ASO).
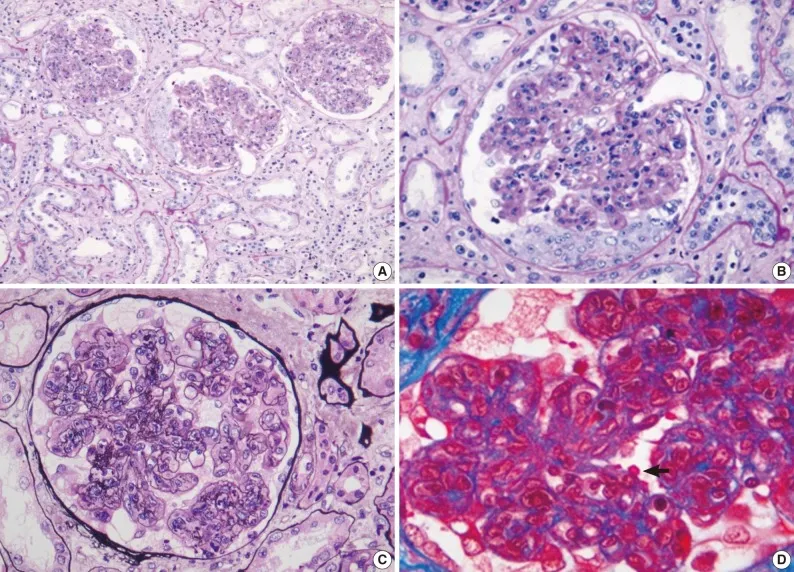
- Gold Standard: Kidney Biopsy (Light, Immunofluorescence, & Electron Microscopy).
⭐ RBC casts are pathognomonic for glomerulonephritis. In nephrotic syndrome, severe hypoalbuminemia (e.g., < 2.5 g/dL) leads to ↓ plasma oncotic pressure, causing massive edema.
High‑Yield Points - ⚡ Biggest Takeaways
- Minimal Change Disease: Top nephrotic cause in children; podocyte effacement with dramatic steroid response.
- FSGS: Leading nephrotic cause in African Americans; linked to HIV, sickle cell, and heroin use.
- Membranous Nephropathy: Common in adults; defined by anti-PLA2R antibodies and "spike-and-dome" appearance.
- IgA Nephropathy: Most common GN worldwide; presents with gross hematuria concurrently with a URI.
- Post-streptococcal GN: Occurs 1-3 weeks post-infection; marked by low C3 and subepithelial "humps".
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

