Pathophysiology - Pressure Cooker Kidneys
- Chronic systemic hypertension transmits excessive pressure to unprotected renal arterioles, especially the afferent arteriole.
- This leads to endothelial injury and leakage of plasma proteins into the vessel walls.
- Histology:
- Hyaline arteriolosclerosis: Homogeneous, pink, glassy thickening of arteriolar walls.
- Fibroelastic hyperplasia: "Onion-skinning" in larger vessels (seen in malignant HTN).
⭐ The earliest and most significant vascular changes occur in the afferent arterioles, as they are not well-protected from high systemic pressures.
Clinical Presentation & Diagnosis - The Silent Saboteur
- Insidious Onset: Often asymptomatic for years; typically discovered incidentally on routine labs.
- Hallmark: Long-standing, poorly controlled hypertension (often >10-15 years).
- Associated Findings:
- Signs of hypertensive end-organ damage:
- Left Ventricular Hypertrophy (LVH).
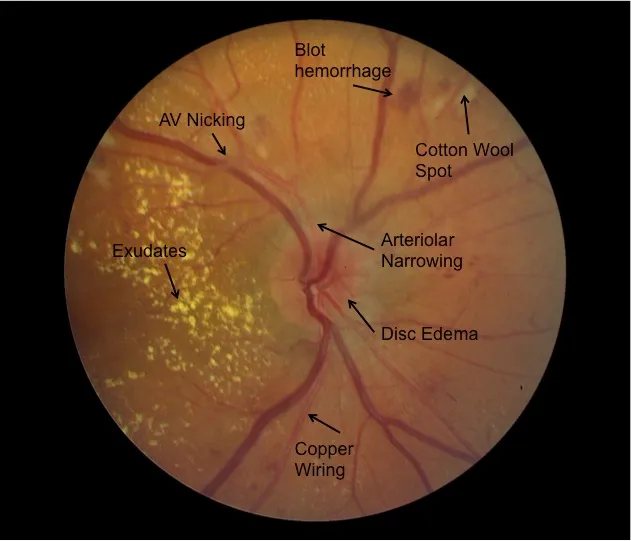
- Hypertensive retinopathy (AV nicking, copper wiring).
- Slowly progressive ↑ serum creatinine & ↓ GFR.
- Signs of hypertensive end-organ damage:
- Urinary Findings:
- Proteinuria: Mild (<1 g/day), non-nephrotic.
- Urinalysis: Bland sediment, few hyaline casts.
- Imaging:
- Ultrasound: Normal or symmetrically small, echogenic kidneys.
- Diagnosis of Exclusion: Must rule out other primary kidney diseases.
⭐ Kidney biopsy, rarely performed, classically shows hyaline arteriolosclerosis of afferent arterioles and fibroelastic hyperplasia of interlobular arteries.
Histopathology - Microscopic Mayhem
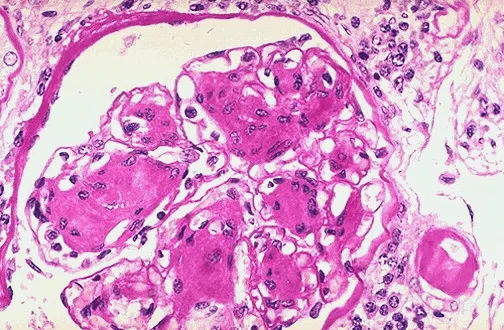
-
Vascular Changes (Arterionephrosclerosis)
- Hyaline arteriolosclerosis: Eosinophilic, homogenous thickening of small arteries & arterioles (especially afferent), leading to luminal narrowing.
- Fibroelastic hyperplasia: Intimal thickening in larger interlobular and arcuate arteries.
-
Glomerular Ischemia
- Wrinkling and thickening of capillary basement membranes.
- Progressive collapse of the glomerular tuft, leading to focal or global glomerulosclerosis.
-
Tubulointerstitial Damage
- Patchy tubular atrophy and interstitial fibrosis secondary to chronic ischemia.
⭐ In contrast, malignant hypertension features hyperplastic arteriolosclerosis (“onion-skinning”) and fibrinoid necrosis of arterioles, indicating acute, severe endothelial injury.
Management - Pressure Under Control
-
Primary Goal: Aggressive blood pressure control to slow CKD progression.
-
Target: BP < 130/80 mmHg. For patients with proteinuria >300 mg/day, a target of < 120/80 mmHg may be considered.
-
First-line Therapy: ACE inhibitors (e.g., Lisinopril) or ARBs (e.g., Losartan).
- These agents reduce systemic BP and preferentially dilate the efferent arteriole, ↓ intraglomerular pressure and ↓ proteinuria.
-
Second-line Agents:
- Thiazide diuretics (e.g., Hydrochlorothiazide) or Calcium Channel Blockers (e.g., Amlodipine) are added if BP remains above target.
⭐ ACE inhibitors and ARBs are the cornerstone of therapy, not just for BP control, but for their direct renoprotective effects by reducing glomerular hypertension.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by chronic, poorly controlled hypertension, leading to progressive renal damage.
- A major cause of end-stage renal disease (ESRD), especially in African Americans.
- Key pathology includes hyaline arteriolosclerosis of small arteries and focal global glomerulosclerosis.
- Kidneys are typically symmetrically small and shrunken with a granular surface.
- Urinalysis is often bland with absent or mild proteinuria (<1 g/day).
- Treatment is centered on strict blood pressure control, with ACE inhibitors or ARBs as first-line agents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

