Portal Hypertension - The Pressure Cooker
- Pathophysiology: Results from ↑ resistance to portal blood flow (primarily intra-hepatic) and ↑ splanchnic circulation, leading to a back-up of pressure.
- Etiologies:
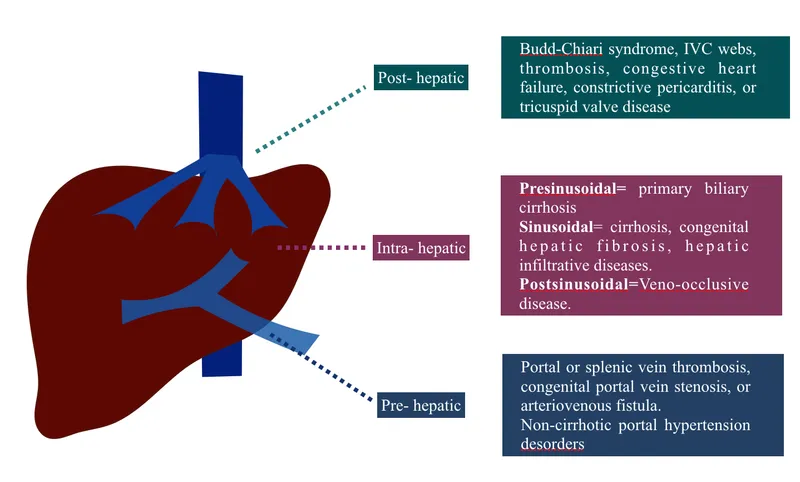
- Pre-hepatic: Portal/splenic vein thrombosis.
- Intra-hepatic: Cirrhosis, schistosomiasis, sarcoidosis.
- Post-hepatic: Budd-Chiari syndrome, right heart failure.
- Measurement: Hepatic Venous Pressure Gradient (HVPG).
- $HVPG = \text{Wedged Hepatic Vein Pressure} - \text{Free Hepatic Vein Pressure}$
- Thresholds: Varices develop at >10 mmHg; bleeding risk at >12 mmHg.
⭐ The most common cause of portal hypertension in the Western world is cirrhosis.
Variceal Hemorrhage - Leaky Volcanoes
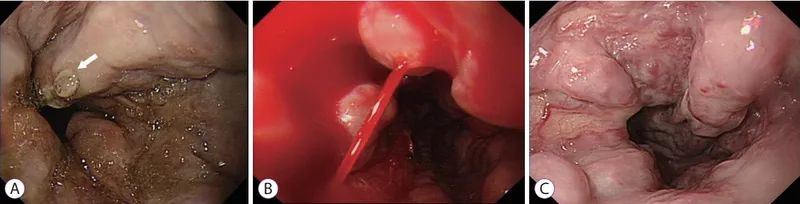
⭐ All patients with newly diagnosed cirrhosis require an upper endoscopy (EGD) to screen for esophageal varices.
- Primary Prophylaxis: For medium-to-large varices, prevent the first bleed using non-selective β-blockers (NSBB) like propranolol, or via Endoscopic Variceal Ligation (EVL).
- Acute Bleed Management: A medical emergency. Transfuse for Hb <7 g/dL.
- Secondary Prophylaxis: To prevent re-bleeding, combine NSBB with serial EVL. A Transjugular Intrahepatic Portosystemic Shunt (TIPS) is considered for refractory cases.
Ascites & SBP - Leaky Pipes, Bad Bugs
- Pathophysiology: Splanchnic vasodilation & RAAS activation → Na⁺/H₂O retention.
- Diagnosis: Paracentesis is key. Calculate Serum-Ascites Albumin Gradient.
- $SAAG = Serum Albumin - Ascites Albumin$. A value >1.1 g/dL suggests portal hypertension.
⭐ A SAAG > 1.1 g/dL is 97% accurate for diagnosing ascites due to portal hypertension.
- Spontaneous Bacterial Peritonitis (SBP): Infection of ascitic fluid.
- Diagnosis: Ascitic fluid PMNs >250/mm³.
- Organisms: E. coli, Klebsiella, Pneumococci.
- Treatment: 3rd-generation cephalosporins (e.g., ceftriaxone).
Hepatic Encephalopathy - Brain Fog Central
-
Pathophysiology: ↑ Ammonia ($NH_3$) neurotoxicity from impaired hepatic clearance.
-
Symptoms & Staging:
- Early: Altered sleep, ↓ attention.
- Late: Confusion, lethargy, coma.
- Asterixis: Classic flapping tremor.
- Staged by West Haven Criteria.
-
Precipitants:
- 📌 HE-PRECIPITANTS: Hemorrhage, Electrolytes, Protein, Renal failure, ETOH, Constipation, Infection, Portosystemic shunt.
-
Treatment:
- Lactulose: ↓ $NH_3$ production/absorption.
- Rifaximin: ↓ $NH_3$-producing bacteria.
⭐ The first step in managing hepatic encephalopathy is to identify and correct the precipitating factor(s).
Hepatorenal Syndrome - Kidney Shutdown
- Pathophysiology: Splanchnic vasodilation from portal hypertension → ↓ systemic resistance → RAAS activation → severe renal vasoconstriction → ↓ GFR.
- Diagnosis & Types: A diagnosis of exclusion (no shock, nephrotoxins, or intrinsic kidney disease).
- Type 1: Rapid, severe (Creatinine >2.5 mg/dL in <2 wks).
- Type 2: Insidious onset with refractory ascites.
- Treatment: Bridge to transplant with Albumin, Midodrine, and Octreotide. Definitive treatment is liver transplantation.
⭐ Hepatorenal syndrome is a functional renal failure; kidneys are histologically normal and can recover function after liver transplantation.
High‑Yield Points - ⚡ Biggest Takeaways
- Esophageal varices are the most lethal complication; use non-selective beta-blockers (nadolol, propranolol) for primary prophylaxis.
- Ascites stems from splanchnic vasodilation and RAAS activation; manage with spironolactone and furosemide.
- Suspect SBP with fever/pain; diagnose with ascitic fluid PMNs > 250 cells/mm³ and treat with third-gen cephalosporins.
- Hepatic encephalopathy presents with asterixis from ↑ ammonia; treat with lactulose and rifaximin.
- A serum-ascites albumin gradient (SAAG) ≥ 1.1 g/dL confirms portal hypertension-related ascites.
- Hepatorenal syndrome is acute renal failure; treat with albumin, octreotide, and midodrine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

