Pathophysiology - The Kidney Squeeze
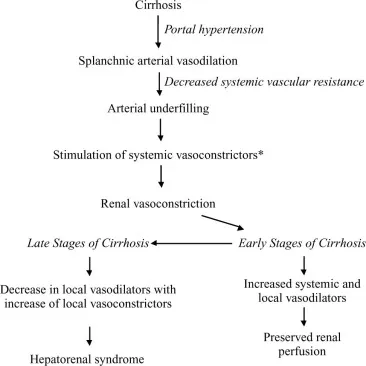
Underlying liver disease (e.g., cirrhosis) triggers a cascade that starves the kidneys of blood flow.
- Portal Hypertension: The primary driver.
- Splanchnic Vasodilation: Blood vessels in the gut widen, primarily due to ↑ Nitric Oxide (NO).
- This causes pooling of blood in the splanchnic circulation.
- ↓ Effective Arterial Volume: The rest of the body, including the kidneys, perceives a state of severe volume depletion.
- Compensatory Activation: The body over-responds:
- Activation of Renin-Angiotensin-Aldosterone System (RAAS).
- Activation of the Sympathetic Nervous System.
- Intense Renal Vasoconstriction: The result is a "squeeze" on the kidney's arteries, leading to ↓ renal perfusion and a sharp ↓ in GFR.
⭐ Despite profound azotemia, the kidneys in HRS are histologically normal and can function perfectly if transplanted into a person with a healthy liver.
Diagnosis & Criteria - The Exclusion Game
Diagnosis of HRS is based on the International Club of Ascites (ICA) criteria, a process of elimination.
-
Prerequisites: Cirrhosis with ascites and Acute Kidney Injury (AKI).
- AKI is defined as an increase in serum creatinine (SCr) by ≥0.3 mg/dL within 48 hours OR a ≥50% increase from a stable baseline.
-
Exclusion Criteria (No other reason for AKI):
- No hypovolemic shock.
- No current or recent use of nephrotoxic drugs.
- No evidence of structural kidney damage (parenchymal disease):
- Proteinuria <500 mg/day.
- No significant hematuria (<50 RBCs/HPF).
- Normal renal ultrasound.
-
Therapeutic Challenge Failure:
- No improvement in renal function after at least 2 days of diuretic withdrawal AND volume expansion with albumin (dose: 1 g/kg of body weight per day).
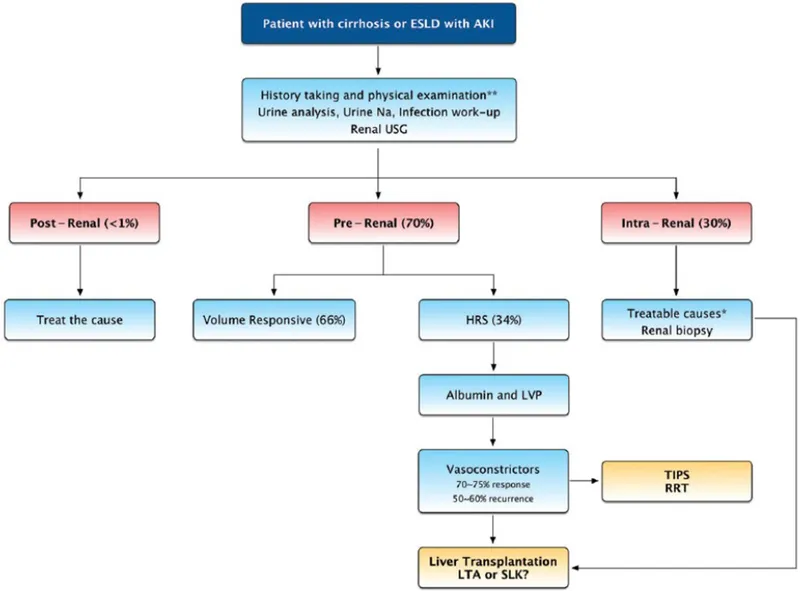
⭐ The diagnosis of HRS is one of exclusion; you must first rule out other causes of acute kidney injury, particularly prerenal azotemia, by administering an albumin challenge.
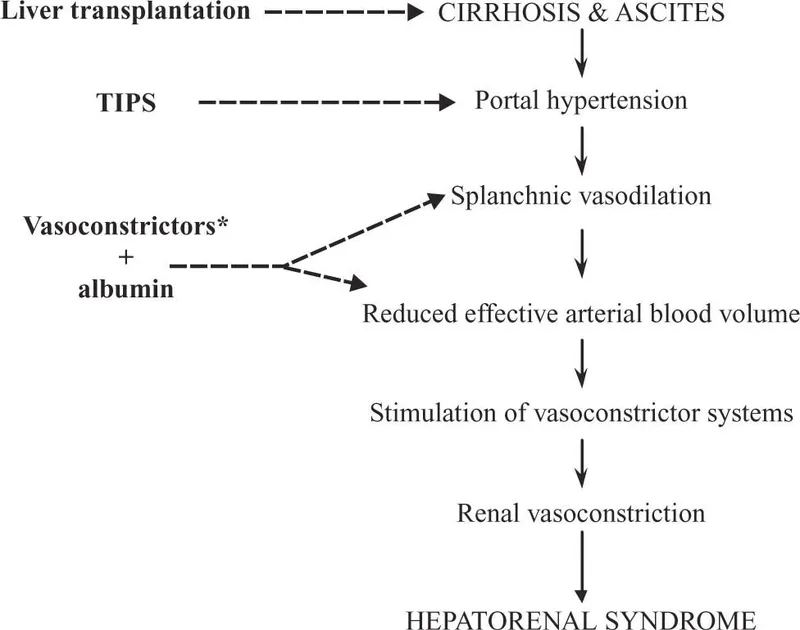
Management - Reversing the Clamp
Primary goal: Reverse splanchnic vasodilation and renal vasoconstriction.
-
Pharmacologic Therapy (Bridge to Transplant)
- Albumin: Crucial for volume expansion and binding vasodilators. Give 1 g/kg on day 1, then 25-50 g/day.
- PLUS Vasoconstrictors:
- Terlipressin: A vasopressin analog; preferred agent.
- Midodrine + Octreotide: Alternative regimen.
-
Definitive & Bridging Therapy
- Liver Transplantation: The only definitive cure.
- TIPS: Can serve as a bridge to transplantation.
📌 TAM: Terlipressin/TIPS, Albumin, Midodrine+Octreotide.
⭐ Albumin is not just a volume expander here; it also binds and inactivates vasodilators and has anti-inflammatory effects, making it a critical component of HRS therapy.
- Hepatorenal syndrome (HRS) is functional renal failure that occurs in patients with advanced liver disease, particularly cirrhosis with ascites.
- The primary mechanism is intense renal vasoconstriction in response to severe splanchnic and systemic vasodilation.
- Common precipitants include spontaneous bacterial peritonitis (SBP), GI bleeding, and large-volume paracentesis.
- It's a diagnosis of exclusion; requires no response to diuretic withdrawal and an albumin challenge.
- Definitive treatment is liver transplantation; bridge therapy includes vasoconstrictors (midodrine, octreotide) and albumin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

