Pneumonia Types - Lungs Under Siege
- Community-Acquired (CAP): Acquired outside a hospital or within 48 hours of admission.
- Hospital-Acquired (HAP): Develops ≥48 hours after hospital admission.
- Ventilator-Associated (VAP): Arises >48 hours after endotracheal intubation.
- Clinical Syndromes:
- Typical: Sudden onset, high fever, purulent cough, lobar consolidation. Caused by typical organisms (S. pneumoniae).
- Atypical ("Walking"): Insidious onset, low-grade fever, non-productive cough, patchy infiltrates. Caused by atypical organisms (Mycoplasma, Chlamydia, Legionella).
⭐ Exam Favorite: Legionella pneumophila, an atypical cause, is classically associated with GI symptoms (diarrhea) and hyponatremia (low sodium).
Etiology - The Usual Suspects
| Pneumonia Type | Common Pathogens |
|---|---|
| CAP (Outpatient) | S. pneumoniae, Mycoplasma, H. influenzae, Viruses |
| CAP (Inpatient) | S. pneumoniae, H. influenzae, S. aureus, Legionella |
| HAP / VAP | Pseudomonas, S. aureus (MRSA), GNRs (Klebsiella, E. coli) |
- **Alcoholism:** *Klebsiella pneumoniae* (currant jelly sputum)
- **COPD/Smoking:** *H. influenzae*, *Pseudomonas*
- **Post-Influenza:** *S. aureus* (often MRSA)
- **Aspiration:** Oral anaerobes (e.g., *Peptostreptococcus*)
⭐ Pseudomonas aeruginosa is a critical pathogen in patients with structural lung diseases like cystic fibrosis or bronchiectasis, often requiring specific antibiotic coverage.
📌 Atypicals: 'My Legion of Clamoring Q-Ts' (Mycoplasma, Legionella, Chlamydophila, Coxiella)
Diagnosis & Severity - Spotting the Shadow
-
Clinical & Radiologic Dx:
- H&P: Fever, cough, dyspnea, crackles on auscultation.
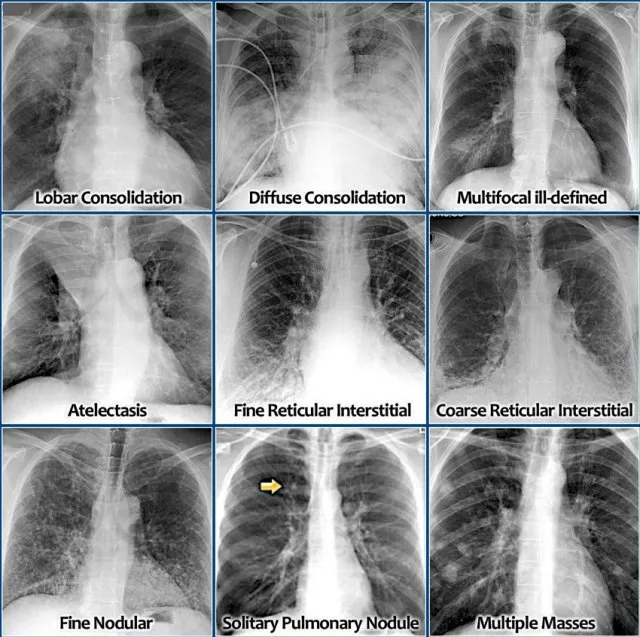
- Chest X-ray: Key to diagnosis. Look for:
- Lobar consolidation: Classic for S. pneumoniae.
- Interstitial infiltrates: Atypical pathogens (e.g., Mycoplasma).
- Cavities: S. aureus, anaerobes, TB.
- Labs: ↑ WBC; ↑ Procalcitonin suggests bacterial etiology.
-
Severity Scoring (CURB-65 for CAP):
- Confusion (new onset)
- Uremia (BUN > 20 mg/dL)
- Respiratory Rate (≥ 30 breaths/min)
- Blood Pressure (SBP < 90 or DBP ≤ 60 mmHg)
- Age (≥ 65 years)
- Disposition: 0-1 (Outpatient), 2 (Inpatient), ≥3 (ICU).
⭐ Procalcitonin is a specific marker for bacterial infections; levels >0.25 ng/mL strongly support bacterial pneumonia and guide antibiotic stewardship.
Treatment - The Antibiotic Arsenal
-
Community-Acquired Pneumonia (CAP): Empiric choice depends on severity.
-
Hospital-Acquired (HAP) / Ventilator-Associated (VAP): Cover MRSA & Pseudomonas.
- MRSA: Vancomycin or Linezolid.
- Anti-pseudomonal: Piperacillin-tazobactam, Cefepime, or a Carbapenem.
⭐ For CAP, empiric outpatient therapy must cover atypical pathogens. Standard beta-lactams alone are insufficient against Mycoplasma, Chlamydia, and Legionella.
High‑Yield Points - ⚡ Biggest Takeaways
- S. pneumoniae is the most common cause of Community-Acquired Pneumonia (CAP).
- Atypical pathogens like Mycoplasma cause "walking pneumonia," especially in young adults.
- Use the CURB-65 score to determine CAP severity and need for hospitalization.
- Hospital-Acquired Pneumonia (HAP) develops >48 hours post-admission; common culprits are Pseudomonas and MRSA.
- Legionella is linked to contaminated water and classically causes hyponatremia and GI symptoms.
- For severe pneumonia, obtain blood and sputum cultures before starting antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

