UC Pathophysiology - Guts Under Siege
- Immune-Mediated: Genetic predisposition (e.g., HLA-B27) + environmental triggers disrupt gut homeostasis.
- Barrier Dysfunction: Defective colonic epithelial barrier allows luminal antigens to penetrate the mucosa.
- Aberrant Immune Response: Predominantly a Th2-mediated response.
- Key cytokines: IL-5 and IL-13.
- IL-13 ↑ epithelial permeability and induces apoptosis.
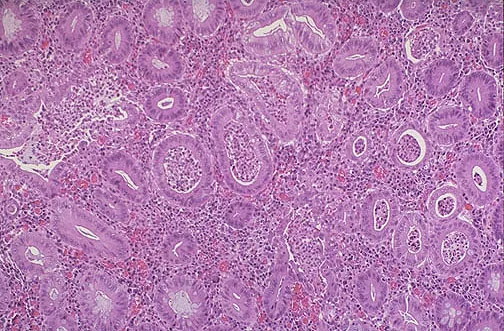
⭐ High-Yield: Approximately 60-70% of individuals with UC are positive for perinuclear anti-neutrophil cytoplasmic antibodies (p-ANCA), suggesting an autoimmune component.
The Blame Game - UC's Triggers
-
Multifactorial Hit: UC arises from a perfect storm of genetic susceptibility, a dysregulated immune response, and environmental insults targeting the colonic mucosa.
-
Genetic Blueprint:
- Polygenic; strong family association.
- Key loci involved in mucosal barrier function and immune recognition (e.g., HLA-B27).
-
Immune System on Overdrive:
- Aberrant, exaggerated response to gut microbiota.
- Primarily a Th2-mediated response.
- Key cytokines: ↑ IL-5, ↑ IL-13, leading to mucosal inflammation and damage.
-
Environmental Triggers:
- Infections (e.g., Salmonella, Campylobacter).
- Medications (NSAIDs can exacerbate).
- Diet: Western diet (↑ fats/sugars, ↓ fiber) implicated.
⭐ Smoking Paradox: Unlike in Crohn's disease, smoking is paradoxically protective in ulcerative colitis and cessation can trigger a flare.
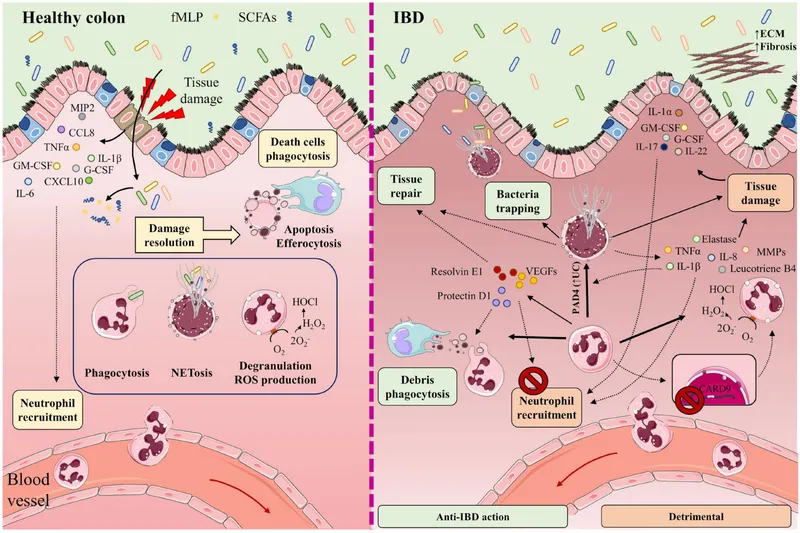
Immune Mayhem - The Attack Within
- Genetic Predisposition: Strong link to HLA-B27 and other susceptibility genes, leading to a dysfunctional immune response to gut microbiota.
- Barrier Dysfunction: Compromised epithelial tight junctions allow luminal bacteria to penetrate the mucosa, triggering inflammation.
- Atypical T-Cell Response: A key feature is a dominant Th2-mediated response (unlike Th1/Th17 in Crohn's).
- Produces cytokines like IL-5 and IL-13.
- IL-5 recruits eosinophils.
- IL-13 increases epithelial permeability and induces apoptosis.
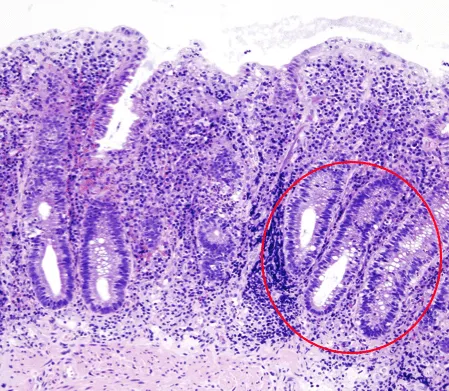
⭐ High-Yield: Positive Perinuclear Anti-Neutrophil Cytoplasmic Antibodies (p-ANCA) are found in ~70% of UC patients, contrasting with their lower prevalence in Crohn's disease.
Under the Scope - A Closer Look
- Immune Profile: Predominantly a Th2-mediated response with atypical T-cells.
- Key Mediator: ↑ production of IL-13, which compromises epithelial barrier integrity.
- Antibody Association: Often positive for perinuclear anti-neutrophil cytoplasmic antibodies (p-ANCA).
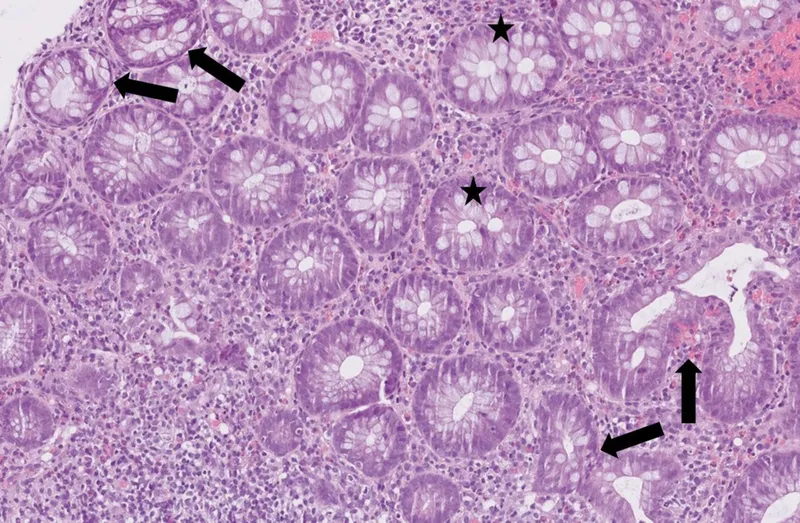
- Histological Hallmarks:
- Inflammation limited to mucosa & submucosa.
- Distorted crypt architecture & branching.
- Goblet cell depletion.
⭐ Exam Favorite: Unlike Crohn's, granulomas are absent. The presence of p-ANCA is seen in up to 70% of UC patients and is strongly associated with co-existing Primary Sclerosing Cholangitis (PSC).
High‑Yield Points - ⚡ Biggest Takeaways
- Ulcerative colitis is a diffuse mucosal and submucosal inflammation limited to the colon.
- It invariably involves the rectum and extends proximally in a continuous, circumferential pattern.
- Hallmark pathology includes crypt abscesses, distorted crypts, and depleted goblet cells.
- This is primarily a Th2-mediated immune response with atypical T-cells.
- Pseudopolyps form as islands of regenerating mucosa.
- Strongly associated with p-ANCA and Primary Sclerosing Cholangitis (PSC).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

