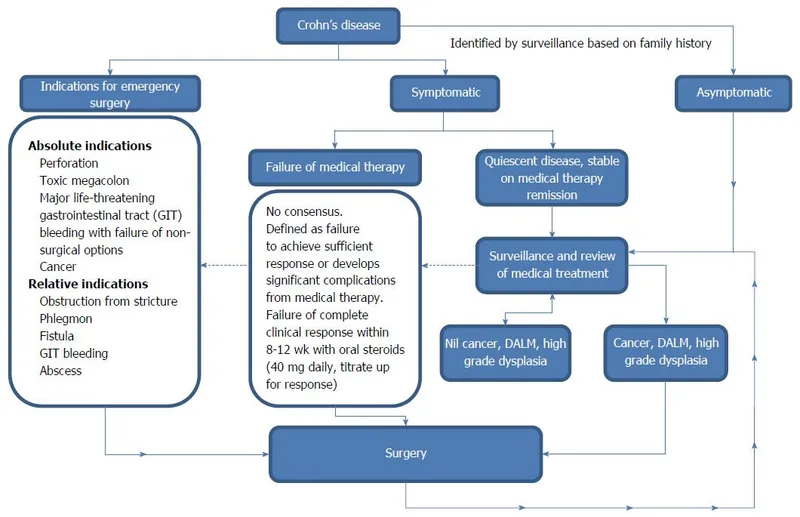
Indications for Surgery - The Cutting Edge
Ulcerative Colitis (UC) - Curative
- Emergent:
- Toxic megacolon (>6 cm colonic dilation + toxicity)
- Fulminant colitis, perforation, uncontrolled hemorrhage
- Elective:
- Medically refractory disease
- Dysplasia or colorectal cancer (CRC)
- Growth retardation in children
Crohn's Disease (CD) - Not Curative; for Complications
- Indications:
- Bowel obstruction from fibrotic strictures (most common)
- Intra-abdominal abscess
- Fistulae (e.g., enterovesical)
- Medically refractory disease
⭐ Smoking is the strongest modifiable risk factor for post-operative recurrence in Crohn's disease.
Ulcerative Colitis Surgery - The Curative Colectomy
- Unlike Crohn's, surgery is curative for UC, removing all diseased colonic and rectal mucosa.
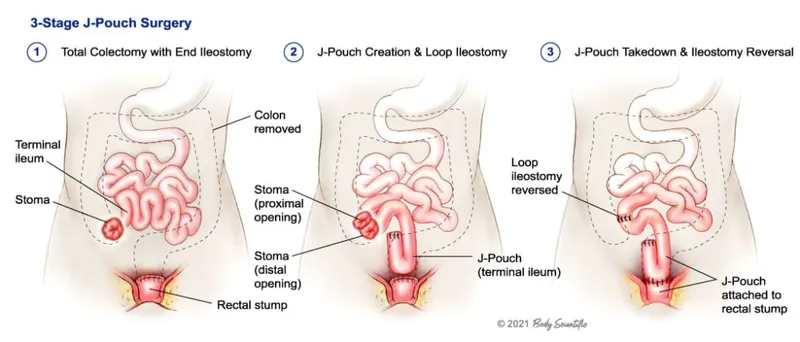
- Standard of Care: Total Proctocolectomy (TPC) with Ileal Pouch-Anal Anastomosis (IPAA).
- The ileal pouch (e.g., "J-pouch") acts as a neorectum.
- Avoids a permanent ileostomy, preserving continence.
- Typically performed in 2 or 3 stages, especially in acutely ill patients on high-dose steroids.
- Key Complications:
- Anastomotic leak, pelvic sepsis
- Pouchitis & Cuffitis
- Small Bowel Obstruction
- Reduced female fertility (due to pelvic adhesions)
⭐ Pouchitis is the most common long-term complication, affecting up to 50% of patients. It presents with ↑ stool frequency, urgency, and cramps. Treat with antibiotics (Metronidazole or Ciprofloxacin).
Crohn's Disease Surgery - Respect the Bowel
- Not Curative: Surgery manages complications, not the underlying disease. The core principle is bowel conservation.
- Primary Indications:
- Fibrotic strictures causing obstruction (most common)
- Intra-abdominal abscesses
- Fistulae (e.g., enterovesical, enterocutaneous)
- Refractory hemorrhage or free perforation
- Failure of maximal medical therapy
- Dysplasia or cancer
- Surgical Approaches:
- Strictureplasty: Widens narrowed segments without resection (e.g., Heineke-Mikulicz). Preserves bowel length.
- Limited Resection: Removal of only the grossly affected bowel segment.
⭐ Post-operative recurrence is high (~60% endoscopic recurrence at 1 year), most commonly occurring in the neoterminal ileum, just proximal to the anastomosis.
Post-Op Complications - The Aftermath
- Anastomotic Recurrence (Crohn's Disease)
- Common at the site of ileocolonic anastomosis.
- Presents with obstruction, fistulas, or abscesses.
- Requires surveillance endoscopy for early detection.
- Pouchitis & Cuffitis (UC after IPAA)
- Pouchitis: Inflammation of the ileal pouch. Presents with cramps, ↑ frequency, urgency.
- Tx: Metronidazole or Ciprofloxacin.
- Cuffitis: Inflammation of the residual rectal cuff.
- Pouchitis: Inflammation of the ileal pouch. Presents with cramps, ↑ frequency, urgency.
- General Surgical Risks
- Early: Anastomotic leak, sepsis, wound infection.
- Late: Adhesions (→ SBO), hernias, short bowel syndrome.
⭐ Pouchitis is the most common long-term complication after an IPAA for UC, affecting up to 50% of patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Surgery is curative in Ulcerative Colitis (total proctocolectomy) but palliative in Crohn's disease, which is reserved for complications.
- Urgent indications for UC surgery include toxic megacolon, perforation, or massive hemorrhage; elective reasons include dysplasia or refractory disease.
- Crohn's surgery addresses strictures, fistulas, and abscesses. The most common procedure is an ileocecal resection.
- Total proctocolectomy with IPAA is the standard restorative surgery for UC.
- Pouchitis is a common complication of IPAA.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

