Pathophysiology - From Gut Fire to Cancer
- Chronic Inflammation: The primary driver. Persistent inflammation with high levels of pro-inflammatory cytokines (TNF-α, IL-6) and reactive oxygen species (ROS) causes continuous mucosal injury and repair.
- Genetic Instability: This leads to oxidative DNA damage, promoting an "inflammation-dysplasia-carcinoma" sequence.
- Key mutation: p53 inactivation is a critical, early event.
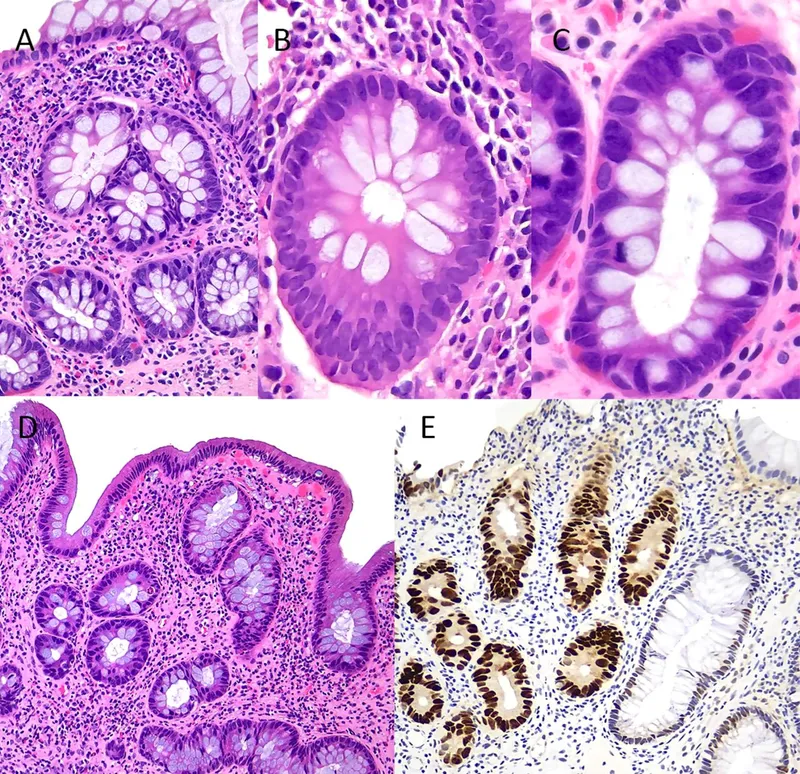
⭐ In contrast to sporadic CRC, IBD-associated cancer arises from flat, invisible dysplasia and p53 mutations occur early in the process.
Risk Factors - The Usual Suspects
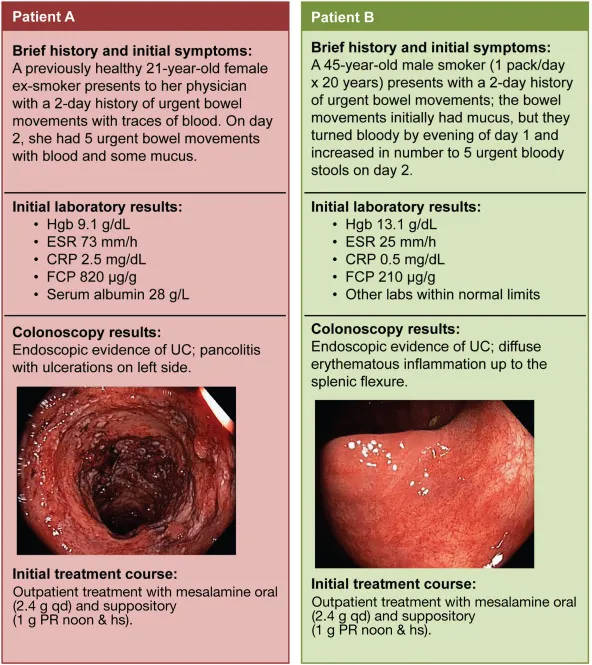
- Disease Duration & Extent: Risk ↑ significantly after 8-10 years of colitis. Pancolitis carries a much higher risk than left-sided colitis or proctitis.
- Severity of Inflammation: Greater histologic and endoscopic inflammation correlates with ↑ cancer risk.
- Primary Sclerosing Cholangitis (PSC): A strong, independent risk factor for both cholangiocarcinoma and colorectal cancer (CRC).
- Family History: First-degree relative with CRC, especially if diagnosed at < 50 years old.
- Anatomic Factors: Presence of strictures or previous finding of dysplasia.
⭐ Patients with IBD and concomitant PSC have a very high CRC risk; surveillance colonoscopy should begin at the time of PSC diagnosis, regardless of colitis duration.
Surveillance Strategy - The Watchful Scope
- Initiation: Begin surveillance colonoscopy 8-10 years after diagnosis of pancolitis, or 12-15 years for left-sided disease.
- Frequency: Every 1-3 years, based on risk stratification (e.g., family history, severity, PSC).
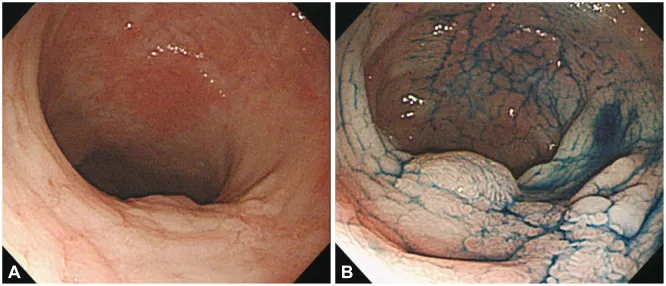
- Procedure: High-definition colonoscopy, ideally with chromoendoscopy (dye spray) to enhance visualization.
- Biopsy Protocol: Random 4-quadrant biopsies every 10 cm, plus targeted biopsies of any suspicious lesions.
⭐ For patients with co-existing Primary Sclerosing Cholangitis (PSC), start annual surveillance immediately upon PSC diagnosis due to markedly ↑ CRC risk.
Dysplasia Management Flow
Dysplasia Management - Nipping Trouble in the Bud
Management hinges on whether dysplasia is endoscopically visible and resectable.
- Invisible Dysplasia (Flat/Non-polypoid):
- Difficult to completely remove endoscopically.
- High risk for synchronous or metachronous cancer.
- Action: Proctocolectomy is the standard of care.
- **Visible Dysplasia (Polypoid):
- Endoscopically Resectable: Complete removal (polypectomy) is possible.
- Follow-up with surveillance colonoscopy in 3-6 months.
- Non-resectable: Treat as invisible dysplasia → Colectomy.
- Endoscopically Resectable: Complete removal (polypectomy) is possible.
⭐ Any dysplasia found in a patient with IBD implies a "field defect," indicating widespread genetic instability in the colonic mucosa, significantly ↑ risk for CRC elsewhere in the colon.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic inflammation is the primary driver of dysplasia and colorectal cancer (CRC) in IBD.
- Risk is highest in ulcerative colitis (UC) and Crohn's colitis, especially with pancolitis and disease duration >8-10 years.
- Primary Sclerosing Cholangitis (PSC) is a major independent risk factor for CRC.
- Surveillance colonoscopy with chromoendoscopy and random biopsies begins 8-10 years post-diagnosis.
- The goal is to detect dysplasia, a precursor to cancer, which may be invisible.
- High-grade dysplasia or multifocal low-grade dysplasia are strong indications for colectomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

