VTE Pathophysiology - The Clot Thickens
- Virchow's Triad underpins VTE development, where ≥2 factors are often present.
- Stasis: Post-op immobility, paralysis, prolonged travel.
- Endothelial Injury: Surgery, trauma, central venous catheters.
- Hypercoagulability:
- Inherited: Factor V Leiden, Prothrombin G20210A mutation.
- Acquired: Malignancy, pregnancy, OCPs, Antiphospholipid Syndrome.
⭐ Factor V Leiden is the most common inherited thrombophilia, causing resistance to activated Protein C, a natural anticoagulant.
VTE Diagnosis - Spot the Clot
- Clinical Probability Assessment:
- Wells' Score: Stratifies risk for DVT/PE. Key criteria include:
- Clinical signs of DVT (leg swelling, tenderness)
- Immobilization or surgery in the last 4 weeks
- Previous DVT/PE
- Malignancy
- Wells' Score: Stratifies risk for DVT/PE. Key criteria include:
- Initial Lab Work:
- D-Dimer: A fibrin degradation product. High sensitivity, low specificity.
- Useful to rule out VTE in low-probability patients (if negative).
- A positive result is non-specific and requires imaging.
- D-Dimer: A fibrin degradation product. High sensitivity, low specificity.
- Confirmatory Imaging:
- DVT: Compression ultrasonography is the first-line test.
- PE: CT Pulmonary Angiography (CTPA) is the gold standard.
- 💡 V/Q scan is an alternative if CTPA is contraindicated (e.g., renal failure, contrast allergy).
⭐ PERC Rule (Pulmonary Embolism Rule-out Criteria): In low-risk patients, if all 8 criteria are met (Age <50, HR <100, SaO2 >94%, no unilateral leg swelling, no hemoptysis, no recent surgery/trauma, no prior PE/DVT, no hormone use), PE can be excluded without D-dimer testing.
VTE Management - Clotbusters
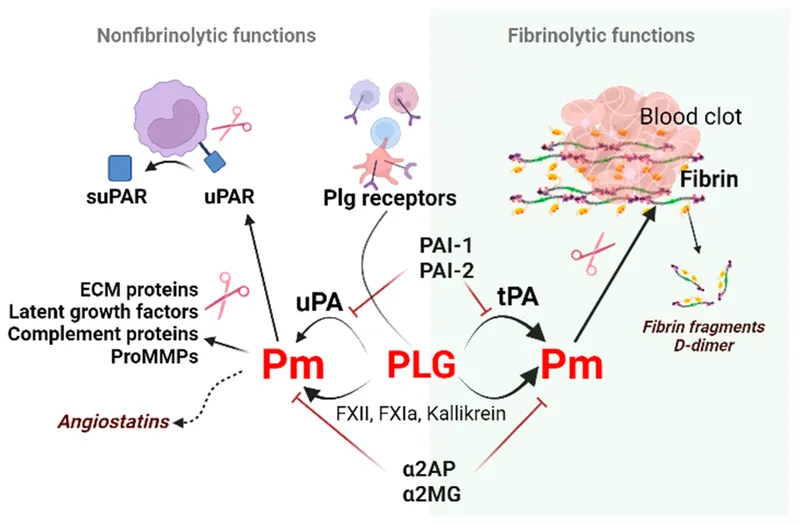
- Mechanism: Thrombolytics (e.g., Alteplase/tPA, Reteplase) activate plasminogen to plasmin, which degrades fibrin and dissolves the clot.
- Primary Indication: Reserved for massive PE with hemodynamic instability (e.g., persistent hypotension SBP <90 mmHg, shock) or limb-threatening DVT (phlegmasia cerulea dolens).
- Administration:
- Systemic IV infusion is the standard approach.
- Catheter-directed thrombolysis offers a lower-dose, targeted alternative, potentially reducing systemic bleeding risk.
- Key Absolute Contraindications:
- Any prior intracranial hemorrhage
- Active bleeding
- Recent major surgery or trauma (<3 weeks)
- Ischemic stroke within 3 months
⭐ The most feared complication of thrombolysis is intracranial hemorrhage. A meticulous screening for contraindications is critical before administration.
VTE Prophylaxis - Pre-emptive Strike
- Goal: Prevent DVT/PE in at-risk hospitalized patients.
- Risk Assessment: Use validated scores (e.g., Padua Prediction Score for medical pts, Caprini for surgical pts).
-
Pharmacologic Options:
- LMWH (e.g., Enoxaparin 40 mg SC daily)
- UFH (e.g., 5000 units SC q8-12h)
- DOACs (e.g., Apixaban, Rivaroxaban)
-
Mechanical Options:
- Intermittent pneumatic compression (IPC) devices.
- Graduated compression stockings (GCS).
⭐ High-Yield: In patients with high bleeding risk (e.g., active bleed, severe thrombocytopenia <50,000/μL), mechanical prophylaxis is preferred over anticoagulants.
High‑Yield Points - ⚡ Biggest Takeaways
- Virchow's triad is key: stasis, hypercoagulability, and endothelial injury.
- Use Wells score to risk-stratify. A low score plus a negative D-dimer reliably rules out VTE.
- CT pulmonary angiography (CTPA) is the gold standard for diagnosing PE.
- Compression ultrasound is the first-line imaging for suspected DVT.
- Treat acutely with heparins or DOACs; bridge to warfarin or continue DOACs for long-term therapy.
- Massive PE with hemodynamic instability requires emergent thrombolysis.
- IVC filters are reserved for when anticoagulation is contraindicated or fails.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

