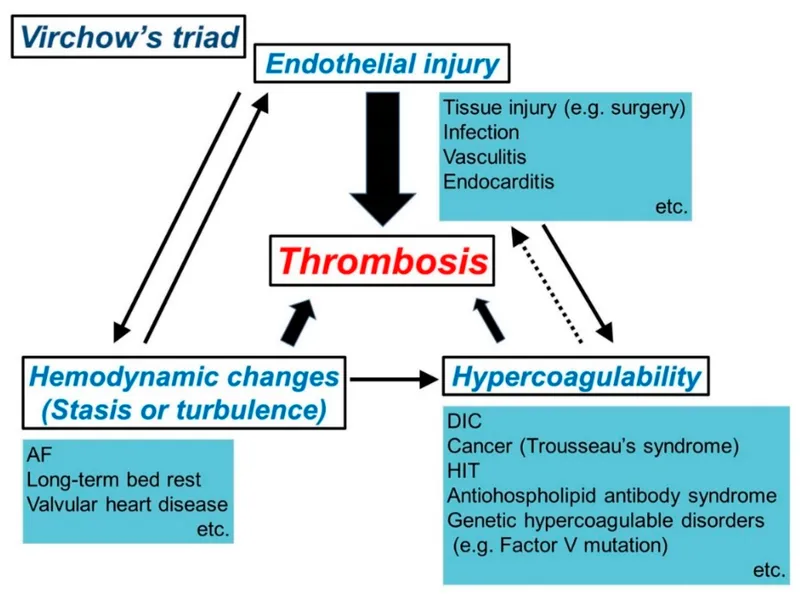
Virchow's Triad - The Clotting Culprits
📌 SHE: Stasis, Hypercoagulability, Endothelial injury.
- Stasis: Disrupted blood flow (e.g., immobilization, atrial fibrillation, venous insufficiency).
- Endothelial Injury: Vessel wall damage (e.g., surgery, trauma, catheters, atherosclerosis).
- Hypercoagulability: Pro-thrombotic state, either inherited or acquired.
- Inherited: Factor V Leiden, Prothrombin gene mutation.
- Acquired: Malignancy, pregnancy, OCPs (estrogen), sepsis.
⭐ Factor V Leiden is the most common inherited thrombophilia in Caucasian populations.
Inherited Thrombophilias - Bad Blood by Birth
-
General Presentation: Suspect in patients < 50 years with unprovoked thrombosis, recurrent venous thromboembolism (VTE), or a significant family history. Most are autosomal dominant.
-
Factor V Leiden (FVL)
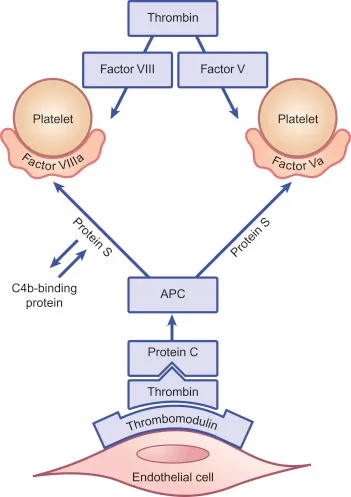
- Pathophysiology: A specific gene mutation makes Factor V resistant to cleavage and inactivation by Activated Protein C (APC).
- Diagnosis: APC resistance assay, confirmed with genetic testing.
-
⭐ Factor V Leiden is the most common inherited thrombophilia in Caucasian populations, significantly increasing the risk for DVT and PE.
-
Prothrombin Gene Mutation (G20210A)
- Pathophysiology: Mutation leads to increased prothrombin levels, promoting excess thrombin generation.
-
Protein C or S Deficiency
- Pathophysiology: Reduced levels of these natural vitamin K-dependent anticoagulants.
- ⚠️ Warning: Can lead to warfarin-induced skin necrosis; always bridge with heparin.
-
Antithrombin Deficiency
- Pathophysiology: Lack of antithrombin impairs the inactivation of thrombin and Factor Xa.
- 💡 Pearl: Patients may show heparin resistance as heparin's anticoagulant effect depends on antithrombin.
Acquired Hypercoagulable States - Clots on the Go
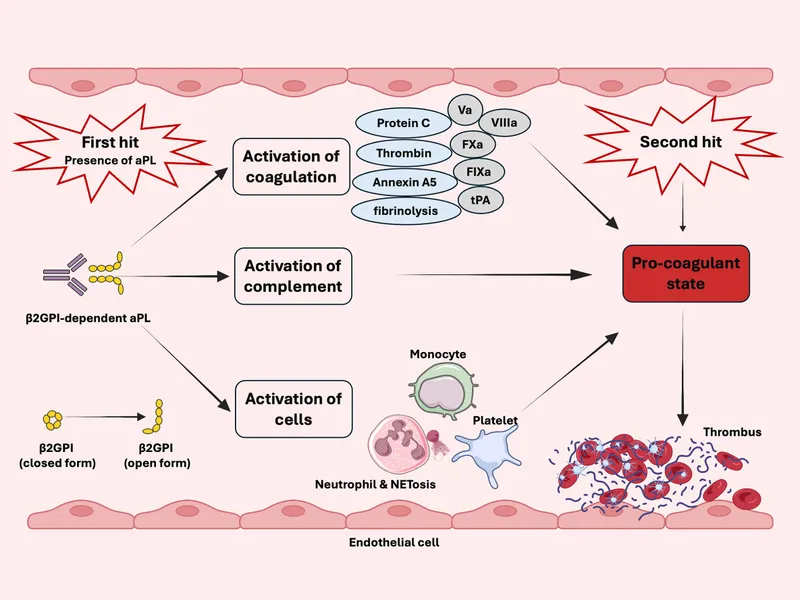
- Antiphospholipid Syndrome (APS): Autoantibodies against phospholipid-binding proteins.
- Clinical: Venous/arterial thrombosis, recurrent fetal loss.
- Labs: Anticardiolipin Ab, Anti-β2 glycoprotein-I Ab, Lupus Anticoagulant.
⭐ Paradoxically, Lupus Anticoagulant can prolong the aPTT in vitro but causes thrombosis in vivo.
- Malignancy: Procoagulants from tumors (e.g., pancreatic, lung adenocarcinoma).
- Presents as Trousseau's syndrome (migratory superficial thrombophlebitis).
- Nephrotic Syndrome: Urinary loss of anticoagulant proteins (Antithrombin III).
- Leads to ↑ risk of DVT, PE, and especially renal vein thrombosis.
- Pregnancy & OCPs: ↑ Estrogen → ↑ clotting factors, ↓ Protein S.
- Immobilization / Post-Op: Stasis + endothelial injury (Virchow's Triad).
- Myeloproliferative Neoplasms: (e.g., Polycythemia Vera) ↑ viscosity & platelet activation.
- Heparin-Induced Thrombocytopenia (HIT): IgG antibodies against heparin-platelet factor 4 (PF4) complexes.
Workup & Management - Spot & Stop the Clot
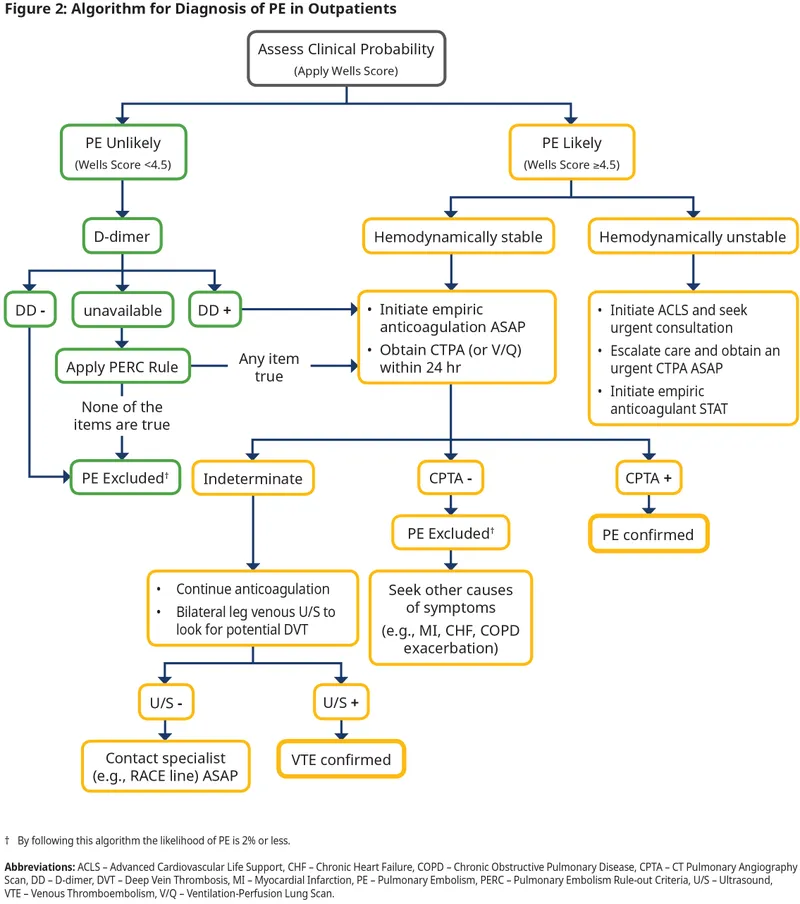
- Initial Workup: Algorithm-driven based on pre-test probability.
-
Acute Management:
- Immediate anticoagulation: DOACs (Apixaban, Rivaroxaban) or LMWH/UFH.
- IVC filter only if anticoagulation is absolutely contraindicated.
-
Long-Term Therapy:
- DOACs are first-line over Warfarin.
- Duration: 3-6 months for provoked VTE; consider lifelong for unprovoked/recurrent cases.
⭐ Factor V Leiden is the most common inherited thrombophilia in Caucasians, causing resistance to activated Protein C.
High‑Yield Points - ⚡ Biggest Takeaways
- Factor V Leiden is the most common inherited thrombophilia, causing resistance to activated Protein C.
- Prothrombin gene mutation is the second most common, leading to ↑ prothrombin levels and venous clots.
- In Antithrombin III deficiency, heparin is less effective as it requires antithrombin to work.
- Protein C or S deficiency carries a risk for warfarin-induced skin necrosis.
- Antiphospholipid syndrome presents with thrombosis, recurrent pregnancy loss, and a paradoxically prolonged aPTT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

