Overview - Red Cell Roulette
- Premature destruction of red blood cells (RBCs) when bone marrow compensation is overwhelmed. RBC lifespan falls below the normal 100-120 days.
- Classification:
- Location: Intravascular (within vessels) vs. Extravascular (spleen, liver).
- Etiology: Inherited (e.g., spherocytosis) vs. Acquired (e.g., autoimmune, MAHA).
- Key Labs: ↑LDH, ↑unconjugated bilirubin, ↑reticulocyte count.
⭐ Haptoglobin is a key marker; it binds free Hb. A sharp ↓ in haptoglobin is highly specific for intravascular hemolysis.
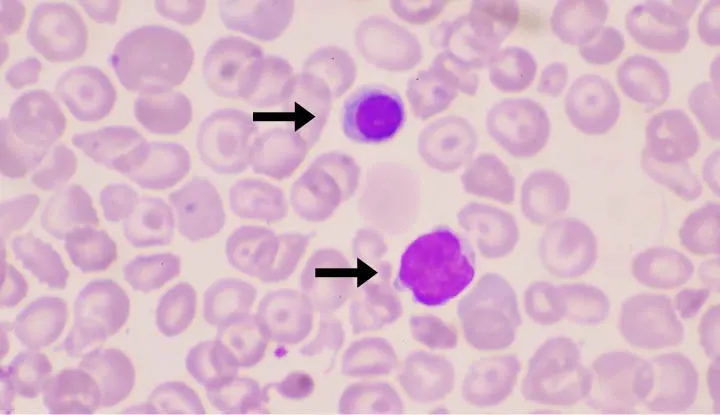
Intrinsic Defects - Born to Lyse
-
Membrane Defect: Hereditary Spherocytosis (HS)
- Autosomal dominant defect in RBC membrane proteins (spectrin, ankyrin).
- Causes loss of membrane surface area → spherocytes (↑ MCHC) → splenic sequestration.
- Presents with splenomegaly, jaundice; diagnosed with osmotic fragility test.
- Risk of aplastic crisis with Parvovirus B19.
-
Enzyme Defects
- G6PD Deficiency (X-linked): ↓ NADPH production impairs defense against oxidative stress.
- Triggers: Sulfa drugs, fava beans, infections.
- Smear shows Heinz bodies and bite cells. 📌 "Bite into some Heinz ketchup."
- Pyruvate Kinase Deficiency (AR): ↓ ATP production → rigid RBCs → extravascular hemolysis.
- G6PD Deficiency (X-linked): ↓ NADPH production impairs defense against oxidative stress.
⭐ In G6PD deficiency, enzyme assays may be falsely normal during an acute hemolytic episode because older, deficient RBCs are hemolyzed first, leaving a younger population of cells.
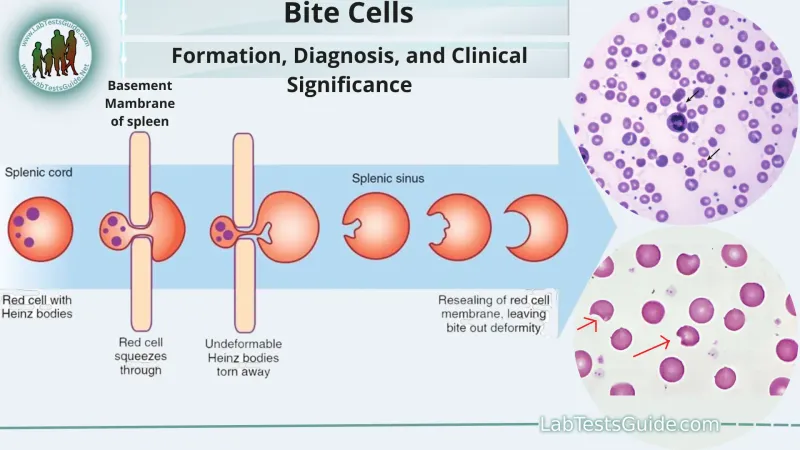
Extrinsic Insults - Acquired Annihilation
-
Immune-Mediated (Coombs Positive)
- Warm AIHA: IgG-mediated; optimal at core body temp. Causes: SLE, CLL, drugs (e.g., α-methyldopa). Labs show spherocytes & +Direct Coombs (anti-IgG).
- Cold Agglutinin Disease: IgM-mediated; optimal <37°C. Causes: Mycoplasma pneumoniae, EBV. Labs show RBC agglutination & +Direct Coombs (anti-C3).
-
Microangiopathic Hemolytic Anemia (MAHA)
- RBC fragmentation in small vessels → Schistocytes ("helmet cells").
- Causes: TTP, HUS, DIC, HELLP syndrome, malignant hypertension.
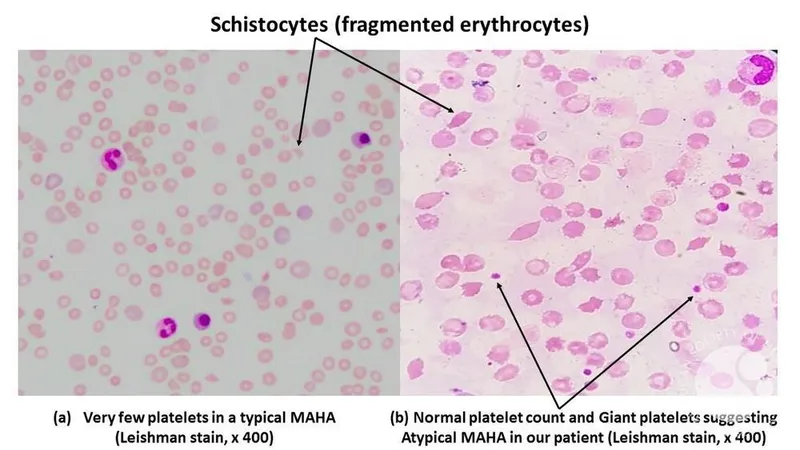
⭐ The TTP classic pentad is Fever, Anemia (MAHA), Thrombocytopenia, Renal failure, and Neurologic symptoms (FAT RN). It's caused by deficient ADAMTS13 activity.
- Other Causes
- Infections: Malaria, Babesia.
- Mechanical Trauma: Prosthetic heart valves, March hemoglobinuria.
Clinical Approach - The Hemolysis Hunt
- Initial Labs: Suspect hemolysis with anemia + ↑ LDH, ↑ indirect bilirubin, and ↓ haptoglobin.
- Reticulocyte Count: Expect ↑ reticulocytes (>2%), indicating bone marrow compensation.
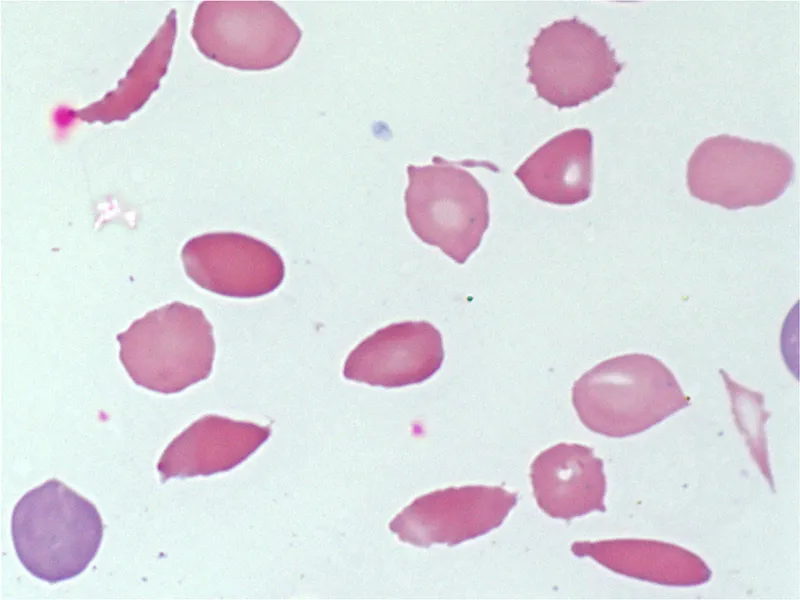
⭐ Haptoglobin is the most sensitive indicator for intravascular hemolysis. Its levels are depleted as it binds free hemoglobin released from lysed RBCs.
High‑Yield Points - ⚡ Biggest Takeaways
- Intravascular hemolysis presents with hemoglobinuria; extravascular with jaundice & splenomegaly.
- Universal labs: ↓ haptoglobin, ↑ LDH, ↑ indirect bilirubin.
- G6PD deficiency: oxidative stress (sulfa drugs, fava beans) triggers hemolysis; see Heinz bodies & Bite cells.
- Hereditary Spherocytosis: AD inheritance, spherocytes, ↑ MCHC, positive osmotic fragility test.
- Sickle Cell Anemia: AR inheritance, vaso-occlusive crises, Howell-Jolly bodies (autosplenectomy).
- AIHA: diagnosed via Direct Coombs test (IgG for warm, C3 for cold).
- PNH: complement-mediated hemolysis with a high risk of thrombosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

