H. pylori - The Stomach Squatter
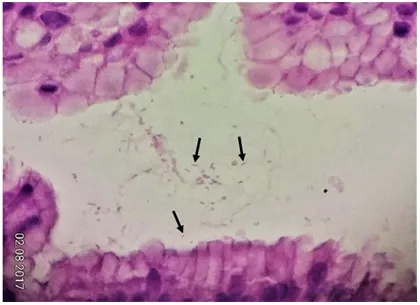
- Gram-negative, spiral-shaped bacterium that colonizes the gastric mucosa.
- Produces urease, which hydrolyzes urea into $NH_3$ and $CO_2$ to neutralize local acid.
- Transmission: Fecal-oral or oral-oral routes.
Clinical Associations:
- Chronic gastritis & Peptic Ulcer Disease (PUD), especially duodenal ulcers.
- Gastric Adenocarcinoma & MALT Lymphoma.
Diagnosis & Management:
- Tests: Urea breath test, stool antigen, or endoscopy with biopsy.
- Treatment:
- 📌 CAP regimen: Clarithromycin + Amoxicillin + PPI.
- Quadruple Therapy for resistance: Bismuth + Metronidazole + Tetracycline + PPI.
⭐ H. pylori is the only bacterium classified as a Class I carcinogen, directly linked to gastric cancer.
Clinical Features - Gut Feelings
- Majority Asymptomatic: Most individuals are carriers without symptoms.
- Chronic Gastritis: The most common clinical outcome.
- Epigastric pain (burning, gnawing), often worse at night or with an empty stomach.
- Nausea, bloating, and early satiety.
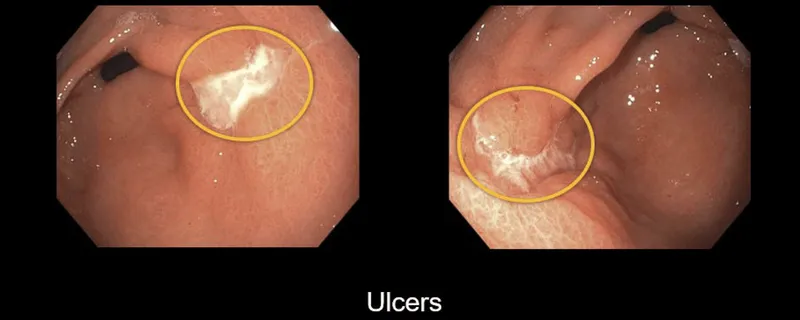
- Peptic Ulcer Disease (PUD):
- Duodenal Ulcer: Pain classically improves with meals.
- Gastric Ulcer: Pain classically worsens with meals.
- Alarm Features: Unintentional weight loss, persistent vomiting, dysphagia, melena/hematemesis, or iron deficiency anemia (IDA).
⭐ H. pylori infection is the strongest known risk factor for gastric MALT lymphoma; successful eradication therapy leads to lymphoma regression in ~75% of cases.
Diagnosis - The Great Detective
- Initial Approach: Choice of test depends on indication for endoscopy.
- Non-Invasive Tests:
- Urea Breath Test (UBT) & Stool Antigen: High sensitivity/specificity for active infection. Used for initial diagnosis and to confirm eradication.
- Serology (IgG): Shows exposure, not active disease. 📌 Stays positive after eradication.
⭐ Test-Modifying Meds: Stop PPIs for 2 weeks and antibiotics/bismuth for 4 weeks before UBT or stool antigen testing to avoid false negatives.
Treatment - Eviction Notice
-
Goal: Eradicate H. pylori to heal peptic ulcers, treat MALT lymphoma, and reduce gastric cancer risk.
-
First-Line Therapy (10-14 days):
- Bismuth Quadruple: PPI + Bismuth + Metronidazole + Tetracycline.
- Preferred if clarithromycin resistance is high or patient had macrolide exposure.
- 📌 Please Make Tummy Better (PPI, Metro, Tetra, Bismuth).
- Clarithromycin Triple: PPI + Clarithromycin + Amoxicillin.
- Use only if local clarithromycin resistance is <15%.
- Use Metronidazole for Amoxicillin if penicillin allergy.
- Bismuth Quadruple: PPI + Bismuth + Metronidazole + Tetracycline.
-
Salvage Therapy: If first-line fails, use an alternative regimen (e.g., Levofloxacin-based).
⭐ Confirm eradication with urea breath test or fecal antigen test >4 weeks after ending antibiotics and >2 weeks after stopping PPIs to prevent false negatives.
- H. pylori is a gram-negative, spiral-shaped bacterium strongly associated with peptic ulcer disease (PUD), especially duodenal ulcers.
- It is a major risk factor for gastric adenocarcinoma and MALT lymphoma.
- Urea breath test and stool antigen testing are the preferred non-invasive diagnostic methods.
- Standard treatment is triple therapy: a Proton Pump Inhibitor (PPI), clarithromycin, and amoxicillin.
- Always confirm eradication with a urea breath or stool antigen test >4 weeks after completing therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

