GI Bleeding - The First Response
- Initial Assessment (ABCs): Secure airway, ensure breathing, manage circulation.
- IV Access: Establish 2 large-bore (≥18 gauge) peripheral IV lines.
- Labs: CBC, CMP, PT/INR, PTT, type & crossmatch.
- Resuscitation:
- Begin IV crystalloids (Normal Saline / Lactated Ringer's).
- Transfuse packed red blood cells (PRBCs) for Hemoglobin < 7 g/dL (or < 9 g/dL in CAD).
- Correct coagulopathy (e.g., FFP for INR > 1.5; platelets if < 50,000/μL).
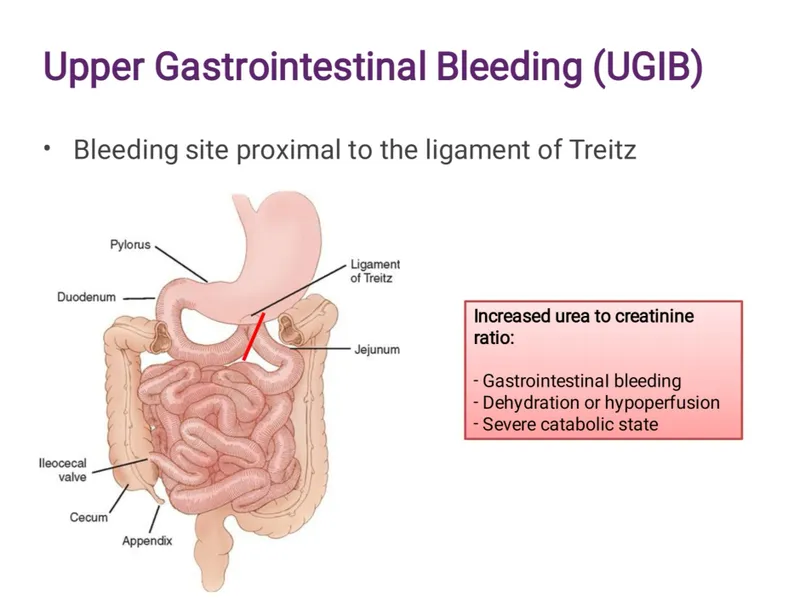
⭐ A BUN/Creatinine ratio > 20 strongly suggests an Upper GI Bleed source due to the digestion and absorption of blood proteins.
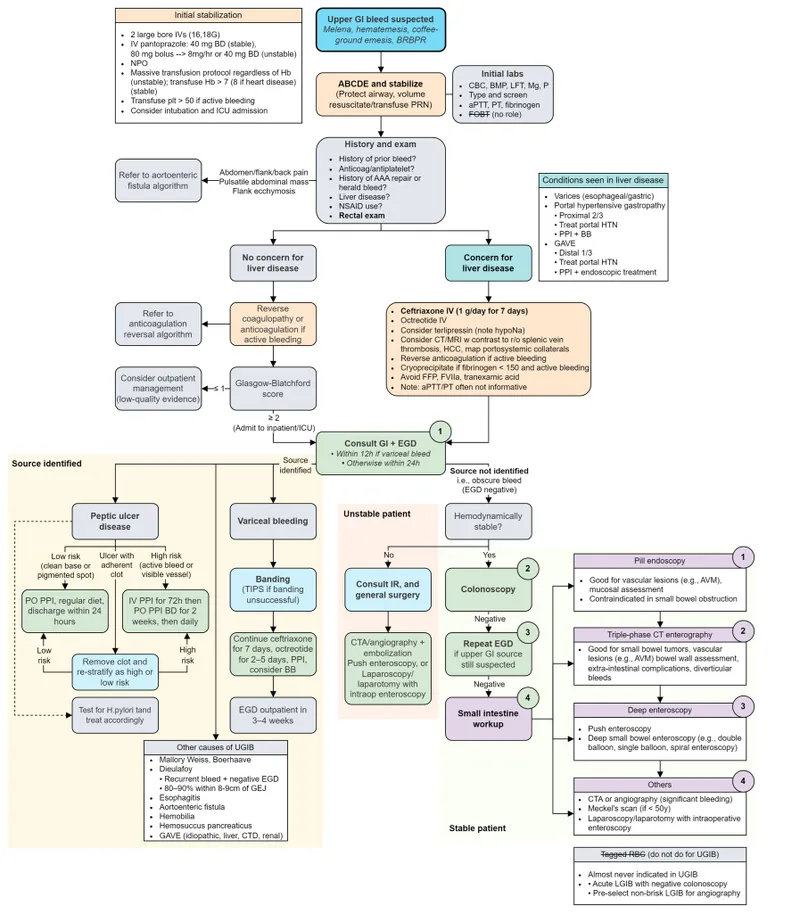
Upper GI Bleed - Above the Ligament
- Definition: Bleeding proximal to the Ligament of Treitz.
- Etiology:
- Peptic Ulcer Disease (PUD) is most common (>50%).
- Esophageal/Gastric Varices (secondary to portal hypertension).
- Mallory-Weiss Tears (forceful retching).
- Erosive gastritis/esophagitis (NSAIDs, alcohol).
- Malignancy.
- Presentation:
- Hematemesis (bright red or coffee-ground emesis).
- Melena (black, tarry stools).
- Anemia symptoms; hemodynamic instability in severe bleeds.
- Management:
- Stabilize: 2 large-bore IVs, fluids, transfuse if Hb < 7 g/dL.
- Medicate: IV Proton Pump Inhibitor (PPI). Consider octreotide for varices.
- Scope: EGD within 24 hours for diagnosis & intervention.
⭐ A BUN/Cr ratio > 20 suggests an upper GI source due to digestion and absorption of blood proteins.
Lower GI Bleed - Below the Divide
- Etiology: Most common is Diverticulosis (painless, arterial bleed). Others: Angiodysplasia (painless, venous), IBD (Crohn's/UC), malignancy, hemorrhoids, ischemic colitis.
- Presentation: Hematochezia (bright red blood per rectum). Always rule out a brisk upper GI bleed first (e.g., NG tube lavage).
- Management Pearls:
- Colonoscopy: Primary diagnostic and therapeutic tool.
- Tagged RBC Scan: Detects slow bleeds (≥0.1 mL/min).
- CTA: Detects faster bleeds (≥0.5 mL/min); better localization than RBC scan.
⭐ Most diverticular bleeds (~80%) resolve spontaneously. Angiodysplasia is a common cause of obscure GI bleeding in the elderly.
Management - Tools & Tactics
- Resuscitation: 2 large-bore IVs, O₂, crystalloids. Transfuse for Hb < 7 g/dL (< 9 in CAD).
- UGIB: IV PPI drip. Octreotide for suspected varices. Endoscopy for diagnosis & therapy (clipping, cautery).
- LGIB: Colonoscopy is primary tool. For ongoing bleeding, use CTA or tagged RBC scan.
- Refractory Bleeds: Angiographic embolization, TIPS (variceal), or surgery.
⭐ IV PPI before endoscopy can decrease high-risk stigmata and the need for endoscopic therapy, but does not reduce rebleeding, surgery, or mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Peptic ulcer disease is the top cause of UGIB; diverticulosis is the most common cause of LGIB.
- First, ensure hemodynamic stability with two large-bore IVs before attempting to identify the source.
- An elevated BUN/creatinine ratio (>20:1) strongly points to an UGIB.
- Endoscopy is the primary diagnostic and therapeutic tool for UGIBs; colonoscopy is used for LGIBs.
- Use IV PPIs for ulcer bleeds; use octreotide and antibiotics for suspected variceal bleeding.
- Hematochezia with instability can indicate a massive UGIB.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

