Functional GI Disorders - The Gut's Acting Up
- Chronic GI symptoms without structural or biochemical abnormalities; a disorder of the gut-brain axis.
- Irritable Bowel Syndrome (IBS): Per Rome IV criteria, recurrent abdominal pain ≥1 day/week for 3 months with ≥2 of:
- Related to defecation
- Change in stool frequency
- Change in stool form (appearance)
- Functional Dyspepsia: Postprandial fullness, early satiety, or epigastric pain without structural disease.
⭐ Red flag symptoms argue against a functional diagnosis: new onset age >50, unintentional weight loss, nocturnal diarrhea, rectal bleeding, iron deficiency anemia.
Irritable Bowel Syndrome (IBS) - The Grumpy Bowel
- Chronic functional GI disorder with recurrent abdominal pain and altered bowel habits, without an identifiable organic cause.
- Pathophysiology: Visceral hypersensitivity, altered gut motility, gut-brain axis dysregulation, and psychosocial factors.
- Diagnosis of Exclusion: Based on Rome IV criteria, after ruling out organic disease. Red flags warrant further investigation (e.g., age >50, rectal bleeding, weight loss).
- Subtypes: IBS-C (constipation), IBS-D (diarrhea), IBS-M (mixed).
⭐ Rome IV Criteria: Recurrent abdominal pain (≥1 day/week for the last 3 months) associated with two or more of the following: related to defecation, change in stool frequency, or change in stool form.
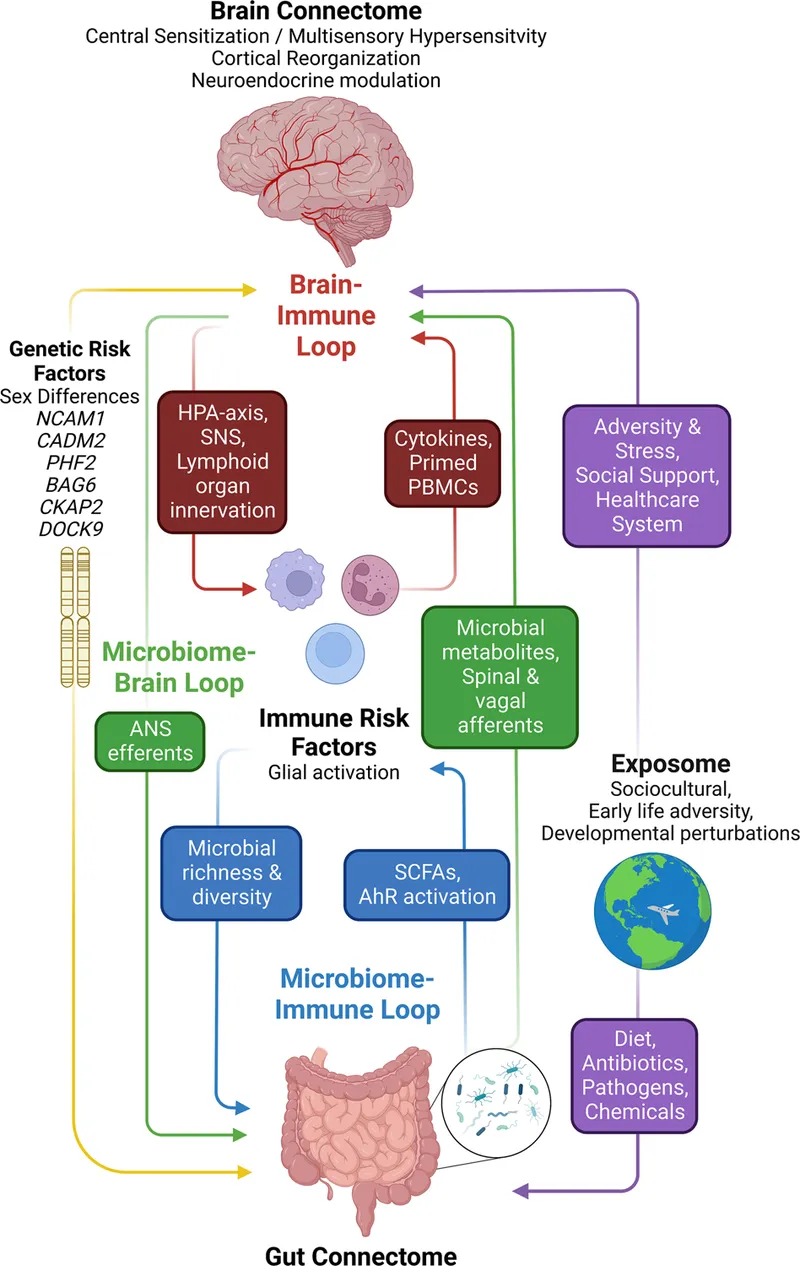
Functional Dyspepsia - The Upset Stomach
*Chronic or recurrent epigastric pain/burning, postprandial fullness, or early satiety with no evidence of structural disease. Diagnosis based on Rome IV criteria (symptoms for ≥3 months, onset ≥6 months prior).
- Key Symptoms: Postprandial fullness, early satiation, epigastric pain/burning.
- Initial Workup: Rule out organic causes. Endoscopy is key if alarm features are present.
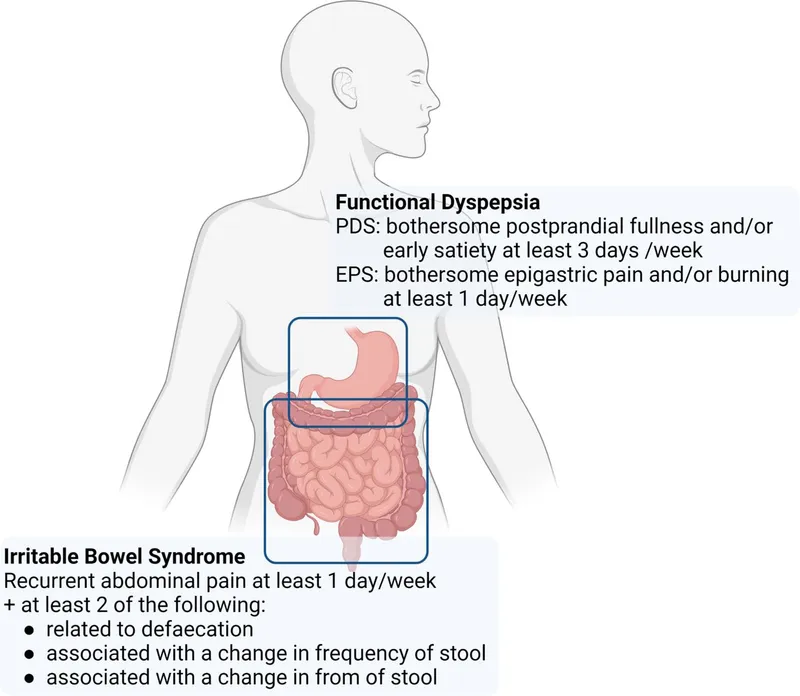
⭐ High-Yield: Functional dyspepsia is a diagnosis of exclusion. The absence of findings on upper endoscopy in a patient with chronic dyspeptic symptoms is a classic presentation.
Diagnosis & Management - Sorting It All Out
- Initial Approach: Rule out organic causes. Focus on identifying alarm features.
- ⚠️ Alarm Features: Age >50, weight loss, nocturnal symptoms, rectal bleeding, iron deficiency anemia, family hx of IBD/cancer.
- Management Strategy
- Lifestyle: Reassurance, education, stress reduction. Low FODMAP diet for IBS.
- IBS-D: Loperamide, Eluxadoline, Rifaximin, Alosetron.
- IBS-C: Fiber, osmotic laxatives (PEG), Lubiprostone, Linaclotide.
- Pain/Bloating: Antispasmodics (Dicyclomine), TCAs (Amitriptyline), SSRIs.
⭐ Rome IV Criteria for IBS: Recurrent abdominal pain at least 1 day/week in the last 3 months, associated with ≥2 of: related to defecation, change in stool frequency, or change in stool form.

High‑Yield Points - ⚡ Biggest Takeaways
- Irritable Bowel Syndrome (IBS) diagnosis hinges on Rome IV criteria: recurrent abdominal pain related to defecation, stool frequency, or form.
- Always rule out organic disease by screening for alarm features like weight loss, rectal bleeding, or anemia.
- First-line management is lifestyle and dietary modification (e.g., low-FODMAP diet) and fiber.
- Functional dyspepsia features chronic epigastric pain or discomfort without any identifiable structural cause on endoscopy.
- Visceral hypersensitivity is a core pathophysiologic mechanism underlying these disorders.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

