Pathophysiology - The Sugar Struggle
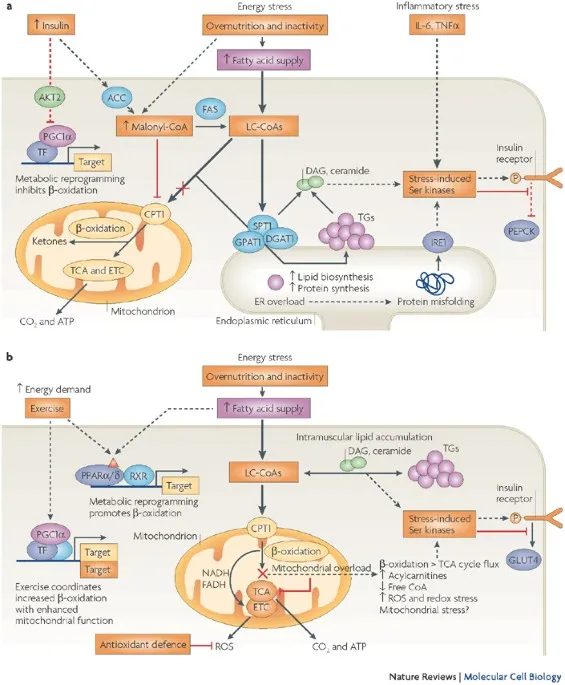
- Insulin Resistance: The primary defect. Peripheral tissues (muscle, adipose) and liver fail to respond to insulin, leading to hyperglycemia.
- Liver: ↑ Hepatic glucose production.
- Muscle: ↓ Glucose uptake.
- Adipose: ↑ Lipolysis, releasing free fatty acids (FFAs) which worsen resistance.
- Beta-Cell Dysfunction: Pancreatic β-cells initially compensate with hyperinsulinemia, but eventually fail, leading to relative insulin deficiency.
- Risk Factors: Central obesity, family history, sedentary lifestyle, ethnicity (Black, Hispanic, Native American).
⭐ Exam Favorite: Initially, T2DM is characterized by high insulin levels (hyperinsulinemia) as the body tries to overcome resistance. Over time, beta-cells exhaust, leading to lower insulin levels (hypoinsulinemia).
Diagnosis & Screening - The Numbers Game
- Screening (USPSTF): Recommended for adults aged 35-70 years with a BMI ≥25. This strategy aims for early detection in at-risk populations to mitigate long-term complications. Re-screen at least every 3 years if results are normal.
- Diagnosis & Prediabetes Thresholds: Diagnosis is established if any one of the primary criteria are met. Prediabetes values signify an elevated risk and a critical window for intervention.
⭐ For an asymptomatic patient, diagnosis requires two abnormal test results (e.g., two tests from one blood draw or two separate occasions).
Pharmacotherapy - The Drug Lineup
-
First Line: Metformin
- MOA: ↓ hepatic gluconeogenesis, ↑ insulin sensitivity.
- SE: GI upset, B12 deficiency, lactic acidosis (rare).
- CI: eGFR < 30 mL/min.
-
Second Line (if ASCVD/HF/CKD):
- GLP-1 Agonists (-tide): CV benefit, promote weight loss.
- SGLT2 Inhibitors (-flozin): CV & renal benefit, promote weight loss.
-
Other Options (based on patient needs):
- Sulfonylureas (e.g., glipizide): ↑ insulin secretion. ⚠️ High risk of hypoglycemia.
- TZDs (-glitazone): ↑ insulin sensitivity. ⚠️ Can cause weight gain, edema, worsen HF.
⭐ SGLT2 inhibitors are notable for reducing the risk of hospitalization for heart failure in patients with and without established ASCVD.
Complications - The Long Haul
- Microvascular
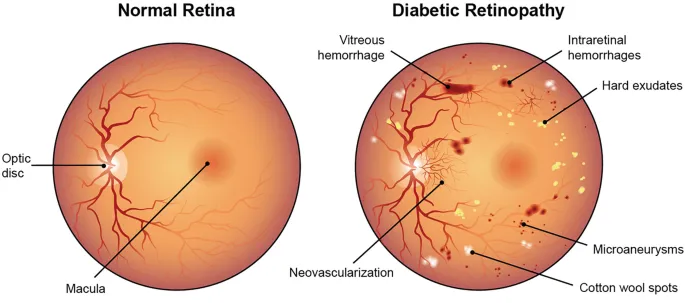
- Retinopathy: Annual screen.
- Nephropathy: Annual screen with urine albumin/creatinine ratio.
- Neuropathy: Annual foot exam.
- Macrovascular
- Coronary Artery Disease (CAD), Peripheral Artery Disease (PAD), Stroke.
- 📌 Manage ABCs: A1c, Blood pressure, Cholesterol.
- Acute
- Hyperosmolar Hyperglycemic State (HHS): Severe hyperglycemia (>600 mg/dL), profound dehydration, high serum osmolality, no significant ketoacidosis.
⭐ In HHS, serum osmolality is often >320 mOsm/kg, and the profound dehydration is a key feature distinguishing it from DKA.
High‑Yield Points - ⚡ Biggest Takeaways
- Type 2 Diabetes Mellitus is primarily a disease of insulin resistance with eventual β-cell dysfunction.
- Obesity and family history are the strongest risk factors.
- First-line treatment is lifestyle modification (diet, exercise) and metformin.
- Diagnostic criteria include an HbA1c ≥ 6.5% or a fasting glucose ≥ 126 mg/dL.
- Long-term complications are macrovascular (CAD, stroke) and microvascular (retinopathy, nephropathy).
- C-peptide levels are detectable, distinguishing it from Type 1 DM.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

