Calcium Homeostasis - The Bone Bank
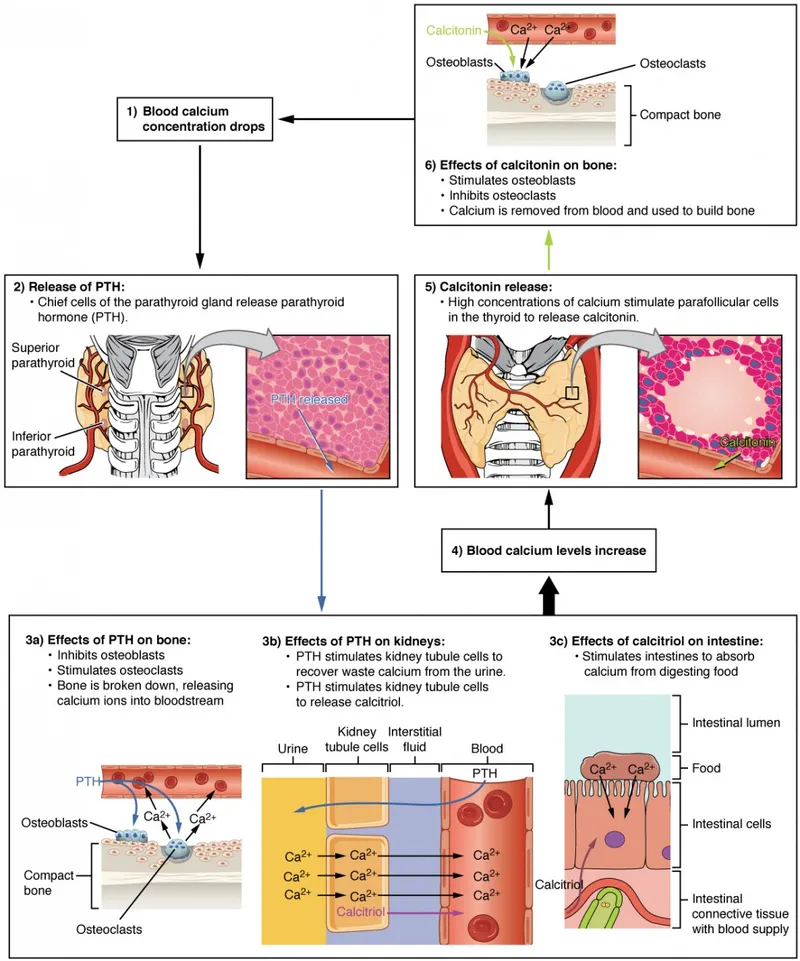
- Parathyroid Hormone (PTH): Chief regulator secreted by chief cells in response to ↓ serum $Ca^{2+}$.
- Bone: ↑ Osteoclast activity, releasing $Ca^{2+}$ and $PO_{4}^{3-}$.
- Kidney: ↑ $Ca^{2+}$ reabsorption (DCT), ↓ $PO_{4}^{3-}$ reabsorption (PCT).
- Kidney: ↑ 1α-hydroxylase activity, converting 25-OH vitamin D to active 1,25-(OH)₂ vitamin D (calcitriol).
- 📌 PTH: Phosphate Trashing Hormone.
- Vitamin D (Calcitriol): ↑ both $Ca^{2+}$ & $PO_{4}^{3-}$ absorption from the gut.
- Calcitonin: Secreted by thyroid parafollicular (C) cells in response to ↑ $Ca^{2+}$. Opposes PTH; "tones down" serum $Ca^{2+}$ by inhibiting osteoclasts.
⭐ In primary hyperparathyroidism, PTH's phosphaturic effect is key. Expect the classic lab triad: ↑ Serum $Ca^{2+}$, ↓ Serum $PO_{4}^{3-}$, and ↑ PTH.
Osteoporosis - Brittle Bone Battle
- Pathophysiology: Low bone mass and microarchitectural disruption leading to increased fracture risk. Imbalance between osteoclast (resorption) and osteoblast (formation) activity.
- Risk Factors: Age, post-menopause (↓ estrogen), smoking, glucocorticoid use, low calcium/vitamin D.
- 📌 ACCESS mnemonic: Alcohol, Corticosteroid, Calcium low, Estrogen low, Smoking, Sedentary.
- Diagnosis: DEXA scan is the gold standard.
- T-score ≤ -2.5.
- Fragility fracture (hip, vertebra) is diagnostic regardless of T-score.
- Management:
- 1st-Line: Bisphosphonates (alendronate).
- 2nd-Line: Denosumab, Teriparatide (anabolic).
⭐ Be aware of atypical femoral fractures with long-term bisphosphonate use.
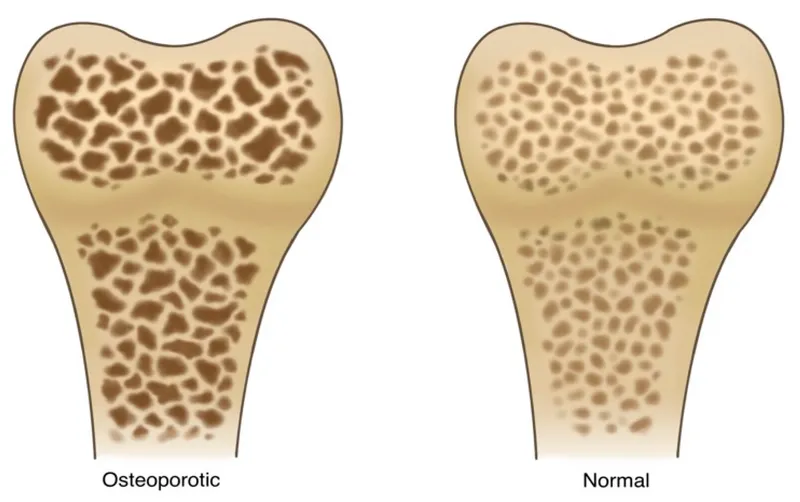
Osteomalacia & Rickets - Bendy Bone Blues
- Pathophysiology: Defective mineralization of bone matrix (osteoid). Rickets affects children (epiphyseal growth plates), while osteomalacia affects adults.
- Etiology: Most commonly due to Vitamin D deficiency → ↓ intestinal absorption of $Ca^{2+}$ and $PO_4^{3-}$.
- Lab Findings: ↓ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$, ↑ Parathyroid Hormone (PTH) (secondary hyperparathyroidism), ↑ Alkaline Phosphatase.
- Clinical Features:
- Adults (Osteomalacia): Diffuse bone pain, muscle weakness, pathologic fractures.
- Children (Rickets): Genu varum (bow-legs), rachitic rosary, craniotabes (soft skull).
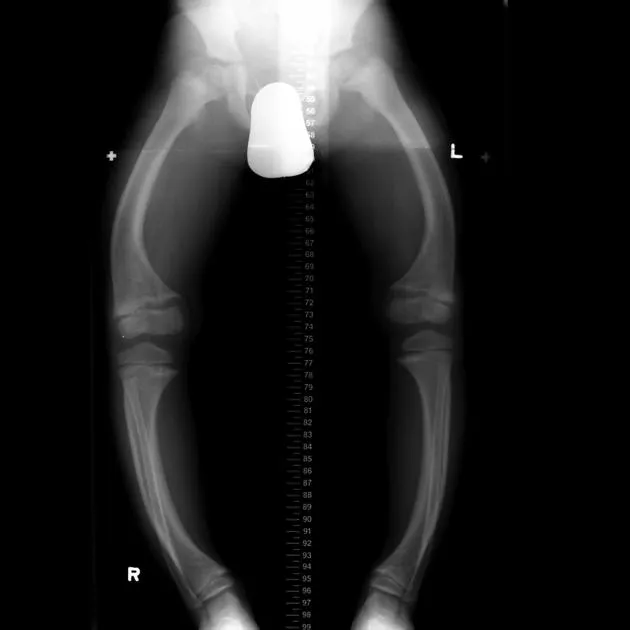
⭐ High-Yield: Look for Looser zones (pseudofractures) on X-ray-transverse, lucent bands perpendicular to the cortex, classically in the femoral neck, scapula, or pubic rami.
Paget Disease of Bone - Hasty & Haphazard
- Disordered, localized bone remodeling in older adults (>55y). Linked to SQSTM1 gene mutations and potentially paramyxovirus.
- Pathophysiology: Starts with a frenzied osteoclastic (lytic) phase, followed by a chaotic osteoblastic (mixed/sclerotic) phase, creating weak, disorganized bone.
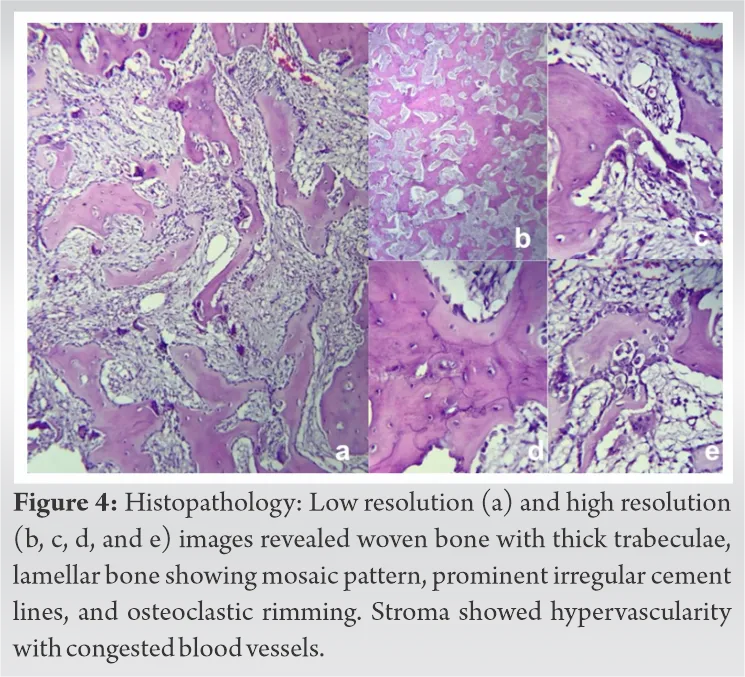
- Histology shows a classic mosaic pattern of lamellar bone with prominent cement lines.
- Clinical: Often asymptomatic. Can present with bone pain, pathologic "chalkstick" fractures, bowing of long bones (tibia), increased hat size, and hearing loss from cranial nerve entrapment.
- Labs: Hallmark is an isolated, markedly ↑ Alkaline Phosphatase (ALP).
⭐ Serum calcium, phosphate, and PTH levels are typically normal.
- Complications: High-output heart failure (AV shunts in bone), osteosarcoma (<1% of cases).
- Treatment: Bisphosphonates (e.g., zoledronic acid).
High‑Yield Points - ⚡ Biggest Takeaways
- Osteoporosis is diagnosed by DEXA scan (T-score ≤ -2.5); first-line treatment is bisphosphonates.
- Vitamin D deficiency causes osteomalacia/rickets (defective mineralization), with ↓ Ca²⁺, ↓ PO₄³⁻, and ↑ PTH/ALP.
- Paget's disease of bone presents with an isolated elevated ALP and a "mosaic" pattern of disorganized bone.
- Primary hyperparathyroidism shows ↑ Ca²⁺, ↓ PO₄³⁻, and ↑ PTH, classically from a parathyroid adenoma.
- Secondary hyperparathyroidism, often from chronic kidney disease, results in ↓ Ca²⁺, ↑ PO₄³⁻, and ↑ PTH.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

