SCD Basics - The Final Countdown
- Definition: Unexpected death from cardiac causes, often within 1 hour of symptom onset in a person without a previously known fatal condition.
- Etiology (Adults):
- >80% due to Coronary Artery Disease (CAD), typically from an acute plaque rupture leading to ischemia.
- Other causes: Cardiomyopathies (HOCM, DCM), channelopathies (e.g., Long QT, Brugada syndrome), and valvular heart disease.
- Terminal Rhythm: Ventricular Fibrillation (VF) or pulseless Ventricular Tachycardia (pVT) is the final common pathway in most cases.
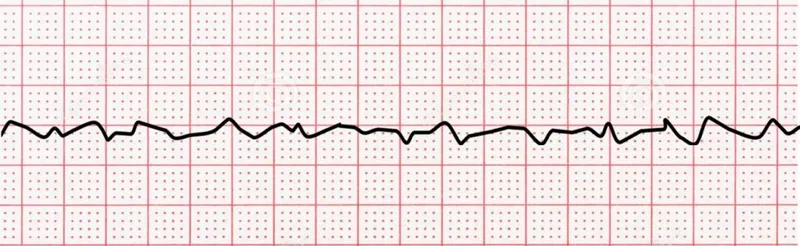
⭐ In young athletes (<35 years), the most common cause of SCD is Hypertrophic Cardiomyopathy (HOCM).
Etiologies & Causes - Heart's Short Circuit
-
Ischemic Heart Disease (>80% of cases)
- Coronary Artery Disease (CAD) is the leading cause, creating a scar-based substrate for re-entrant ventricular tachycardia (VT).
-
Non-Ischemic Cardiomyopathies
- Structural Heart Disease:
- Hypertrophic Cardiomyopathy (HCM)
- Dilated Cardiomyopathy (DCM)
- Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC)
- Primary Electrical Disorders (Channelopathies):
- Long QT Syndrome (LQTS)
- Brugada Syndrome
- Catecholaminergic Polymorphic VT (CPVT)
- Structural Heart Disease:
⭐ In young athletes (<35 years), the most common cause of SCD is hypertrophic cardiomyopathy (HCM).
Risk Stratification - Dodging Danger
- Primary Prevention (No prior SCD event):
- Core metric: Left Ventricular Ejection Fraction (LVEF).
- LVEF ≤ 35% despite optimal medical therapy (OMT) is a class I indication for an Implantable Cardioverter-Defibrillator (ICD).
- Ischemic (Post-MI): Wait ≥ 40 days post-event.
- Non-ischemic: Wait ≥ 3 months after OMT optimization.
- Secondary Prevention (SCD survivor):
- History of VF or hemodynamically unstable VT arrest.
- Strong indication for ICD if the cause was not transient or reversible.
⭐ For primary prevention in post-MI patients, ICD implantation is deferred for at least 40 days to allow for potential LV function recovery. This waiting period is a common exam point.
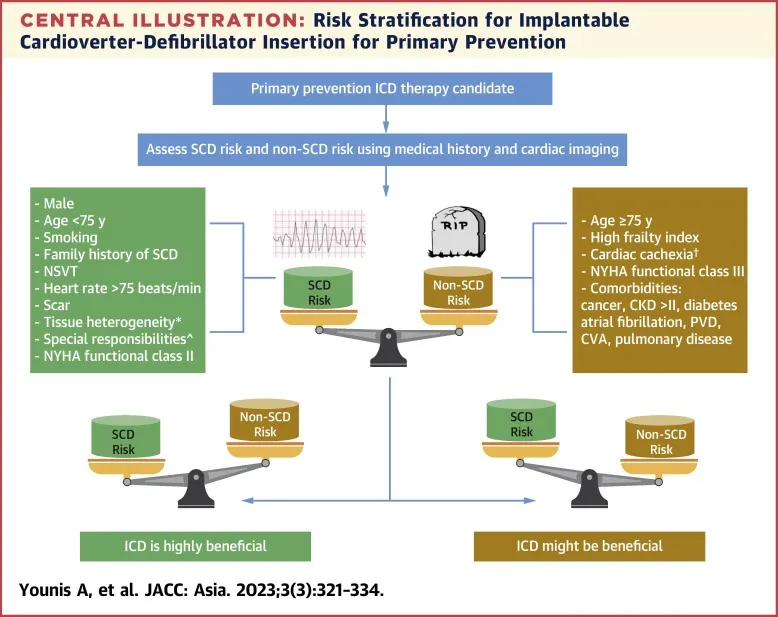
Prevention & ICDs - The Shocking Solution
- Primary Prevention: Aims to prevent SCD in high-risk individuals who have not yet had a life-threatening arrhythmia.
- Core Indication: Left Ventricular Ejection Fraction (LVEF) ≤ 35% due to prior MI (at least 40 days post-MI) or non-ischemic cardiomyopathy (NICM).
- Prerequisite: Patient must be on optimal medical therapy (OMT) for at least 3 months with reasonable survival expectancy (>1 year).
- Secondary Prevention: For survivors of SCD.
- Indication: Documented history of VF arrest or hemodynamically unstable sustained VT.
⭐ In primary prevention for NICM, an ICD is indicated if LVEF is ≤ 35% and NYHA class II-III symptoms persist despite >3 months of OMT (SCD-HeFT trial).
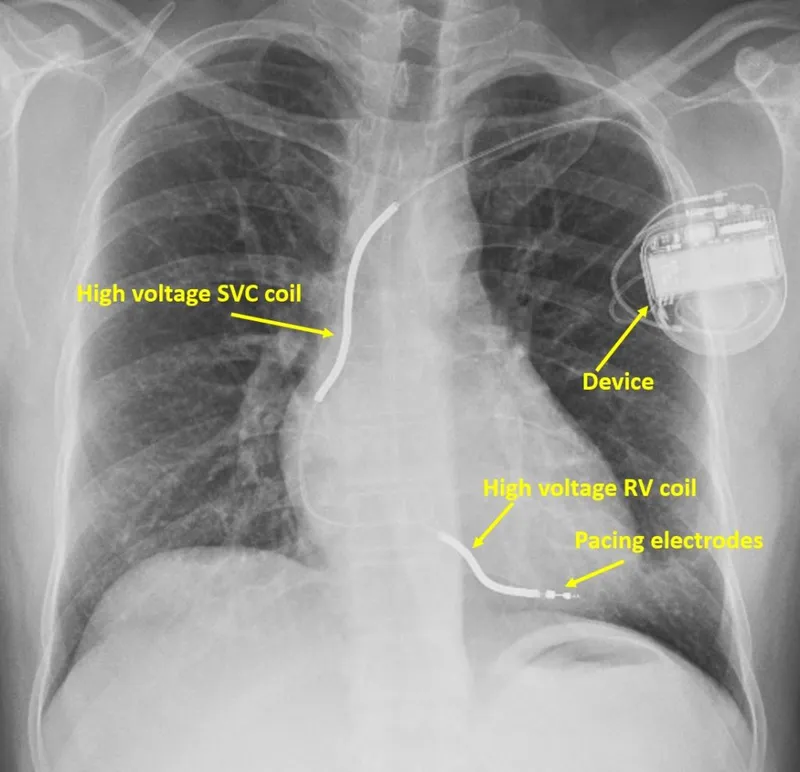
- Most common cause of SCD is ventricular fibrillation (VF), typically from underlying coronary artery disease.
- Key predictors include prior myocardial infarction and severe left ventricular dysfunction (EF < 35%).
- In young athletes, the leading cause is Hypertrophic Cardiomyopathy (HCM), followed by anomalous coronary arteries.
- Immediate survival depends on high-quality CPR and rapid defibrillation.
- Implantable Cardioverter-Defibrillator (ICD) is the mainstay for primary and secondary prevention in high-risk patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

