Vaughan-Williams Classification - The Arrhythmia Orchestra
📌 Mnemonic: Some Block Potassium Channels
| Class | Mnemonic | Mechanism of Action (MOA) |
|---|---|---|
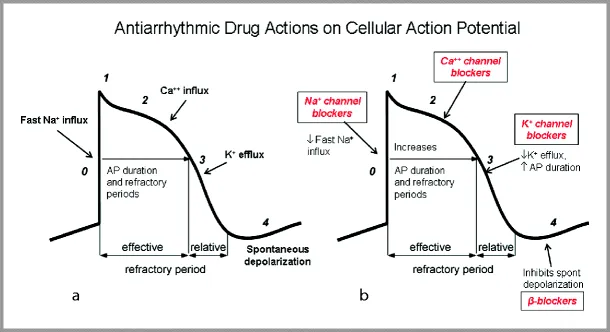
| I | Some | Na+ Channel Blockers |
| II | Block | Beta-Blockers |
| III | Potassium | K+ Channel Blockers |
| IV | Channels | Ca2+ Channel Blockers |
- IA (e.g., Quinidine): Intermediate on/off. ↑Action Potential Duration (APD).
- IB (e.g., Lidocaine): Fast on/off. ↓APD.
- IC (e.g., Flecainide): Slow on/off. No APD change.
⭐ Use-Dependence: Class IC drugs show profound effects at faster heart rates. They are contraindicated post-MI and in structural heart disease due to increased mortality risk.
Class I Agents - Salty Situation Stoppers
-
Mechanism: Block voltage-gated Na⁺ channels, slowing Phase 0 depolarization. State-dependent, binding best to open/inactivated channels.
-
Subtypes & Use-Dependence: (Strongest in IC > IA > IB)
- IA: Quinidine, Procainamide, Disopyramide. Intermediate block.
- 📌 Queen Proclaims Diso's pyramid.
- IB: Lidocaine, Mexiletine. Weak block, fast dissociation. Preferentially affects ischemic tissue.
- IC: Flecainide, Propafenone. Strong block, slow dissociation.
- IA: Quinidine, Procainamide, Disopyramide. Intermediate block.
⭐ CAST Trial: Class IC agents (Flecainide, Propafenone) are contraindicated in structural and ischemic heart disease due to increased mortality.

Class II & IV Agents - Nodal Knockout Crew
- Primary Action: Slow sinoatrial (SA) and atrioventricular (AV) nodal conduction, reducing heart rate.
- Class II (Beta-Blockers): e.g., Metoprolol. Decrease slope of phase 4 diastolic depolarization.
- Class IV (Non-DHP CCBs): e.g., Diltiazem, Verapamil. Decrease slope of phase 0 depolarization.
- Core Use: Rate control in atrial fibrillation and atrial flutter.
- Adverse Effects: Bradycardia, AV block, heart failure exacerbation.
⭐ Beta-blockers are first-line for rate control and show a mortality benefit in post-myocardial infarction patients.
Class III Agents - Potassium's Power Play
- Mechanism: Block K+ channels, prolonging repolarization (Phase 3). This action ↑ action potential duration and the QT interval.
- Key Drugs: Amiodarone, Ibutilide, Dofetilide, Sotalol (AIDS).
- ⚠️ Major Side Effect: A prolonged QT interval significantly increases the risk for Torsades de Pointes (TdP).
⭐ Amiodarone exhibits widespread, multi-organ toxicity, affecting the lungs (fibrosis), liver (hepatitis), thyroid (hyper/hypothyroidism), skin (blue-gray discoloration), eyes (corneal deposits), and nervous system (neuropathy).

Miscellaneous Meds - The Odd Squad
- Adenosine
- Ultra-short half-life (<10s); used to diagnose and terminate SVT.
- Digoxin
- MOA: Directly inhibits the $Na^{+}/K^{+}$-ATPase pump, increasing intracellular calcium.
- Toxicity: Cholinergic symptoms (nausea, vomiting), visual disturbances (yellow halos), and life-threatening arrhythmias.
- Magnesium ($Mg^{2+}$)
- First-line treatment for Torsades de Pointes.
⭐ Adenosine causes transient flushing, chest pain, and a sense of impending doom due to its potent, brief vasodilatory and bronchospastic effects.
High-Yield Points - ⚡ Biggest Takeaways
- Class I drugs exhibit use-dependence; Class IC is strongly proarrhythmic, especially post-MI.
- Class II (beta-blockers) are crucial for rate control in AFib and reduce mortality after myocardial infarction.
- Class III agents (Amiodarone, Sotalol) prolong the QT interval, increasing the risk of Torsades de Pointes.
- Amiodarone carries significant risks of pulmonary fibrosis, thyroid dysfunction, and hepatotoxicity.
- Class IV agents (Verapamil, Diltiazem) control rate in AFib and terminate AVNRT.
- Adenosine is extremely short-acting and used for acute SVT termination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

