MI Complications - Timeline of Trouble
-
Acute (0-48 hours)
- Arrhythmias (esp. V-fib): #1 cause of early death.
- Cardiogenic shock.
- Acute congestive heart failure.
-
Subacute (3-14 days)
- Free wall rupture → Cardiac tamponade.
- Papillary muscle rupture → Acute severe mitral regurgitation.
- Interventricular septal rupture → VSD.
- Fibrinous pericarditis.
-
Chronic (>2 weeks)
- Dressler syndrome (autoimmune pericarditis).
- True ventricular aneurysm → Mural thrombus.
- Chronic heart failure.
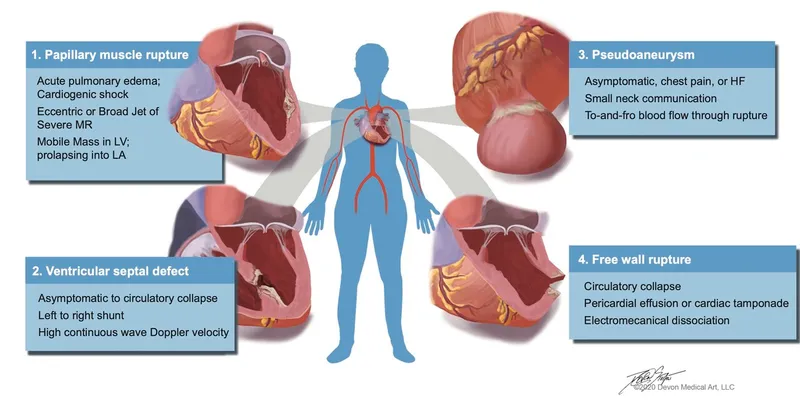
⭐ A new, harsh holosystolic murmur 5-7 days post-MI strongly suggests a ventricular septal rupture, typically heard best at the left sternal border.
Electrical Instability - Faulty Wiring Fiascos
- Arrhythmias are the most common cause of death in the first 48 hours post-MI.
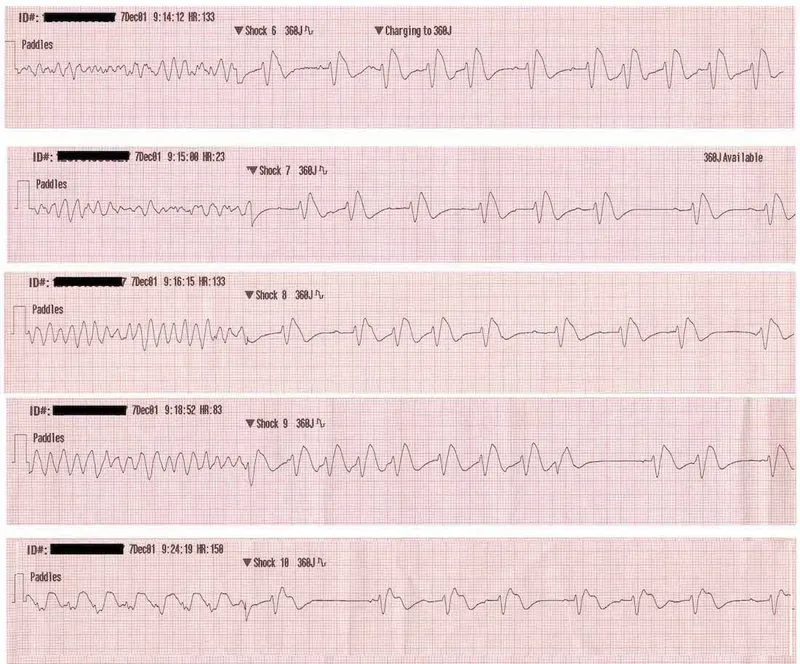
- Ventricular Fibrillation (VFib):
- Most frequent cause of sudden cardiac death, especially in the first 24 hours.
- Requires immediate defibrillation.
- Ventricular Tachycardia (VTach):
- Can be sustained or non-sustained; may lead to VFib.
- Treat with amiodarone or synchronized cardioversion if hemodynamically unstable.
- AV Block:
- Commonly associated with inferior wall MIs (RCA occlusion).
- Often transient; treat symptomatic bradycardia with atropine or temporary pacing.
⭐ Post-inferior MI, new-onset heart block (especially complete heart block) is a major concern due to ischemia of the AV node, which is typically supplied by the RCA.
Mechanical Ruptures - Structural Catastrophes
*Occur subacutely (3-14 days) post-MI as macrophages degrade structural collagen, leading to catastrophic failure. Presents with sudden, severe hypotension and shock.
| Rupture | Onset (days) | Murmur | Vessel | Key Finding |
|---|---|---|---|---|
| Papillary Muscle | 3-5 | New holosystolic (mitral regurg) | RCA | Giant V-waves in PCWP |
| Interventricular Septum | 3-5 | New harsh holosystolic + thrill | LAD | ↑ O₂ step-up (RA → RV) |
| Free Wall | 5-14 | Muffled heart sounds | LAD | Pericardial tamponade, PEA |
📌 Mnemonic: Remember the timeline: Inflammation (1-3 days) → Softening/Rupture (3-14 days) → Scarring (>2 weeks).
Pump & Pericardial Problems - Powerless & Pained
-
Cardiogenic Shock (Killip IV): Severe LV dysfunction causing hypotension (SBP <90 mmHg), ↓ cardiac index (<2.2 L/min/m²), and pulmonary congestion (PCWP >18 mmHg).
-
Pericardial Inflammation: Two distinct forms based on timing.
- **Early Post-Infarction Pericarditis:** Occurs **1-3** days post-MI. Treat with high-dose Aspirin.
- **Dressler Syndrome:** Autoimmune-mediated, weeks to months later. Treat with NSAIDs/Colchicine.
⭐ The friction rub in early pericarditis is often transient; in Dressler's, it's more persistent.
Chronic Remodeling - Scars and Stretches
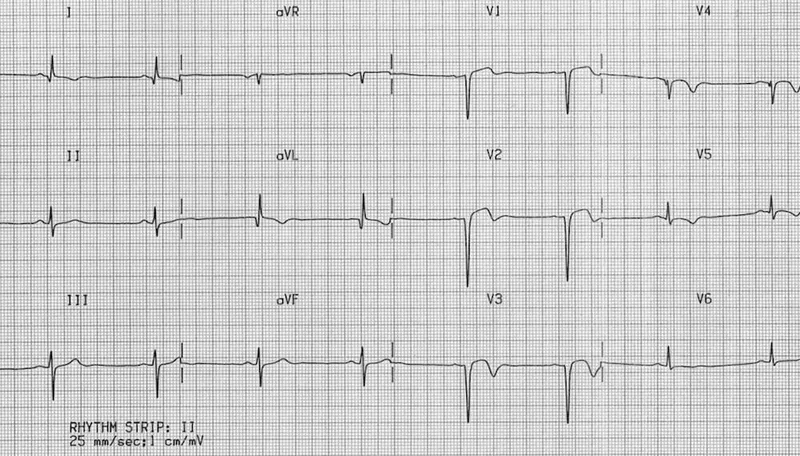
- True Ventricular Aneurysm: A late complication, occurring >2 weeks to months post-MI. The infarcted wall is replaced by a thin, non-contractile fibrous scar that bulges paradoxically during systole.
- Key Feature: Persistent ST-segment elevation in the leads of the prior infarction.
- Major Risks: Formation of a mural thrombus leading to systemic embolization, and progressive heart failure.
⭐ Unlike a pseudoaneurysm, a true ventricular aneurysm has a low risk of rupture because it is composed of fibrous scar tissue.
High‑Yield Points - ⚡ Biggest Takeaways
- Ventricular fibrillation is the most common cause of death within 24 hours post-MI.
- Papillary muscle rupture (2-7 days) causes acute, severe mitral regurgitation.
- Ventricular free wall rupture (5-14 days) leads to cardiac tamponade and sudden death.
- Interventricular septal rupture (3-5 days) creates a VSD with a new holosystolic murmur.
- Ventricular aneurysm (weeks later) causes persistent ST elevation and risk of mural thrombus.
- Dressler syndrome is an autoimmune pericarditis occurring weeks to months post-MI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

