Anticoagulation in ACS - The Clotting Crisis
- Goal: Prevent thrombus extension & re-occlusion.
- Agents: Choice depends on strategy (PCI vs. medical) & bleeding risk.
- Unfractionated Heparin (UFH): Preferred for planned PCI/CABG due to short half-life. Monitor aPTT. ⚠️ Risk of HIT.
- LMWH (Enoxaparin): Good for medical management. Requires renal dose adjustment.
- Bivalirudin: For PCI, especially with high bleeding risk or HIT.
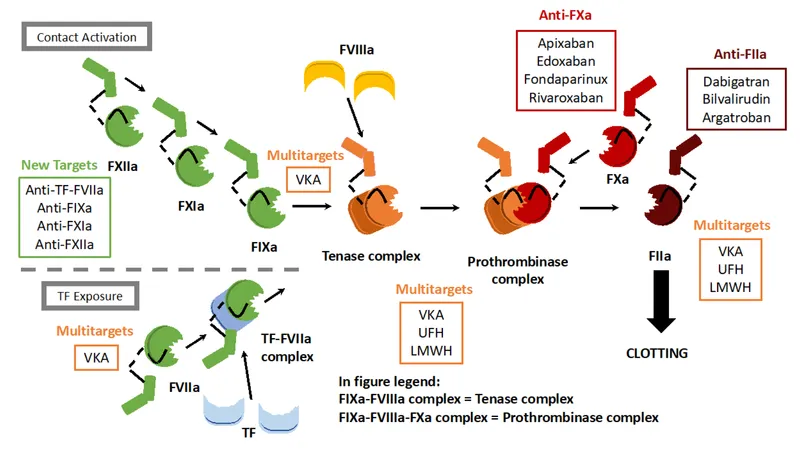
⭐ Fondaparinux, used in medically managed NSTEMI, has the lowest bleeding risk but is contraindicated as the sole anticoagulant during PCI due to a higher risk of catheter thrombosis.
The Anticoagulant Arsenal - Meet the Players
A rapid-comparison of parenteral anticoagulants used in Acute Coronary Syndrome.
| Class | Mechanism of Action | Administration | Key Monitoring | Reversal Agent |
|---|---|---|---|---|
| Unfractionated Heparin (UFH) | Binds Antithrombin III, inactivating Thrombin (IIa) & Factor Xa equally. | IV infusion | aPTT (activated partial thromboplastin time) | 100% Protamine Sulfate |
| LMWH (e.g., Enoxaparin) | Binds Antithrombin III, preferentially inactivating Factor Xa > IIa. | Subcutaneous (SC) | Anti-Xa levels (esp. in renal failure) | Partial w/ Protamine Sulfate |
| Bivalirudin | Direct Thrombin Inhibitor (DTI) - binds directly to thrombin's active site. | IV infusion | ACT (activated clotting time) | None (short half-life) |
| Fondaparinux | Selective Factor Xa inhibitor via Antithrombin III. | Subcutaneous (SC) | Not required | None |
Strategic Selection - The ACS Playbook
Your choice of anticoagulant is guided by the specific ACS type and the intended management strategy-balancing ischemic prevention with bleeding risk.
- Invasive (PCI): Unfractionated Heparin (UFH) or Bivalirudin are the agents of choice.
- Medical (Conservative): Fondaparinux is preferred due to a superior safety profile (↓ bleeding).
- ⚠️ Fondaparinux & PCI: If a patient on fondaparinux requires PCI, administer a bolus of UFH to prevent catheter thrombosis.
⭐ In NSTEMI, Fondaparinux is the only anticoagulant that has demonstrated a mortality benefit (OASIS-5 trial) and carries the lowest risk of major bleeding, making it a prime choice for medically managed patients.
Risks & Regimens - The Fine Print
- Major Risks
- ⚠️ Bleeding: Most common complication. Monitor hemoglobin/hematocrit.
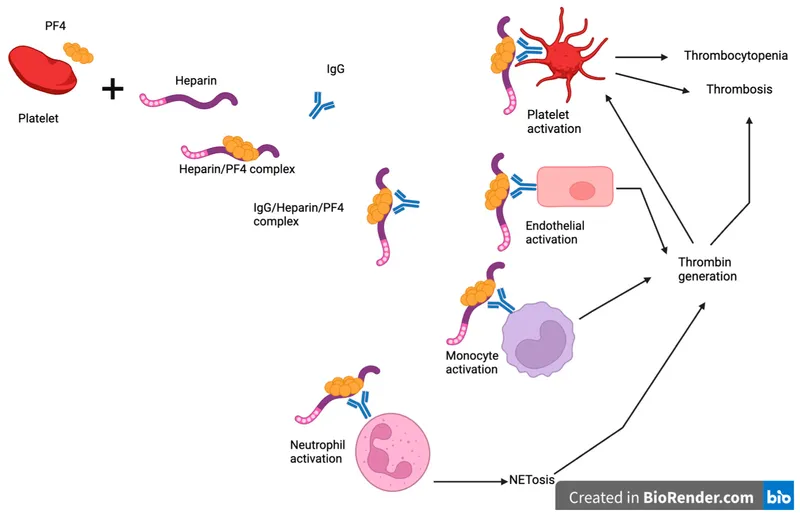
- Heparin-Induced Thrombocytopenia (HIT): Suspect if platelets drop >50%. A prothrombotic state.
- Key Contraindications
- Active internal bleeding
- Recent major surgery or trauma (especially CNS)
- Severe thrombocytopenia (<100,000/μL)
- Dosing & Adjustments
- UFH: 60 U/kg bolus, then 12 U/kg/hr infusion.
- Enoxaparin: 1 mg/kg SC q12h. If CrCl <30 mL/min, dose q24h.
⭐ In HIT, immediately stop all heparin products and start a direct thrombin inhibitor (e.g., Argatroban, Bivalirudin). Do not use LMWH due to high cross-reactivity.
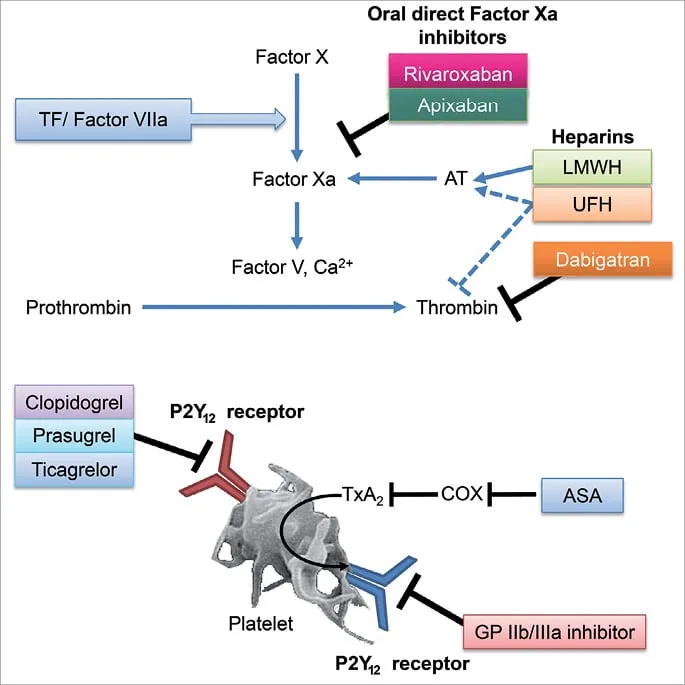
- Dual Antiplatelet Therapy (DAPT), combining aspirin and a P2Y12 inhibitor, is the cornerstone of treatment for all ACS patients.
- The choice of P2Y12 inhibitor-clopidogrel, prasugrel, or ticagrelor-depends on the clinical scenario and bleeding risk.
- Prasugrel is contraindicated in patients with a history of stroke or TIA due to increased bleeding risk.
- A parenteral anticoagulant (e.g., heparin, enoxaparin, bivalirudin) is added to DAPT during the initial phase.
- Glycoprotein IIb/IIIa inhibitors are reserved for high-risk patients undergoing PCI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

