Intro to QoL - More Than a Pulse
Quality of Life (QoL) is a multidimensional concept assessing a patient's subjective perception of their well-being. It extends beyond mere absence of disease to include overall life satisfaction.
-
Core Domains (WHO-QoL):
- Physical Health (pain, energy)
- Psychological (positive feelings, self-esteem)
- Social Relationships (personal support)
- Environment (safety, financial resources)
-
Assessment: Crucial in chronic illness (cancer, heart failure) & palliative care. Tools include SF-36, EQ-5D.
⭐ In oncology, patient-reported QoL scores can be a stronger predictor of hospitalizations and survival than some objective tumour markers.
QoL Assessment - Scoring the Feeling
Quality of Life (QoL) is measured using validated scales. Performance status is a key proxy, especially in oncology.
| Tool | Type | Key Features |
|---|---|---|
| EQ-5D-5L | Generic | 5 dimensions (Mobility, Self-care, Usual activities, Pain, Anxiety). Simple, 5-level response. |
| SF-36 | Generic | Broader 8-domain survey (e.g., physical functioning, social functioning, pain, vitality). |
| Karnofsky | Performance | Cancer-specific. Scale from 100 (Normal) to 0 (Dead). Clinician-assessed. |
| ECOG/WHO | Performance | Simpler cancer scale. 0 (Fully active) to 5 (Dead). Widely used in trials. |
⭐ ECOG 2 is a key threshold: Ambulatory and capable of self-care, but unable to carry out any work activities. Up and about more than 50% of waking hours.
Prioritizing Interventions - The Balancing Act
Balancing life extension with Quality of Life (QoL) is a central clinical skill. The goal is to align medical interventions with the patient's values and overall well-being, not just survival.
- Core Metric: Quality-Adjusted Life Year (QALY) is a key measure.
- $QALY = (Years of Life Gained) \times (Utility Value)$
- Utility Value: A score from 0 (death) to 1 (perfect health) representing QoL.
- Key Considerations:
- Patient Autonomy: Respecting the patient's goals and preferences.
- Treatment Burden: Assessing the impact of side effects, financial cost, and time.
- Prognosis: The likely outcome with and without the intervention.
⭐ A QALY of 1.0 represents a year in perfect health. Interventions are often evaluated based on their cost per QALY gained, guiding health policy and clinical choices.
Decision Flowchart:
Key Scenarios - Palliation & Geriatrics
- Goal Shift: Transition from curative intent to optimizing Quality of Life (QoL), prioritizing patient values and functional status.
- Palliative Principles:
- Symptom Control: Use validated tools (e.g., ESAS). Address "total pain" (physical, psychological, social, spiritual).
- Opioid Use: Follow WHO analgesic ladder. Morphine is key for pain/dyspnea.
- Advance Care Planning: Document patient wishes via Living Will & Durable Power of Attorney for Healthcare.
- Geriatric Focus:
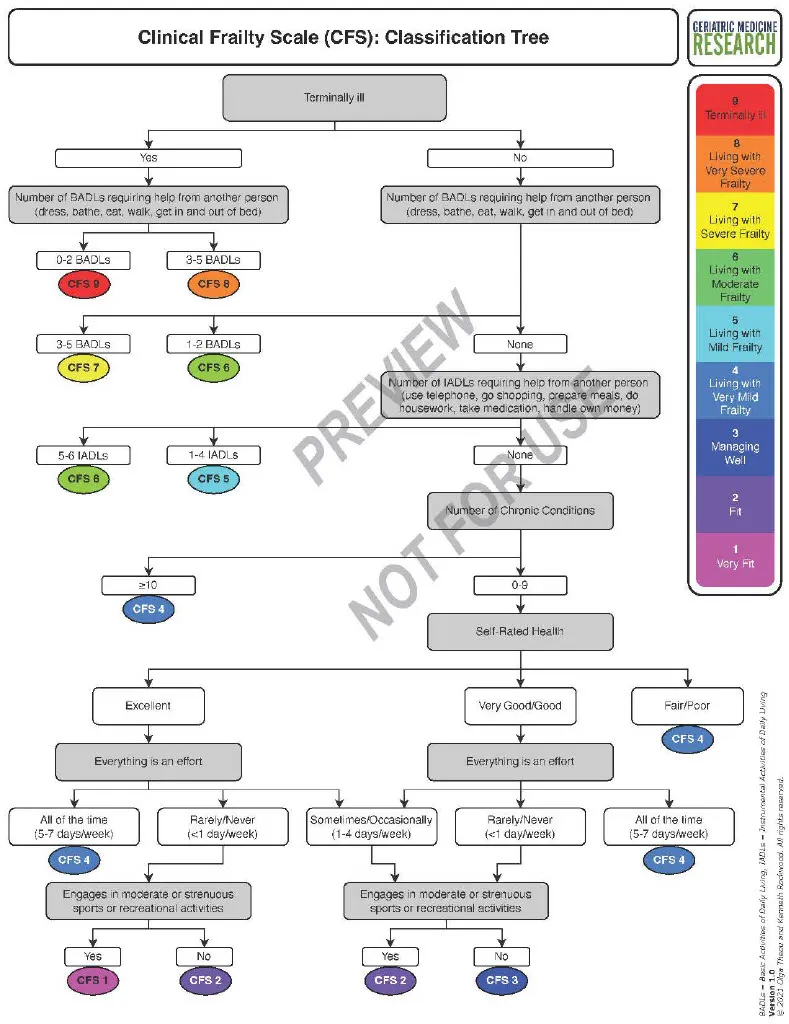
- Frailty Assessment: Use Clinical Frailty Scale to guide intervention intensity.
- De-prescribing: Systematically reduce polypharmacy to prevent adverse drug events.
⭐ The "Surprise Question" ("Would you be surprised if this patient died in the next year?") is a key trigger to initiate goals of care conversations.
High-Yield Points - ⚡ Biggest Takeaways
- In CCS cases, prioritize interventions enhancing Quality of Life (QoL), not just extending survival, especially in chronic or terminal illness.
- Use objective measures like QALYs (Quality-Adjusted Life Years) to balance longevity with well-being.
- The goal often shifts from curative treatment to symptom control and palliative care.
- Patient autonomy and shared decision-making are paramount when considering QoL.
- Consider the socio-economic impact and cost-effectiveness of interventions on the patient's life.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

