PCC Foundations - Patient Over Protocol
- Core Principle: A shift from a disease-focused model to care that is respectful of and responsive to individual patient preferences, needs, and values, ensuring that patient values guide all clinical decisions.
- Shared Decision-Making (SDM): The cornerstone of PCC.
- A collaborative process between clinician and patient.
- Involves discussing treatment options, evidence, and the patient's personal context.
- Goal: To select a management plan that is medically sound and aligns with the patient's priorities.
- Key Components:
- Empathy: Understand the patient's experience.
- Communication: Elicit preferences, explain options clearly.
- Respect: Uphold patient autonomy and dignity.
⭐ In CCS cases, demonstrating SDM by offering choices and asking, "What matters most to you?" can significantly boost your score, reflecting a higher order of clinical competence.
Shared Decision-Making - The SHARE Approach
A collaborative process where clinicians and patients make healthcare decisions together, balancing clinical evidence with the patient's preferences and values.
📌 The SHARE Model:
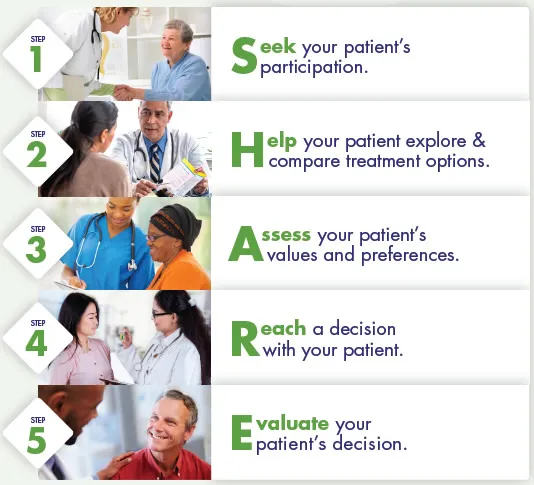
- Seek your patient's participation.
- Summarize the health problem and explicitly state that a choice needs to be made.
- Help your patient explore and compare treatment options.
- Present evidence-based options, discussing risks and benefits.
- Use patient decision aids.
- Assess your patient's values and preferences.
- Ask what matters most to them regarding their health and life.
- Reach a decision with your patient.
- Jointly decide on the best course of action.
- Evaluate your patient's decision.
- Revisit the decision during follow-up to ensure it remains appropriate.
⭐ The core of patient-centered care is not just giving information, but also ensuring the patient's values guide all clinical decisions.
Prioritization Skills - Juggling Patient Needs
- Foundation: Always start with the ABCDE approach to identify and treat immediate life-threats.
- Triage Sieve: Differentiate between Urgent (immediate threat to life/limb) and Important (necessary for long-term outcome but can wait).
- Urgent: Airway compromise, active hemorrhage, septic shock.
- Important: Glycemic control, nutritional support, routine meds.
- Dynamic Process: Re-evaluate priorities as the patient's condition evolves. What was important may become urgent.
- Shared Decision Making (SDM): When multiple options exist with similar clinical urgency, involve the patient. Discuss risks, benefits, and alternatives to align care with their values.
⭐ The Two-Challenge Rule: In a crisis, if your concern is ignored, state it at least twice. If still unaddressed, you have a responsibility to seek a third party's input. This is a key patient safety tool.
High‑Yield Points - ⚡ Biggest Takeaways
- Prioritize ABCDE (Airway, Breathing, Circulation) first in all emergencies, overriding immediate patient preference.
- In stable patients, the core is shared decision-making, aligning care with patient values and preferences.
- Informed consent requires a clear discussion of risks, benefits, and alternatives (RBA).
- For incapacitated patients, decisions fall to the legally authorized surrogate decision-maker.
- Always honor a patient's valid advance directive or living will.
- Effective, empathetic communication is the foundation of patient-centered care.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

