Endoscopic Procedures - The Inner Tube Tour
-
Upper GI Endoscopy (EGD): For dysphagia, GERD, PUD, & upper GI bleeds. Allows biopsy (H. pylori, malignancy) & therapy (variceal banding).
-
Colonoscopy: Gold standard for colorectal cancer (CRC) screening (age 45+). For lower GI bleeds, IBD workup. Requires bowel prep.
-
ERCP: Therapeutic for biliary/pancreatic ducts (stones, strictures). ⚠️ High risk of pancreatitis (~5-10%).
-
Endoscopic Ultrasound (EUS): Best for loco-regional staging (T/N) of GI cancers. Guides FNA for tissue diagnosis.
-
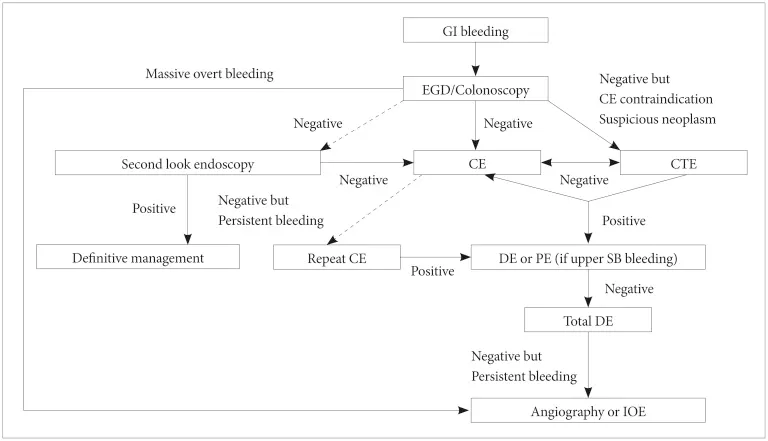
Capsule Endoscopy: Investigates obscure GI bleeding by visualizing the small bowel.
⭐ In suspected variceal bleeding, perform EGD within 12 hours for diagnosis and endoscopic variceal ligation (EVL).
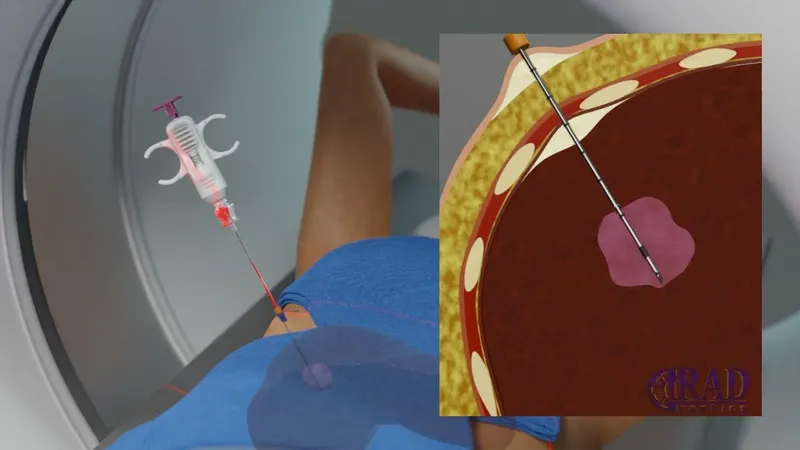
Interventional Radiology - Guided Needle Adventures
-
Guidance Modalities: Ultrasound (USG) for real-time, superficial lesions; CT for deep, complex locations (abdomen, lung).
-
Core Procedures:
- Fine Needle Aspiration Cytology (FNAC): Aspirates cells for cytology (e.g., thyroid, lymph nodes). Less invasive.
- Core Needle Biopsy (CNB): Obtains a tissue cylinder for histology (e.g., liver, kidney, breast). Provides architectural information.
- Percutaneous Catheter Drainage (PCD): For abscesses, collections. Pigtail catheters are commonly used.
⭐ Contraindication Alert: Uncorrectable coagulopathy is a major contraindication. Aim for INR <1.5 and Platelets >50,000/μL before proceeding.
Electrophysiology - Charting The Sparks
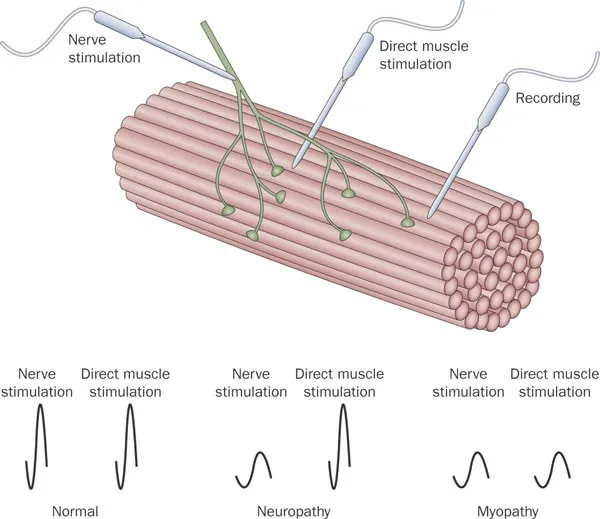
- Nerve Conduction Study (NCS): Measures nerve signal speed (velocity) & strength (amplitude). Differentiates peripheral neuropathies.
- Demyelinating: ↓ velocity, ↑ latency.
- Axonal: ↓ amplitude (CMAP/SNAP).
- Electromyography (EMG): Needle electrode assesses muscle electrical activity (MUAPs). Differentiates myopathy vs. neuropathy.
- Myopathy: Small, short duration, polyphasic MUAPs with early recruitment.
- Neuropathy: Large, long duration, polyphasic MUAPs with late recruitment.
- Repetitive Nerve Stimulation (RNS): Crucial for NMJ disorders.
- Myasthenia Gravis: >10% decremental response on slow RNS (3 Hz).
- LEMS: Incremental response (>100%) on rapid RNS (20-50 Hz).
⭐ A decremental response of >10% in CMAP amplitude on slow (3 Hz) Repetitive Nerve Stimulation is the classic electrodiagnostic finding for Myasthenia Gravis.
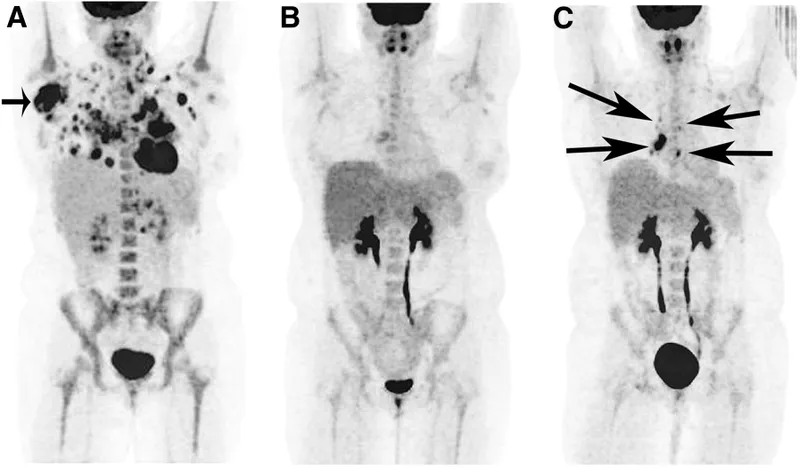
Nuclear Medicine - Radioactive Roadmaps
- PET-CT (Positron Emission Tomography): Uses $F^{18}$-FDG to map metabolic activity. Crucial for cancer staging, monitoring treatment response, and identifying viable myocardium.
- SPECT (Single Photon Emission CT): For functional imaging, e.g., Myocardial Perfusion Imaging (Thallium-201, Tc-99m sestamibi) to detect ischemia.
- Bone Scan: Uses Technetium-99m MDP to detect skeletal metastases, occult fractures, and osteomyelitis. Shows areas of ↑ osteoblastic activity.
- V/Q Scan: Assesses ventilation/perfusion mismatch for Pulmonary Embolism diagnosis, especially when CTPA is contraindicated (e.g., renal failure, pregnancy).
⭐ On a thyroid scan, a "cold" nodule (doesn't take up radioiodine) carries a higher suspicion of malignancy (~15-20%) compared to a "hot" nodule.
High‑Yield Points - ⚡ Biggest Takeaways
- In CCS, always progress from least to most invasive and cost-effective diagnostic tests.
- Reserve specialized procedures like endoscopy or biopsy for when initial tests are inconclusive but clinical suspicion remains high.
- These are often the gold standard for diagnosis but are not first-line due to risk or cost.
- The "next best step" is rarely an immediate invasive test without foundational workup.
- Always confirm patient stability and check for contraindications first.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

