Glycogen Basics - The Body's Sugar Stash
- Function: Main storage form of glucose in the body, providing a rapid energy reserve.
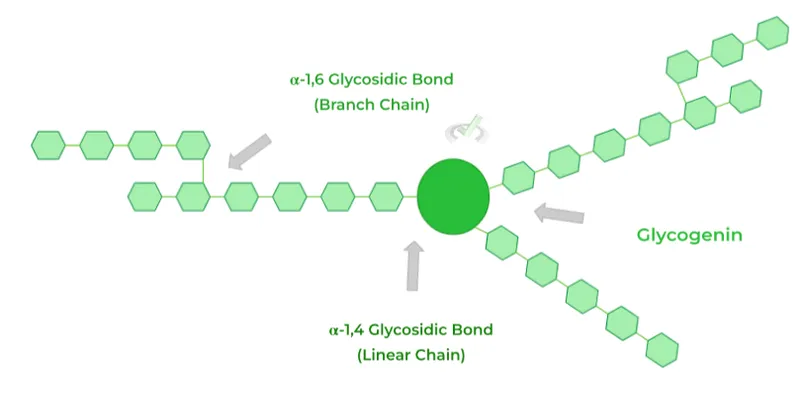
- Structure: A large, branched polymer of glucose.
- Linear chains are linked by $α-1,4$ glycosidic bonds.
- Branch points are created by $α-1,6$ glycosidic bonds every 8-12 residues.
- Storage Sites:
- Liver: Maintains blood glucose. Stores up to 10% of its weight.
- Skeletal Muscle: Fuel reserve for muscle contraction. Stores 1-2% of its weight.
⭐ Muscle lacks Glucose-6-Phosphatase, so its glycogen stores cannot be released into the bloodstream to maintain blood glucose levels.
Glycogenesis - Building the Branches
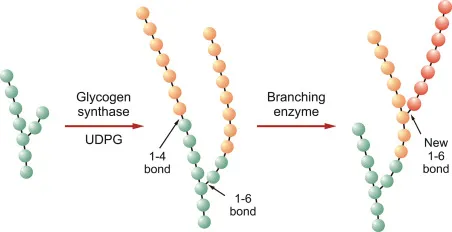
- Key Enzyme: Glycogen Branching Enzyme (amylo-α-1,4→α-1,6-transglucosidase).
- Action: It cleaves a block of approximately 7 glucose residues from a linear chain (that is at least 11 residues long).
- This block is then transferred to an interior glucose residue, forming an α-1,6 glycosidic bond.
- This process increases glycogen solubility and the number of non-reducing ends for faster synthesis and degradation.
⭐ Andersen Disease (GSD Type IV) results from a branching enzyme deficiency. The accumulation of abnormal glycogen with few branches leads to infantile cirrhosis and hepatosplenomegaly.
Glycogenolysis - Tapping the Reserve
- Primary Goal: Break down stored glycogen to release glucose, primarily in liver and muscle.
- Key Enzymes:
- Glycogen Phosphorylase: Cleaves α-1,4 glycosidic bonds. Requires pyridoxal phosphate (Vitamin B6).
- Debranching Enzyme: Handles α-1,6 branch points with two activities: transferase and glucosidase.
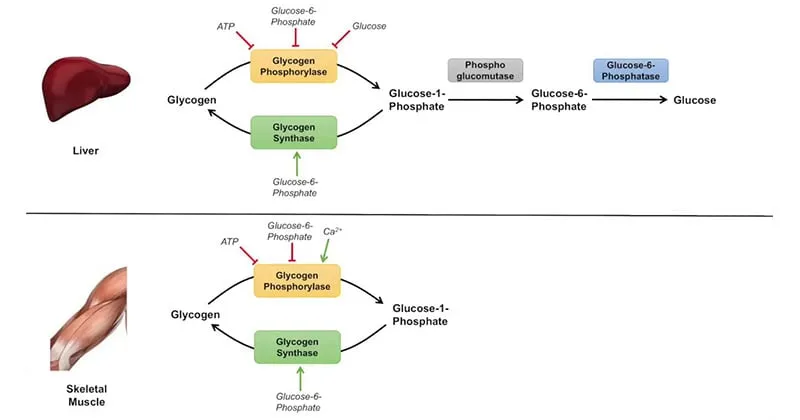
⭐ Liver-Specific Step: Only the liver has Glucose-6-phosphatase, allowing it to release free glucose into the bloodstream to maintain blood sugar levels. Muscle lacks this enzyme; its glycogen stores are for its own energy needs.
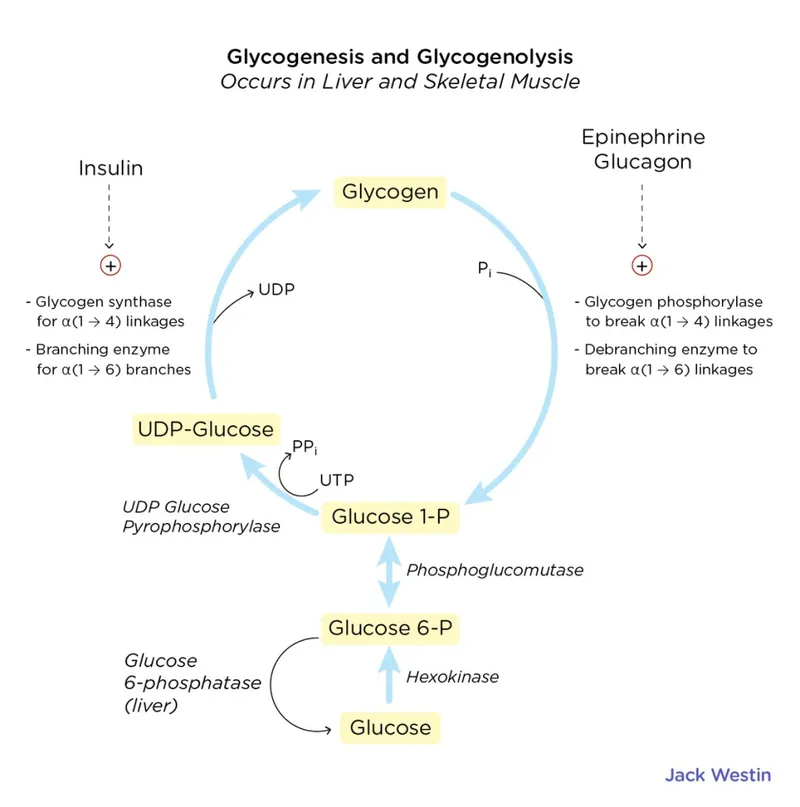
Regulation - The Metabolic Tug-of-War
Hormonal and allosteric signals create a reciprocal push-pull.
- Fed State (Insulin): ↑ Insulin activates protein phosphatase.
- Dephosphorylates & activates Glycogen Synthase.
- Dephosphorylates & inactivates Glycogen Phosphorylase.
- Fasting/Stress (Glucagon/Epinephrine): ↑ cAMP/PKA pathway.
- Phosphorylates & inactivates Glycogen Synthase.
- Phosphorylates & activates Glycogen Phosphorylase.
📌 Insulin Dephosphorylates; Glucagon Phosphorylates.
⭐ In muscle, $Ca^{2+}$ (contraction) and AMP (ATP use) are potent allosteric activators of glycogen phosphorylase, ensuring rapid energy for exercise independent of hormones.
Glycogen Storage Diseases - When the Stash is Stuck
- Type I (von Gierke): Glucose-6-phosphatase def. → Severe fasting hypoglycemia, ↑ lactate, hepatomegaly, hyperuricemia.
- Type II (Pompe): Lysosomal α-1,4-glucosidase def. → Cardiomegaly, muscle weakness. 📌 Pompe trashes the Pump (heart).
- Type III (Cori): Debranching enzyme def. → Milder Type I; normal blood lactate.
- Type V (McArdle): Muscle glycogen phosphorylase def. → Exercise intolerance, muscle cramps, myoglobinuria.
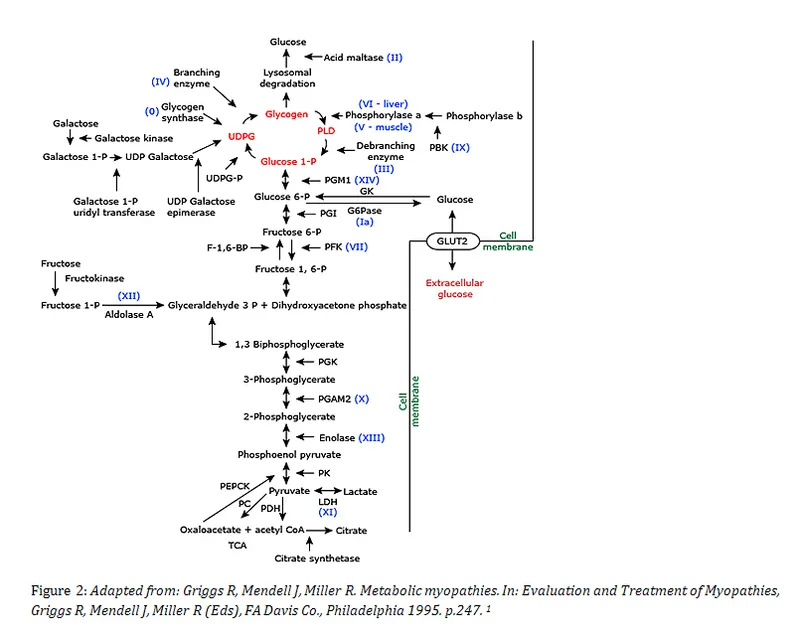
⭐ McArdle Disease (Type V): Patients often report a "second wind" phenomenon during exercise due to ↑ muscle blood flow and utilization of alternative fuels like fatty acids.
High‑Yield Points - ⚡ Biggest Takeaways
- Glycogenolysis (breakdown) is primarily activated by glucagon in the liver and epinephrine in both liver and muscle.
- Glycogenesis (synthesis) is activated by insulin in response to high blood glucose.
- Liver glycogen is the primary source for maintaining blood glucose homeostasis.
- Muscle glycogen serves as an exclusive energy reserve for the muscle itself.
- Glycogen phosphorylase is the rate-limiting enzyme of glycogenolysis; glycogen synthase for glycogenesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

