I-Cell Disease - Address Unknown
- Inheritance: Autosomal Recessive.
- Defect: Failure of Golgi to phosphorylate mannose residues on lysosomal proteins (failure of N-acetylglucosaminyl-1-phosphotransferase).
- Pathophysiology: Lysosomal enzymes are secreted extracellularly instead of being delivered to the lysosome. This leads to the accumulation of cellular debris (inclusions) inside the cell.
- Clinical: Presents in infancy with coarse facial features, clouded corneas, restricted joint movement, and skeletal abnormalities.
⭐ Diagnosis: High levels of lysosomal enzymes in the plasma, while intracellular levels are low.
📌 Mnemonic: I-C-E-L-L → Inclusion Cells, Enzymes Loose in Lymph.
Transport Defects - Cellular Gridlock
-
I-Cell Disease (Mucolipidosis II)
- Pathophysiology: Autosomal recessive defect in N-acetylglucosaminyl-1-phosphotransferase. This prevents the phosphorylation of mannose residues to mannose-6-phosphate (M6P) on lysosomal hydrolases.
- Result: Enzymes are secreted extracellularly instead of being delivered to lysosomes. Substrates accumulate within lysosomes, forming characteristic inclusion cells.
- Features: Presents in infancy with coarse facial features, gingival hyperplasia, clouded corneas, skeletal abnormalities (dysostosis multiplex), and severe psychomotor delay.
- 📌 Mnemonic: I-CELL = Inclusions in Cytoplasm, Enzymes Lost from Lysosome.
-
Cystinosis
- Pathophysiology: Defect in the lysosomal cystine transporter, cystinosin (CTNS gene).
- Result: Accumulation and crystallization of cystine within lysosomes.
- Features: Leads to renal tubular Fanconi syndrome, photophobia (corneal cystine crystals), and progressive renal failure.
⭐ In I-cell disease, the hydrolase enzymes themselves are functional, but are secreted into the plasma. This leads to high plasma levels of lysosomal enzymes, a key diagnostic finding.

Niemann-Pick Type C - Cholesterol Jam
- Pathophysiology: Autosomal recessive disorder from mutations in NPC1 (95%) or NPC2 genes, disrupting cholesterol transport out of lysosomes.
- Mechanism: Leads to intracellular accumulation of unesterified cholesterol and glycosphingolipids, creating a cellular "traffic jam."
- Clinical Triad:
- Neurologic: Progressive ataxia, dystonia, and cognitive decline. Vertical supranuclear gaze palsy (VSGP) is a hallmark sign.
- Visceral: Hepatosplenomegaly, often presenting with prolonged neonatal jaundice.
- Psychiatric: Early-onset psychosis or behavioral issues in adult forms.
- Diagnosis:
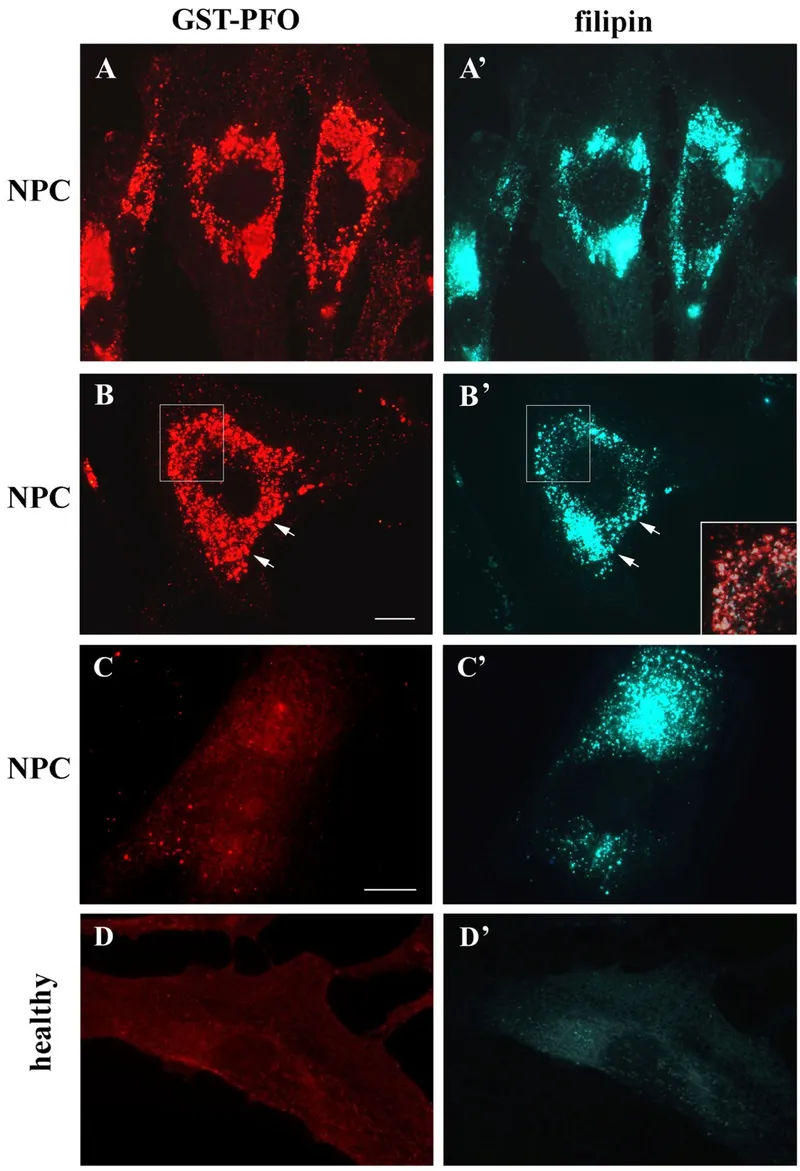
- Biochemical: Filipin stain on cultured fibroblasts shows characteristic perinuclear cholesterol accumulation.
- Biomarkers: Elevated plasma oxysterols (e.g., cholestane-3β, 5α, 6β-triol).
- Genetic: Definitive diagnosis via NPC1/NPC2 gene sequencing.
⭐ Exam Favorite: Vertical supranuclear gaze palsy (difficulty with voluntary up-and-down eye movements) is the most specific early neurological sign.
High‑Yield Points - ⚡ Biggest Takeaways
- I-cell disease results from a defective N-acetylglucosaminyl-1-phosphotransferase, leading to failure of mannose-6-phosphate tagging.
- Lysosomal enzymes are subsequently secreted extracellularly, causing high plasma levels.
- Key features include coarse facial features, dysostosis multiplex, and clouded corneas.
- Cystinosis is a defect in the CTNS gene (cystinosin), causing cystine crystal accumulation.
- Salla disease and ISSD involve defects in the sialic acid transporter, sialin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

