Pathophysiology - The Energy Choke
- Genetic Defect: Autosomal recessive deficiency of the muscle (M) subunit of Phosphofructokinase-1 (PFK-1).
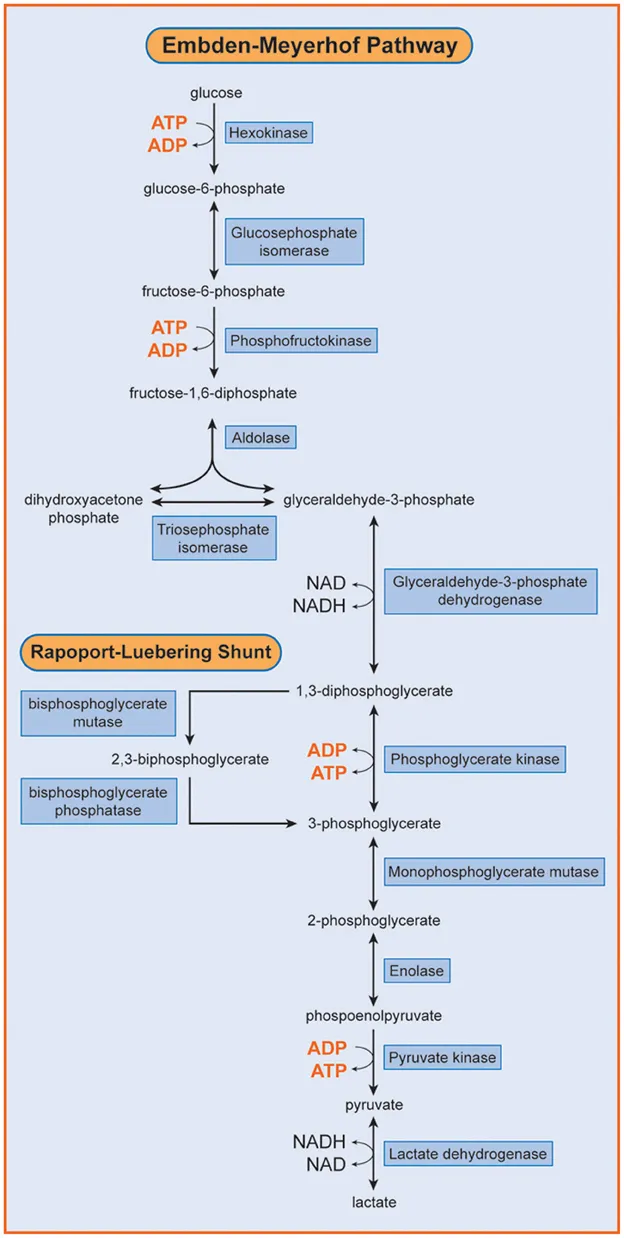
- Metabolic Block: PFK-1 is a rate-limiting enzyme in glycolysis. Its absence halts the conversion of fructose-6-phosphate to fructose-1,6-bisphosphate, choking cellular energy production.
- Consequences:
- ↓ ATP in Muscle: Impairs energy supply during anaerobic exercise, causing premature fatigue, pain, and cramps.
- Paradoxical Effect: Glucose infusion worsens symptoms by increasing upstream substrates ($Glucose-6-P$, $Fructose-6-P$), intensifying the metabolic traffic jam.
⭐ A hallmark finding is a flat venous lactate curve with exercise, as glycolysis cannot proceed to produce pyruvate and subsequently lactate.
Clinical Presentation - Pain, No Gain
- Exercise Intolerance & Myalgia: Manifests as premature fatigue and painful muscle cramps, typically triggered by brief, strenuous activities like sprinting. Onset is in childhood or adolescence, not infancy.
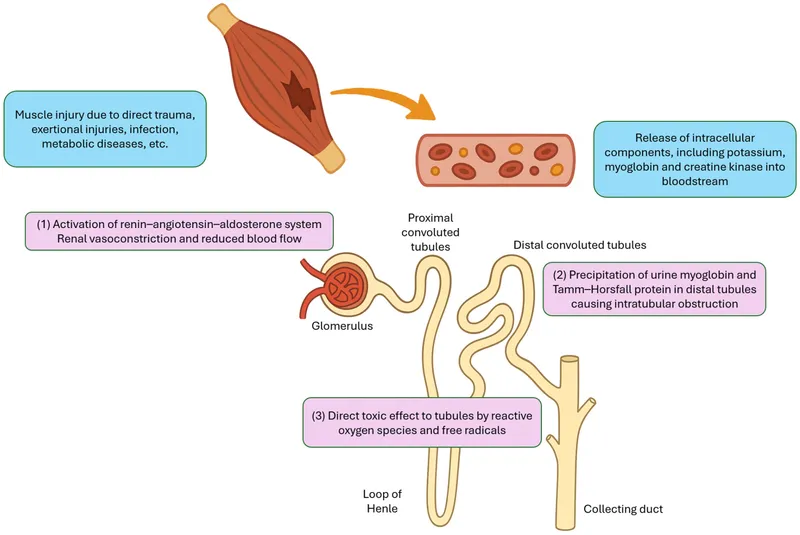
- Rhabdomyolysis & Myoglobinuria: Strenuous exercise can induce muscle breakdown (rhabdomyolysis), leading to dark, reddish-brown urine.
- Key Associated Findings:
- Compensated Hemolytic Anemia: RBCs also have PFK deficiency, leading to non-spherocytic hemolysis and sometimes jaundice.
- Hyperuricemia: Caused by increased nucleotide degradation in muscle during exercise.
⭐ Absence of "Second Wind": Unlike McArdle disease, patients do not experience a "second wind" (improvement in symptoms with continued aerobic activity), as both glycogenolysis and glycolysis are blocked.
Diagnosis - The Lactate Flatline
- Lab Findings:
- ↑ Serum Creatine Kinase (CK), which spikes dramatically with exercise.
- Hyperuricemia.
- Signs of hemolysis: ↑ reticulocytes, ↑ unconjugated bilirubin.
- Ischemic Forearm Exercise Test:
- Key finding: A flat or absent rise in venous lactate post-exercise.
- Ammonia levels, in contrast, show a normal or exaggerated rise.
- Muscle Biopsy:
- Histology: Reveals glycogen accumulation, staining positive with PAS.
- Definitive diagnosis: Assay shows deficient PFK-1 enzyme activity.
- Genetic Testing:
- Identifies mutations in the PFKM gene.
⭐ High-Yield: Tarui disease is unique among GSDs for its dual presentation of metabolic myopathy and compensated hemolysis, as the PFK enzyme is deficient in both muscle and red blood cells.
Management - Fueling Carefully
- Primary Strategy: Strict avoidance of triggers like intense exercise and high-carbohydrate meals, particularly before physical activity.
- Dietary Therapy: A ketogenic (high-fat, protein-rich) diet can supply alternative muscle fuel (ketones, fatty acids), bypassing the enzymatic block.
- Symptomatic Care: Manage myoglobinuria with vigorous hydration and urine alkalinization to prevent renal failure.
- Genetic Counseling: Advised for patients and families.
⭐ A pre-exercise glucose load paradoxically worsens exercise tolerance by inhibiting lipolysis and ketogenesis, the muscle's only alternative energy pathways.
High‑Yield Points - ⚡ Biggest Takeaways
- Enzyme deficiency: Muscle Phosphofructokinase-1 (PFK-1), which impairs glycolysis.
- Classic presentation: Exercise intolerance, painful muscle cramps, and myoglobinuria upon strenuous activity.
- Key diagnostic finding: No rise in blood lactate levels after an ischemic exercise test.
- Associated condition: Mild, compensated hemolytic anemia is often present, as RBCs are also affected.
- Inheritance pattern: Autosomal recessive.
- Metabolic block: Leads to accumulation of G6P and F6P.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

