Pathophysiology - Lysosome's Sugar Jam
- Enzyme Defect: Deficiency of lysosomal acid α-glucosidase (GAA), also known as acid maltase.
- This enzyme is crucial for breaking down glycogen within the lysosome.
- Cellular Pathology: Without GAA, glycogen progressively accumulates inside lysosomes, causing them to swell.
- Engorged lysosomes disrupt cellular architecture and function, leading to cell death.
- Primarily affects high-metabolism tissues: cardiac, skeletal, and smooth muscle.
- Result: Progressive muscle damage and organ dysfunction.
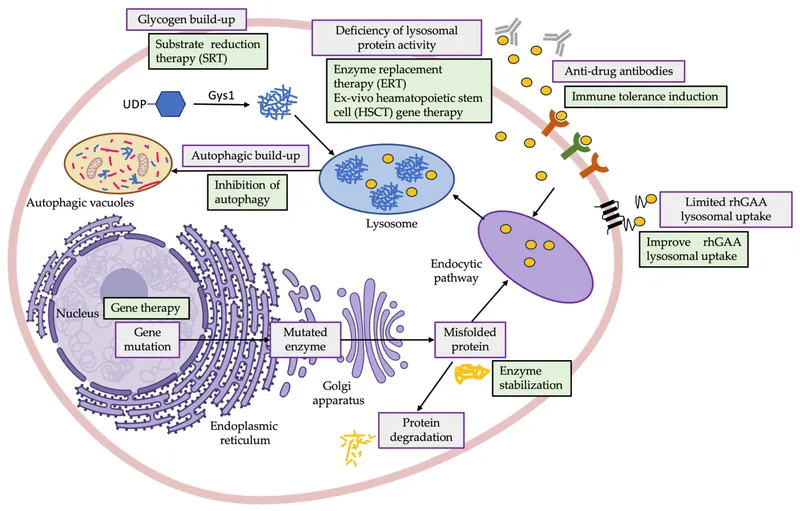
⭐ Unlike other GSDs, Pompe disease is a lysosomal storage disease. Blood glucose levels are typically normal as cytosolic glycogen metabolism is unaffected.
Clinical Presentation - The Floppy Baby Saga
- Infantile-Onset (Classic): Presents within the first few months of life.
- Profound Hypotonia & Muscle Weakness: The hallmark "floppy baby." Generalized weakness, head lag, and inability to meet motor milestones.
- Cardiomyopathy: Massive cardiomegaly, almost always hypertrophic, is characteristic.
- Feeding & Breathing: Poor feeding leads to failure to thrive. Respiratory distress from diaphragm weakness.
- Other Signs: Macroglossia (enlarged tongue) and mild hepatomegaly.
- Late-Onset (Juvenile/Adult): Milder, progressive proximal muscle weakness, often mimicking muscular dystrophies. Spares the heart initially.
📌 Mnemonic: Pompe hurts the Pump (heart), Oesophagus (feeding), Muscles, and Pulmonary system.
⭐ Exam Favorite: The combination of profound hypotonia and massive cardiomegaly on chest X-ray is virtually pathognomonic for infantile-onset Pompe disease.
Diagnosis - Spotting Sugar Buildup
- Screening: Dried blood spot (DBS) test for ↓ acid alpha-glucosidase (GAA) enzyme activity.
- Confirmatory Testing:
- Definitive GAA enzyme assay in fibroblasts or leukocytes.
- GAA gene sequencing to identify mutations.
- Supportive Labs:
- ↑ Serum Creatine Kinase (CK), AST, ALT.
- ↑ Urinary glucose tetrasaccharides ($Glc_4$).
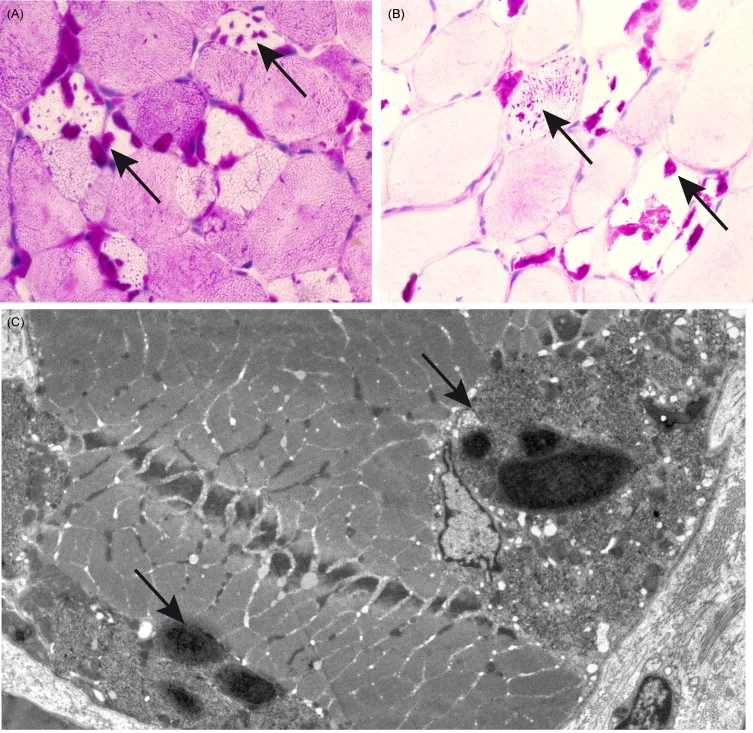
⭐ Muscle biopsy, though less common now, classically shows lysosomes filled with periodic acid-Schiff (PAS)-positive material that is resistant to diastase digestion.
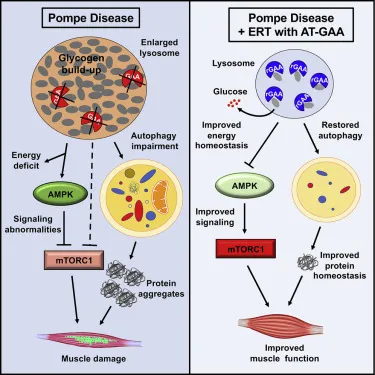
Management - Enzyme Power-Up
- Enzyme Replacement Therapy (ERT): Cornerstone of treatment.
- Drug: Alglucosidase alfa (Myozyme®, Lumizyme®), a recombinant human acid α-glucosidase (rhGAA).
- Mechanism: IV infusion replaces the deficient enzyme, reducing glycogen accumulation in lysosomes, particularly in skeletal and cardiac muscle.
- Goal: Improve muscle function, reduce ventilator dependence, and enhance survival.
⭐ ERT significantly improves cardiomyopathy and motor outcomes, but immune reactions (infusion-associated reactions) can occur. Antibody formation against the replacement enzyme may limit efficacy.
- Supportive Care: Multidisciplinary approach is crucial.
- Respiratory: Non-invasive ventilation (BiPAP) or mechanical ventilation.
- Nutrition: Caloric support, feeding tube if needed.
- Rehabilitation: Physical, occupational, and speech therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- The only lysosomal storage disease among glycogen storage disorders, due to deficient lysosomal α-1,4-glucosidase (acid maltase).
- Autosomal recessive inheritance.
- Classic infantile form presents with profound hypotonia, massive cardiomegaly, and macroglossia, leading to death by age 2.
- Unlike other GSDs, it does not cause hypoglycemia; blood glucose levels are normal.
- Adult-onset form mimics muscular dystrophy, primarily affecting skeletal muscles.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

