Wound Stasis - The Healing Stalemate
- Prolonged Inflammatory Phase: The wound is trapped, unable to progress to proliferation.
- Cellular Dysfunction: Persistent neutrophils & pro-inflammatory (M1) macrophages release damaging reactive oxygen species (ROS) and proteases.
- Senescent Fibroblasts: Poor response to growth factors, leading to ↓ collagen deposition.
- Proteolytic Environment: An imbalance of ↑ Matrix Metalloproteinases (MMPs) and ↓ Tissue Inhibitors of Metalloproteinases (TIMPs) degrades the extracellular matrix (ECM).
- Biofilm Presence: Microbial colonies shield bacteria from immune cells and antibiotics, perpetuating inflammation.
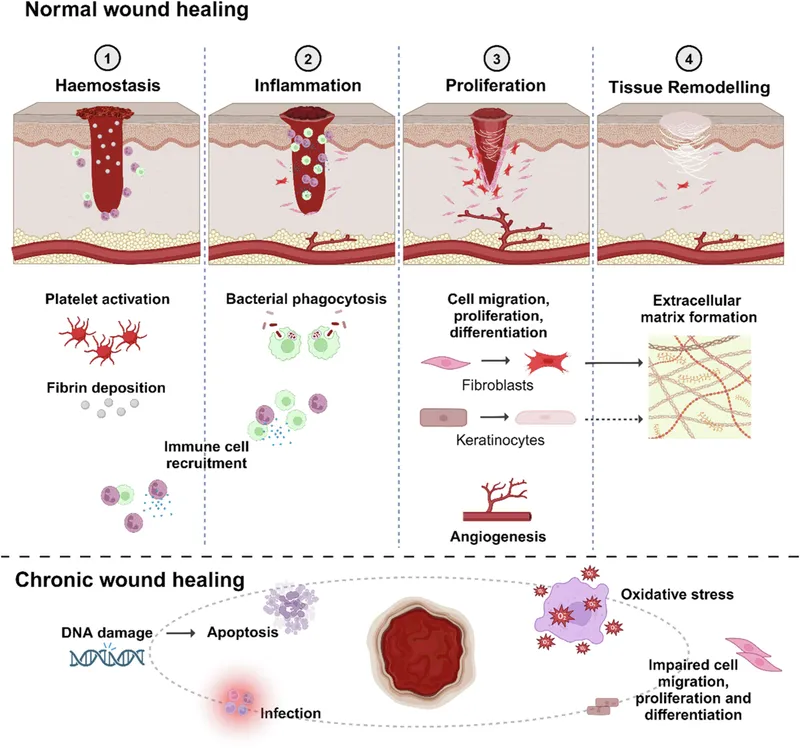
⭐ The key pathological feature is an elevated MMP:TIMP ratio, which actively degrades newly formed granulation tissue and growth factors, preventing effective healing.
Vicious Cycles - Pathophysiology Deep Dive
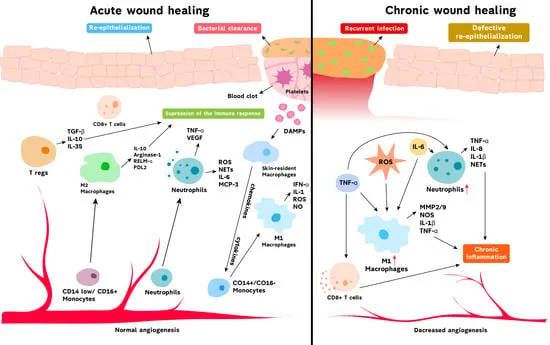
- Stalled Inflammation: The healing cascade is arrested in a chronic inflammatory state, dominated by neutrophils.
- Protease Overload:
- Persistent neutrophils release excessive Matrix Metalloproteinases (MMPs) and elastase.
- This overwhelms the natural Tissue Inhibitors of Metalloproteinases (TIMPs).
- Destructive Microenvironment:
- High MMP levels degrade the extracellular matrix (ECM), growth factors (GFs), and their receptors.
- This prevents cell migration and the formation of a stable scaffold for new tissue.
- Cellular Dysfunction: Fibroblasts become senescent-metabolically active but non-proliferative and unresponsive to GFs.
- Biofilm Formation: Chronic wounds are often colonized by bacteria in biofilms, which perpetuate inflammation and resist host defenses.
⭐ In chronic wounds, the ratio of MMPs to TIMPs is significantly elevated, leading to uncontrolled matrix destruction and preventing the transition to the proliferative phase of healing.
The Big Four - Ulcer Personalities
| Feature | Venous Stasis Ulcer | Arterial (Ischemic) Ulcer | Diabetic (Neuropathic) Ulcer | Pressure Ulcer (Decubitus) |
|---|---|---|---|---|
| Location | Medial malleolus (Gaiter area) | Tips of toes, pressure points | Plantar foot, metatarsal heads | Sacrum, heels, ischium, trochanter |
| Appearance | Large, shallow, irregular border, heavy exudate, hemosiderin staining | "Punched-out," pale/necrotic base, minimal exudate, shiny skin, hair loss | Calloused rim, deep, painless, often infected | Staged (I-IV), can have undermining/tunneling |
| Pain | Aching, relieved by elevation | Severe, worse with elevation | Typically painless | Painful if sensation intact |
| Pathophys | Venous hypertension, valve incompetence | Peripheral Artery Disease (PAD), ↓ arterial inflow | Peripheral neuropathy, pressure, microangiopathy | Unrelieved pressure > capillary filling pressure |
⭐ An Ankle-Brachial Index (ABI) < 0.9 is diagnostic for PAD, the cause of arterial ulcers. Values < 0.4 indicate critical limb ischemia. Compression therapy, key for venous ulcers, is contraindicated.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic wounds are trapped in a prolonged inflammatory phase, preventing progression to proliferation.
- Cellular senescence of fibroblasts leads to ↓ collagen deposition and impaired matrix formation.
- Persistent bacterial biofilms create a pro-inflammatory microenvironment and resist host defenses.
- Local tissue ischemia and hypoxia are central, starving the wound of oxygen and nutrients.
- An imbalance with ↑ Matrix Metalloproteinases (MMPs) excessively degrades the extracellular matrix.
- Underlying systemic diseases like diabetes mellitus and vascular insufficiency are major drivers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

